The Human Form Of Mad Cow Disease
As a geriatric psychiatrist, I recognized that Marjories symptoms warranted careful evaluation. Even though she was only in her late 50s, very young for the onset of a dementia, her problem seemed unlike a routine case of depression. Her memory difficulty and her trouble carrying out tasks that had been simple a few months earlier suggested a neurocognitive problem such as delirium or dementia. The careful work of a local neurologist to whom I referred Marjorie led to a sad discovery. Marjorie was suffering from Creutzfeldt-Jakob disease, an infection of the brain that produces rapidly progressive dementia. Creutzfeldt-Jakob disease is a transmissible spongiform encephalopathy, sometimes called the human form of mad cow disease, and is caused by microscopic particles called prions, which are simple and potentially devastating proteins that cause certain host proteins to undergo a destructive change in shape. Although no curative treatment is available for this disorder, recognition of the diagnosis allowed Marjories family to prepare for her death and to ease her final weeks of suffering by providing a palliative and loving environment.
Tips For Family Members
What should a patient, or a patients family, do to make sure that infections are not overlooked in someone with suspected Alzheimers disease or another dementia? First and foremost, make sure to express your concern to the clinicians who are caring for someone with an altered mental state. Also, it is crucial to ensure that the patients history is known by his or her health care providers. This is especially important if the cognitive changes are recent, or developed rapidly, or were associated with a known medical illness or known exposure to an infectious disease. Identifying an infection can require special tests of blood or cerebrospinal fluid that are not routinely ordered in many treatment settings. Awareness of a disease history or of an exposure may lead to further assessment and earlier identification of an infection even when typical medical symptoms such as fever, cough, or pain with urination are subtle or absent.
Dementia With Lewy Bodies
| Other names | Diffuse Lewy body disease, dementia due to Lewy body disease |
|---|---|
| Microscopic image of a Lewy body in a neuron of the substantia nigra scale bar=20 microns | |
| After the age of 50, median 76 | |
| Duration | |
| Average survival 8 years from diagnosis | |
| Frequency | About 0.4% of persons older than 65 |
Dementia with Lewy bodies is a type of dementia characterized by changes in sleep, behavior, cognition, movement, and regulation of automatic bodily functions. Memory loss is not always an early symptom. The disease worsens over time and is usually diagnosed when cognitive decline interferes with normal daily functioning. Together with Parkinson’s disease dementia, DLB is one of the two Lewy body dementias. It is a common form of dementia, but the prevalence is not known accurately and many diagnoses are missed. The disease was first described by Kenji Kosaka in 1976.
You May Like: Senile Vs Dementia
Treatment And Care For Lewy Body Dementia
While LBD currently cannot be prevented or cured, some symptoms may respond to treatment for a period of time. An LBD treatment plan may involve medications, physical and other types of therapy, and counseling. A plan to make any home safety updates and identify any equipment can make everyday tasks easier.
A skilled care team often can suggest ways to improve quality of life for both people with LBD and their caregivers.
What Is Lewy Body Dementia Causes Symptoms And Treatments
On this page:
Lewy body dementia is a disease associated with abnormal deposits of a protein called alpha-synuclein in the brain. These deposits, called Lewy bodies, affect chemicals in the brain whose changes, in turn, can lead to problems with thinking, movement, behavior, and mood. Lewy body dementia is one of the most common causes of dementia.
LBD affects more than 1 million individuals in the United States. People typically show symptoms at age 50 or older, although sometimes younger people have LBD. LBD appears to affect slightly more men than women.
Diagnosing LBD can be challenging. Early LBD symptoms are often confused with similar symptoms found in other brain diseases or in psychiatric disorders. Lewy body dementia can occur alone or along with other brain disorders.
It is a progressive disease, meaning symptoms start slowly and worsen over time. The disease lasts an average of five to eight years from the time of diagnosis to death, but can range from two to 20 years for some people. How quickly symptoms develop and change varies greatly from person to person, depending on overall health, age, and severity of symptoms.
In the early stages of LBD, symptoms can be mild, and people can function fairly normally. As the disease advances, people with LBD require more help due to a decline in thinking and movement abilities. In the later stages of the disease, they often depend entirely on others for assistance and care.
You May Like: Does Prevagen Work For Dementia
Types Of Lewy Body Dementia And Diagnosis
LBD refers to either of two related diagnoses dementia with Lewy bodies and Parkinson’s disease dementia. Both diagnoses have the same underlying changes in the brain and, over time, people with either diagnosis develop similar symptoms. The difference lies largely in the timing of cognitive and movement symptoms.
In DLB, cognitive symptoms develop within a year of movement symptoms. People with DLB have a decline in thinking ability that may look somewhat like Alzheimer’s disease. But over time, they also develop movement and other distinctive symptoms of LBD.
In Parkinson’s disease dementia, cognitive symptoms develop more than a year after the onset of movement symptoms . Parkinson’s disease dementia starts as a movement disorder, with symptoms such as slowed movement, muscle stiffness, tremor, and a shuffling walk. These symptoms are consistent with a diagnosis of Parkinson’s disease. Later on, cognitive symptoms of dementia and changes in mood and behavior may arise.
Not all people with Parkinson’s disease develop dementia, and it is difficult to predict who will. Many older people with Parkinson’s develop some degree of dementia.
Caregivers may be reluctant to talk about a person’s symptoms when that person is present. Ask to speak with the doctor privately if necessary. The more information a doctor has, the more accurate a diagnosis can be.
Managing Sleep Disorders In Lewy Body Dementia
Sleep problems may increase confusion and behavioral problems in people with LBD and add to a caregiver’s burden. A physician can order a sleep study to identify any underlying sleep disorders such as sleep apnea, restless leg syndrome, and REM sleep behavior disorder.
REM sleep behavior disorder, a common LBD symptom, involves acting out one’s dreams, leading to lost sleep and even injuries to individuals and their sleep partners. Clonazepam, a drug used to control seizures and relieve panic attacks, is often effective for the disorder at very low dosages. However, it can have side effects such as dizziness, unsteadiness, and problems with thinking. Melatonin, a naturally occurring hormone used to treat insomnia, may also offer some benefit when taken alone or with clonazepam.
Excessive daytime sleepiness is also common in LBD. If it is severe, a sleep specialist may prescribe a stimulant to help the person stay awake during the day.
Some people with LBD have difficulty falling asleep. If trouble sleeping at night persists, a physician may recommend a prescription medication. It is important to note that treating insomnia and other sleep problems in people with LBD has not been extensively studied, and that treatments may worsen daytime sleepiness and should be used with caution. Sleep problems can also be addressed by avoiding lengthy naps, increasing daytime exercise, and avoiding caffeine, alcohol, and chocolate late in the day.
Also Check: Dementia Color Ribbon
Memory Loss & Dementia
Degenerative thinking abilities or severe memory loss marked eventually set in and affect a persons ability to perform their normal daily activities.
Memory loss is a primary Lewy body dementia symptom and its marked by forgetfulness, misidentifying objects, challenges multitasking, reasoning and problem-solving.
Confusion is yet another symptom that accompanies dementia and the person may suddenly have difficulties making sense of time and place.
However, unlike with Alzheimers dementia, the memory problems do not manifest at first but they start becoming apparent as LBD progresses.
Dementia can also alter mood and behavior leading the person to start displaying loss of initiative or poor judgment.
Genetic Study Of Lewy Body Dementia Supports Ties To Alzheimers And Parkinsons Diseases
NIH-led study locates five genes that may play a critical role in Lewy body dementia.
In a study led by National Institutes of Health researchers, scientists found that five genes may play a critical role in determining whether a person will suffer from Lewy body dementia, a devastating disorder that riddles the brain with clumps of abnormal protein deposits called Lewy bodies. Lewy bodies are also a hallmark of Parkinsons disease. The results, published in Nature Genetics, not only supported the diseases ties to Parkinsons disease but also suggested that people who have Lewy body dementia may share similar genetic profiles to those who have Alzheimers disease.
Lewy body dementia is a devastating brain disorder for which we have no effective treatments. Patients often appear to suffer the worst of both Alzheimers and Parkinsons diseases. Our results support the idea that this may be because Lewy body dementia is caused by a spectrum of problems that can be seen in both disorders, said Sonja Scholz, M.D., Ph.D., investigator at the NIHs National Institute of Neurological Disorders and Stroke and the senior author of the study. We hope that these results will act as a blueprint for understanding the disease and developing new treatments.
The study was led by Dr. Scholzs team and researchers in the lab of Bryan J. Traynor, M.D., Ph.D., senior investigator at the NIHs National Institute on Aging .
Article:
NIHTurning Discovery Into Health®
Don’t Miss: What Color Ribbon Is Alzheimer’s
Specificity Of Lewy Bodies For Parkinson’s Disease
Although Lewy bodies are highly characteristic, they are not pathognomonic for Parkinson’s disease. They have been found in 46 percent of routine autopsies17,39, but their occurrence below the age of 60 years is unusual. These incidental cases may represent early undiagnosed, or preclinical parkinsonism. Yahr’s observations on the frequently subtle and elusive early symptomatology in Parkinson’s disease58 is consistent with this interpretation. An example of Lewy body formation , antedating the onset of parkinsonism, was reported by Stadlan et al.51. The rare occurrence of Lewy bodies in postencephalitic parkinsonism8,39 can be explained by the presence of both postencephalitic and idiopathic parkinsonism in the same patient. Such a coincidence cannot be claimed for a few other conditions where Lewy bodies have been described23, for example for Hallervorden-Spatz disease7.
Can Mad Cow Disease Be Prevented Or Avoided
Mad cow disease is extremely rare in the United States. Most cases have occurred in Europe, especially in the United Kingdom.
U.S. government agencies have taken many steps to keep food in the United States safe. The Food and Drug Administration and the U.S. Department of Agriculture regulate animal feed to keep cows safe from BSE. They also prevent high-risk cows and cow products from entering the country from other countries. These and other steps have worked very well to keep mad cow disease out of the United States.
If you live in the United States, you dont need to do anything to avoid mad cow disease. If you are traveling to another country, the best way to reduce your risk is to avoid eating beef.
Mad cow disease isnt contagious. It cant be transmitted by being around someone who has the disease. So practices like good hygiene or handwashing dont prevent it.
You May Like: What Color Ribbon Is Alzheimer’s
What Can I Expect If I Or My Loved One Have A Diagnosis Of Lewy Body Dementia
Each persons experience with Lewy body dementia is unique to them. How slowly or quickly the disease progresses is impossible to know, but may be influenced by your general health and any existing diseases you may have. Because LBD is a progressive disease, difficulties with mind and body functions get worse over time. Currently, there is no known way to stop the progression of the disease. After diagnosis, most people with LBD live between five and seven years. Some people with LBD live up to 20 years after their diagnosis.
However, theres always hope. Research on LBD, dementia with lewy bodies, Alzheimers disease, Parkinsons disease with dementia are ongoing. New medications are being developed and new approaches to treatment are being investigated.
Can You Prevent Lewy Body Dementia
If you have a family history of Lewy body dementia or Parkinson’s disease, it’s understandable to be concerned about developing Lewy body dementia. Like other types of dementia, there’s not a guaranteed way to completely prevent Lewy body dementia. However, understanding the factors that increase the risk helps us identify opposing strategies that can decrease this likelihood, and these strategies are generally connected with better physical health, as well.
Read Also: What Color Ribbon Is Alzheimer’s
Hallucinations Or Delusions Of Reality
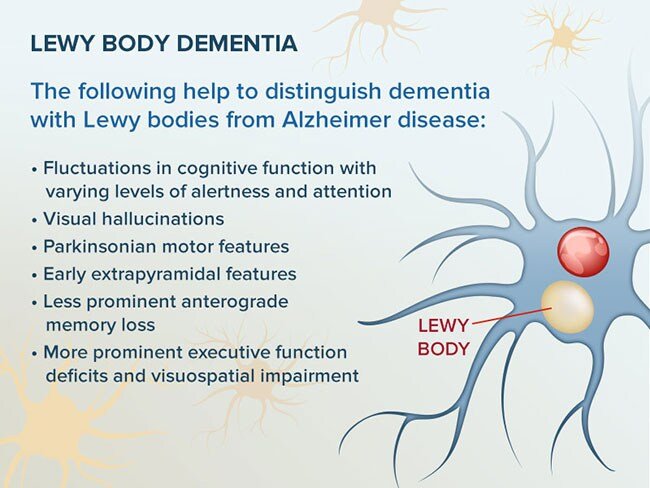
Unlike Alzheimers disease, individuals in the early stages of Lewy Body Dementia may exhibit cognitive changes such as hallucinations or distortions of reality. In general, hallucinations caused by LBD are vivid and usually visual, rather than auditory. LBD differs from other forms of dementia in that most early-stage cases do not involve memory loss.
The Effect Of Dementia On Sepsis Survival
Not a lot of research has been done yet on patients with dementia and their outcomes following sepsis. A study published in 2015 looked at patients with COPD who also had dementia. The researchers found that patients in this group had a higher risk of dying than patients with COPD who did not have dementia.
Recommended Reading: What Color Ribbon Is Alzheimer’s
Treating Movement Symptoms In Lewy Body Dementia
LBD-related movement symptoms may be treated with medications used for Parkinson’s disease, called carbidopa-levodopa. These drugs can help make it easier to walk, get out of bed, and move around. However, they cannot stop or reverse the disease itself. Side effects of this medication can include hallucinations and other psychiatric or behavioral problems. Because of this risk, physicians may recommend not treating mild movement symptoms with medication. Other Parkinson’s medications are less commonly used in people with LBD due to a higher frequency of side effects.
People with LBD may benefit from physical therapy and exercise. Talk with your doctor about what physical activities are best.
Cold Feet And Shuffling Gait
Reviewed on 8/5/2020
There are a few different medical conditions that are strongly associated with:
- Cold Feet
- Shuffling Gait
While the symptoms above can be considered a guide to help associate symptoms common among the conditions below, this is not a substitute for a diagnosis from a health care provider. There are many other medical conditions that also can be associated with your symptoms. Below are the top condition matches for your symptom combination from MedicineNet:
You May Like: What Color Ribbon Is Alzheimer’s
Progression Of Lewy Body Pathology
Lewy body pathology begins in the medulla and olfactory bulbs, spreading progressively through six Braak stages to involve the pons, midbrain, limbic lobe, amygdala and neocortex . Cortical Lewy bodies are similar to those encountered in the brain stem, but do not have a halo and are present even in cases without dementia. Pathological inclusions are also found in the autonomic nervous system, including the enteric nervous system in the gastrointestinal tract.
Spread of Lewy body pathology may reflect selective vulnerability of certain brain regions or could be due to stepwise spread along anatomical pathways. Since the olfactory bulb is affected first, the possibility of a pathogenic virus infection gaining access to the brain via the nasal mucosa has been postulated.
Mariah Lelos, in, 2020
What Caregivers Can Do
Caring for a loved one with dementia is challenging, but watching for signs of infections is important. Since people with dementia may not be able to tell you they are unwell or have pain, it can be hard to detect some types of infections. Here are some tips that may help:
- Signs of a fever or lower than normal temperature. Not everyone with dementia will allow their caregiver to take their temperature. If you cant check for fever that way, watch for other signs, such as the skin is warmer to touch than usual, flushing , lips or skin dryer than usual, or shivering even if it is warm. Dont forget that a lower than normal temperature may also be a sign of sepsis.
- Increasing confusion or agitation, personality change, drowsiness. If there is a significant change in behavior, it could be a sign of an infection. The person may become drowsier, just wanting to sleep. Or someone who is usually calm may become agitated or aggressive.
- Signs of pain or discomfort. If your loved one cant say that something hurts or where theres pain, body language may tell you. Some signs could include: protecting or guarding a part of the body, moaning or grimacing, eating less than usual, increasing restlessness, unwillingness to move, falling or having difficulty balancing, or crying.
- Coughing, wheezing, or shortness of breath. These signs could be caused by pneumonia.
Other things to keep in mind is if your loved one had an invasive procedure or hurt him or herself in some way:
Also Check: Purple Ribbon Alzheimers
Retrospective Study With Humans
In a study followeing up on more than 6,100 people who had been previously injected with human growth hormones, researchers tested those hormones and found that , they contained small amounts of the tau and beta amyloid proteins that are present in the brains of people who have Alzheimer’s. These people have since been monitored to determine if they have developed Alzheimer’s disease. Thus far, none of the participants have developed Alzheimer’s disease, although most are still fairly young for a typical onset of dementia.