Stage : Very Severe Mental Decline/severe Dementia Quality Of Life: Very Severe Impact
Your loved one will not remember any of the past or recognize loved ones. He or she will have likely lost the ability to make healthcare decisions. You will need 24-hour care in the home for day-to-day activities. You may see your loved one:
- Lose the ability to speak, eat or swallow.
- Not be able to use the toilet or get dressed without help.
- Not be able to walk or sit without help.
- Loss of language skills throughout this stage
- Lose all bladder and bowel control.
- Loss of muscle control
Are There Options For Treatment
Today, there is no cure for FTD. Unfortunately, no current treatments slow or stop the progression of the disease. However, if you or a family member or loved one are affected, there are important steps that you can take to preserve and maximize quality of life. A growing number of interventions not limited to medication can help with managing FTD symptoms.
It is important for you and your care partner to identify a team of experts who can help with coordinating care and with the legal, financial, and emotional challenges brought on by this disease.
The Seven Stages Of Dementia
One of the most difficult things to hear about dementia is that, in most cases, dementia is irreversible and incurable. However, with an early diagnosis and proper care, the progression of some forms of dementia can be managed and slowed down. The cognitive decline that accompanies dementia conditions does not happen all at once – the progression of dementia can be divided into seven distinct, identifiable stages.
Learning about the stages of dementia can help with identifying signs and symptoms early on, as well as assisting sufferers and caretakers in knowing what to expect in further stages. The earlier dementia is diagnosed, the sooner treatment can start.
Don’t Miss: Does Medicare Cover Respite Care For Alzheimer’s
How Is Ftd Diagnosed
FTD can be hard to diagnose because the symptoms are similar to those of other conditions. For example, bvFTD is sometimes misdiagnosed as a mood disorder, such as depression. To make matters more confusing, a person can have both FTD and another type of dementia, such as Alzheimer’s disease. Also, because these disorders are rare, physicians may be unfamiliar with the signs and symptoms.
To help diagnose frontotemporal dementia, a doctor may:
- Perform an exam and ask about symptoms
- Look at personal and family medical history
- Use laboratory tests to help rule out other conditions
- Order genetic testing
- Conduct tests to assess memory, thinking, language skills, and physical functioning
- Order imaging of the brain
A psychiatric evaluation can help determine if depression or another mental health condition is causing or contributing to the condition. Only genetic tests in familial cases or a brain autopsy after a person dies can confirm a diagnosis of FTD.
Researchers are studying ways to diagnose FTD earlier and more accurately and to distinguish them from other types of dementia. One area of research involves biomarkers, such as proteins or other substances in the blood or cerebrospinal fluid which can be used to measure disease progression or the effects of treatment. Researchers are also exploring ways to improve brain imaging and neuropsychological testing.
Is There Treatment Available
There is not yet a cure for FTD, or any disease modifying treatment. However, various therapies can help with some of the symptoms. Secondary symptoms, such as depression, may be helped by medication.
Knowing more about FTD and why the person is behaving as they are can help people to cope with the disease.
Family members and carers can, with support, develop coping strategies to work around problems rather than trying to change the behaviour of the person with FTD.
Psychological therapies are important to help manage abnormal behaviour.
Speech therapy is of benefit to people with PNFA, particularly in helping to develop alternative communication methods.
The input of an occupational therapist can help improve everyday functioning at home.
You May Like: Can Prevagen Help Dementia
What Causes Frontotemporal Dementia
Frontotemporal dementia occurs when abnormal proteins build up in the brain. This leads to death of brain cells and deterioration and shrinkage of the frontal and temporal lobes of the brain. Sometimes the disease is genetic, and passed down through families, but in most cases no specific cause can be found.
What Are Specific Care Needs At Each Stage
An individual may not require care assistance after the initial diagnosis of dementia, but that will change as the disease progresses and symptoms become worse. There are about 16 million unpaid caregivers of people with dementia in the United States. While many caregivers are providing daily help for family members, they also hire someone to help. There are many options of care assistance, such as in-home care, adult day care, and nursing home care. There is also financial assistance available.
Early Stage DementiaAs mentioned above, in the early stage of dementia a person can function rather independently and requires little care assistance. Simple reminders of appointments and names of people may be needed. Caregivers can also assist with coping strategies to help loved ones remain as independent as possible, such as writing out a daily to-do list and a schedule for taking medications. Safety should always be considered, and if any tasks cannot be performed safely alone, supervision and assistance should be provided. During this period of dementia, its a good idea for caregivers and loved ones to discuss the future. For example, a long-term care plan should be made and financial and legal matters put in place.
You May Like: Alzheimer’s Paranoia Medication
Outlook For Frontotemporal Dementia
How quickly frontotemporal dementia gets worse varies from person to person and is very difficult to predict.
People with the condition can become socially isolated as the illness progresses. They may not want to spend time in the company of others, or may behave in rude or insulting ways.
Home-based help will usually be needed at some stage, and some people will eventually need care in a nursing home.
The average survival time after symptoms start is around 8 to 10 years. But this is highly variable and some people live much longer than this.
If you or a loved one has been diagnosed with dementia, remember you’re not alone. The NHS and social services, as well as voluntary organisations and specialist support groups, can provide advice and support for you and your family.
Mid Stage Frontotemporal Dementia
As FTD symptoms progress, they tend to become more consistent. In many cases, people living the behavioral variant of frontotemporal dementia will also develop symptoms of the language variants in this stage . Generally, it is difficult for a person to recognize these symptoms on their own usually the people around them are better able to distinguish the behavioral and language changes that develop in the early and mid stages of FTD.
Read Also: How To Change Diaper Of Dementia Patient
Stage : Very Mild Changes No Dementiaquality Of Life: Little To No Impact
You still might not notice any changes in your loved one. Youll see daily memory problems that look like a normal part of aging. You may see:
- Some difficulty finding the right words.
- The ability to make up for memory problems, such as substituting one word for another.
- Normal functioning in the home, community, and workplace.
How You Can Help:
As with Stage 1, start to plan now. Use our tools to help your loved one document his or her values and priorities about the type of care wanted during the various stages of dementia.
You can also watch for new signs that you may not have seen before.
Jade Isnt As Worried About The Possibility Of Developing Ftd As She Is About Mnd Because She Doesnt Feel She Would Be As Aware Of What Was Happening
Dementia doesnt bother me so much because you dont suffer so much physically in the way of your body shutting down and your swallowing and things. You just go a bit nuts. I kind of figure that if that happens, I will be in cuckoo land and it wont matter so much. I said to my husband, Just stick me in a nice little home and only visit me if Im pleased to see you. If Im horrible, then dont even bother because I wont know anything about it. Dont put the kids through it. I mean, having watched my father die, I would never want my children to see anything happen to me, especially like how my father died. So, its made me think, you know, if something happens, just shove me away in a corner and let me die quietly, but if it doesnt, then great. What will be will be. And Id rather have the FTD than the MND, if I get a choice.
Other people had less experience of seeing relatives with FTD, which affected how they felt about it. Lillian hadnt seen the first-hand effects of FTD, so it doesnt quite hold the horrors that motor neurone disease held for me. Lizbeth and Sam did not really think about the possibility of developing FTD, because they hadnt seen relatives with this disease. Lizbeth said, I dont think I could choose which one Id want Id rather not have either.
Also Check: Alzheimer’s And Dementia Ribbon
Support With Later Stage Symptoms
Some of the symptoms that people living with different forms of FTD might develop are outlined below. These symptoms will not apply to everybody. If you would like to talk to somebody about how the issues raised here have affected you, please get in touch.
People with bvFTD may find that behavioural and personality problems progress over time. Other aspects of their thinking may also become affected such as: finding the right word, understanding speech, and memory. However some behaviours such as disinhibition may become less of a problem. The speed of these changes can differ largely between individuals.
As the disease progresses, people will need help with most aspects of daily life. Continence may become a problem and eventually nursing care may become necessary.
In the later stages of bvFTD people may experience issues around eating and swallowing, for example compulsively putting objects in their mouths. Difficulties with swallowing can have serious consequences: people may be at risk of losing weight, of chest infections and pneumonia or of choking on food.
Common problems around eating and swallowing that you may notice:
In general, the beginning of other neurological problems such as difficulties with movement or swallowing tends to bring reduced independence and a need for increased support.
If you would like to talk to somebody about how the issues raised here have affected you, please get in touch.
Living with FTD
Behavioral Variant Frontotemporal Dementia
The most common FTD, bvFTD, involves changes in personality, behavior, and judgment. People with this disorder may have problems with cognition, but their memory may stay relatively intact. Symptoms can include:
- Problems planning and sequencing
- Difficulty prioritizing tasks or activities
- Repeating the same activity or saying the same word over and over
- Acting impulsively or saying or doing inappropriate things without considering how others perceive the behavior
- Becoming disinterested in family or activities they used to care about
Over time, language and/or movement problems may occur, and the person living with bvFTD will need more care and supervision.
Also Check: Does Prevagen Help With Dementia
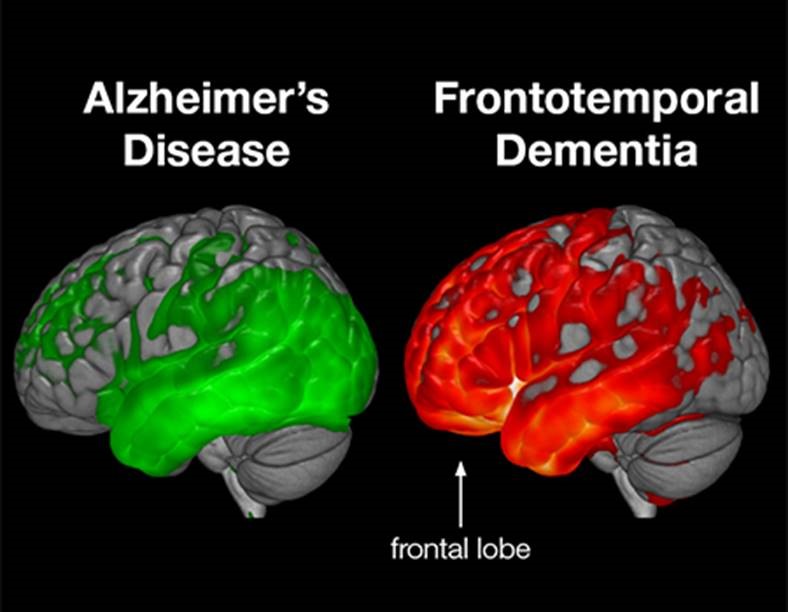
How Ftd And Alzheimer’s Differ
In Alzheimers, the typical initial symptoms are short-term memory impairment and difficulty learning something new. In FTD, the memory usually remains intact initially early symptoms include difficulty with appropriate social interactions and emotions, as well as some language challenges.
FTD and Alzheimers also differ in how the brain is physically affected. FTD mainly affects the brain’s frontal and temporal lobes, whereas Alzheimers affects the temporal lobes in early stages, but with progression impacts most areas of the brain.
FTD also targets younger individuals. The average age of onset for FTD is about 60 years old. While some people have early-onset Alzheimers, the majority of patients are over 65 and many of those are well into their 70s or 80s.
What Is The History Behind Ftd
Dr. Arnold Pick, a German neurologist, discovered Picks disease in 1892. He encountered a patient with distinct symptoms affecting their language, so Pick wanted to dig deeper. This patient is believed to be the first documented case of primary progressive aphasia. Later, he looked at two other patients who were experiencing behavioral changes, decreased cognitive function and language difficulties. Pick determined that dementia can affect certain regions of the brain that cause these particular changes.
Don’t Miss: Senile Vs Dementia
Stage : Severe Mental Decline/moderately Severe Dementiaquality Of Life: Severe Impact
Your loved one will not remember much or any of the past and may not recognize you and other family and friends. He or she may have trouble making healthcare decisions. You may need 24-hour care in the home for day-to-day activities. You may see your loved one:
- Show strong personality changes and mood swings.
- Have delusions, such as thinking it is time to go to work when there is no job.
- Not be able to use the toilet or get dressed without help.
- Getting lost or wandering off.
- Have problems sleeping at night but sleep during the day.
- Lack of awareness of events and experiences.
- Changes in eating habits.
Help the health care team follow your loved ones care preferences. You can:
- Help with dressing, toileting, and other daily activities.
- Continue to try to connect with your loved one. Sometimes connecting in ways other than talking can help, such as listening to music or reading a story.
- Respond with patience.
Stage : Moderately Severe Mental Decline/moderate Dementiaquality Of Life: Moderate Impact
Your loved one will likely remember some of their past and still recognize loved ones. He or she may have trouble making healthcare decisions. You may need some care in the home for day-to-day activities. You may see your loved one:
- Experience personality changes and mood swings.
- Repeat the same questions over and over again.
- Have gaps in memory and become confused about the date, where you are, or your address and phone number.
- Need help with eating or using the toilet.
- Have trouble choosing clothing, such as what kind of close to wear for the season.
- Have bladder problems.
How You Can Help:
If you havent already helped your loved one document his or her care wishes, talk with the health care team and the options for care.
If you have, help the health care team follow your loved ones care preferences.
You can:
- Help with dressing, toileting, and other daily activities.
- Respond to repeated questions with patience.
Recommended Reading: Does Prevagen Help Dementia
Where To Live With Dementia
Eventually, caregiving for someone with dementia wont be appropriate anymore. The needs of a person with progressive dementia become overwhelming, and moving into a full-time residence with trained staff becomes necessary. You should plan for this well before it becomes necessary, by visiting communities and asking the right questions.
Depending on your loved ones stage of illness, different living options are available:
Assisted Living in Early StagesAssisted living residences combine room and board with medical and personal care, and are often sufficient for someone in the early stages of Alzheimers disease or related dementia. Full-time supervision means residents are safe, with living units like private studios or apartments so someone with mild dementia can still feel a sense of independence.
Services offered in assisted living include meals, help with activities of daily living , social activities, and transportation to and from doctors appointments. Before moving in, the residence will assess your loved one to make sure its a good fit.
Memory care residences have physical designs that are appropriate for people with dementia. Someone with Alzheimers, for instance, may become upset when encountering a wall, so memory care buildings have circular hallways. Because people with dementia are prone to wander, memory care residences have increased security and supervision, and special locks on doors.
Did You Know?
Although Her Ftd Means They Cant Have The Conversations They Otherwise Might Have Louisa Sees It As A Blessing That Her Mum Is Able To Continue Enjoying Life
Im more worried about – no, not more – Im as worried about the frontal lobe dementia as I am about the motor neurone disease, because you know, people with motor neurone disease without dementia, I know that theres the physical disability and inability to speak and stuff, I dont know. Like is it better that you understand and hopefully by some method of communication can get your thoughts and feeling across?
I think its a blessing for my mum, you know, I think – I totally like contradict what I say there, dont I – but for my mum, I think, awesome. She doesnt think shes got it until recently and shes plodding on with her life as normal. The only, but the problems are for us because she poses a little bit of a risk to herself when she picks up knives and well, shes fallen over now and broken her wrist so thats something that my dads having to cope with and, well were having to cope with.
But I think at least shes happy just getting on like she would normally, and its probably a bit selfish that I want her to be able to not have that so we can like sit and chat about just stuff, you know, like life, love, that sort of thing, by whatever means would assist her to communicate.
But for myself Im as worried. Wouldnt it be nice like not to actually know anything about it – or not not know anything about it, but like not be quite so tuned in? But thats not, I dont feel like that because I dont want that to, I dont want to have any burden on my family.
You May Like: Alzheimer Disease Life Expectancy After Diagnosis