What Are The Symptoms Of Alzheimers Disease
AD is a type of dementia, a term used to describe a condition that involves memory loss and other cognitive difficulties. There are a number of different types of dementia, howevereach with its own causes and specific symptom profile. AD is just one variation.
The best-recognized sign of mental decline in AD is problems with memory. In the early stages of the disease, this often manifests as difficulties creating new memories, and problems are especially noticeable with , or memories about information and events . Early on, patients are typically able to maintain older memories and non-declarative memories. Over time, however, all memory can be affected, and even the most enduring memories may deteriorate.
But memory deficits are just one aspect of AD symptomatology. Patients can also experience problems with communication, and the ability to read and write may be impaired. Unpredictable mood disturbances, ranging from apathy and depression to angry outbursts, can occur. Thinking often becomes delusional, and a substantial subset of patients even experience visual hallucinations.
Its not just cognition thats affected, though. Movement is hindered, causing patients to begin to lose mobility and have trouble performing even the simplest acts of self-care. Basic motor functions like chewing and swallowing become faulty, and incontinence eventually occurs.
How Is Alzheimers Disease Treated
Alzheimers is complex, and it is therefore unlikely that any one drug or other intervention will successfully treat it in all people living with the disease.
Scientists are exploring many avenues to delay or prevent the disease as well as to treat its symptoms. In ongoing clinical trials, scientists are developing and testing several possible interventions. Under study are drug therapies aimed at a variety of disease interventions, as well as nondrug approaches such as physical activity, diet, cognitive training, and combinations of these. Just as we have many treatments for heart disease and cancer, we will likely need many options for treating Alzheimers. Precision medicine getting the right treatment to the right person at the right time will likely play a major role.
Current approaches to treating Alzheimers focus on helping people maintain mental function, treating the underlying disease process, and managing behavioral symptoms.
How Is Alzheimer’s Different From Other Forms Of Dementia
Alzheimer’s disease is distinguished from other forms of dementia by characteristic changes in the brain that are visible only upon microscopic examination during autopsy. Brains affected by Alzheimer’s disease often show presence of the following:
-
Fiber tangles within nerve cells
-
Clusters of degenerating nerve endings
Another characteristic of Alzheimer’s disease is the reduced production of certain brain chemicals necessary for communication between nerve cells, especially acetylcholine, as well as norepinephrine, serotonin, and somatostatin.
Read Also: Andrea Mitchell Drunk
How The Body Shuts Down
As your body declines it raises the risk for other health problems.
- Infections may develop as your immune system begins to fail.
- Pneumonia can set in, especially if you inhale food or drinks by accident.
- Injuries from falls are more likely to happen.
Most people with Alzheimer’s disease die from pneumonia, another infection, or a heart attack.
It’s best to have conversations early on about how you’d like to be cared for. These conversations can be hard, but having a plan can make it easier for you and your family.
Show Sources
A Coordinated Push For Better Diagnosis And New Treatments
We heard from Dr Jennifer Whitwell from the Mayo Clinic in the US whose research into brain imaging in FTD is identifying new ways to distinguish between the different types of FTD. On average, people with FTD can wait up to five years for an accurate diagnosis, and reports suggest that almost three quarters of people are initially misdiagnosed. So advances in this area are vital for families affected, as well as helping researchers to improve their approach to studying the disease.
Brain imaging is also a central theme in the Genetic Frontotemporal Dementia Initiative , outlined today by Dr Jonathan Rohrer from UCL. This collaborative programme is following hundreds of people whose families are affected by inherited forms of FTD. Using brain scans, the team has already identified particular networks of nerve cells in the brain that are affected differently in FTD caused by different faulty genes.
The study is now entering a second phase with the ultimate aim to map what changes happen in brain, blood and spinal fluid in FTD and when. This will be vital for helping to guide future clinical trials of new treatments in the disease.
As the Alzheimers Research UK Drug Discovery Institutes are kick-starting new drug discovery programmes and a Dementia Consortium drug discovery project already focusing on FTD, its vital these kinds of initiatives run hand-in-hand.
- Weve already funded over £11m into FTD, donate to help us fund more.
Don’t Miss: Quality Of Life Alzheimer’s Disease
Stages Of The Disease
There are three recognized stages of Alzheimer disease: preclinical, mild cognitive impairment , and Alzheimer dementia. For clinical diagnosis the two most relevant stages are MCI and dementia. Recognition of the preclinical stage acknowledges that the Alzheimer disease process begins before symptoms are apparent and anticipates advances in diagnostic testing that may eventually enable diagnosis at the preclinical stage.
MCI often is subdivided into different types, namely amnestic and nonamnestic. One of the first symptoms marking the transition from normal aging to Alzheimer disease is forgetfulness. This transitional stage represents amnestic MCI and is characterized by noticeable dysfunction in memory with retention of normal cognitive ability in judgment, reasoning, and perception. In nonamnestic MCI, impairments in cognitive functions related to attention, perception, and language predominate over deficits in memory. However, as MCI progresses to Alzheimer disease, memory loss becomes more severe, and language, perceptual, and motor skills deteriorate. Mood becomes unstable, and the individual tends to become irritable and more sensitive to stress and may become intermittently angry, anxious, or depressed. Those changes mark the transition to Alzheimer dementia, which in its advanced stages is characterized by unresponsiveness and loss of mobility and control of body functions death ensues after a disease course lasting from 2 to 20 years.
Tangles And Cell Death
In normal brain tissue, a protein called tau stabilizes microtubules. Microtubules are key parts of cell structure.
In a diseased brain, protein strands, or threads, become tangled. As a result, the brain system of transporting cell nutrients along parallel structures which can be compared to railroad tracks falls apart.
Without these critical nutrients, brain cells die.
Memory and thinking depend on the transmission of signals across 100 billion neurons in the brain.
AD interferes with this cell signal transmission. It also affects the activity of brain chemicals called neurotransmitters.
The scrambled chemistry produces flawed signaling, so the brains messages are lost. This impacts the ability to learn, remember, and communicate.
Microglia are a type of cell that initiate immune responses in the brain and spinal cord. When AD is present, microglia interpret the beta-amyloid plaque as cell injury.
The microglia go into overdrive, stimulating inflammation that further damages brain cells.
Some AD research focuses on how this inflammatory response can be reduced or controlled.
Read Also: Alzheimer’s Disease Neurotransmitters
How Can You Help Your Loved One With Alzheimer’s Disease
If you are or will be taking care of a loved one with Alzheimer’s, start learning what you can expect. This can help you make the most of the person’s abilities as they change. And it can help you deal with new problems as they arise.
Work with your loved one to make decisions about the future before the disease gets worse. It’s important to make an advance care plan and name a substitute decision-maker.
Your loved one will need more and more care as the disease gets worse. You may be able to give this care at home. Or you may want to think about using assisted living or a nursing home.
Ask your doctor about local resources such as support groups or other groups that can help as you care for your loved one. You can also search the Internet for online support groups. Help is available.
How Is Alzheimers Disease Diagnosed
Doctors use several methods and tools to help determine whether a person who is having memory problems has Alzheimers disease.
To diagnose Alzheimers, doctors may:
- Ask the person and a family member or friend questions about overall health, use of prescription and over-the-counter medicines, diet, past medical problems, ability to carry out daily activities, and changes in behavior and personality.
- Conduct tests of memory, problem solving, attention, counting, and language.
- Carry out standard medical tests, such as blood and urine tests, to identify other possible causes of the problem.
- Perform brain scans, such as computed tomography , magnetic resonance imaging , or positron emission tomography , to support an Alzheimers diagnosis or to rule out other possible causes for symptoms.
These tests may be repeated to give doctors information about how the persons memory and other cognitive functions are changing over time.
People with memory and thinking concerns should talk to their doctor to find out whether their symptoms are due to Alzheimers or another cause, such as stroke, tumor, Parkinsons disease, sleep disturbances, side effects of medication, an infection, or another type of dementia. Some of these conditions may be treatable and possibly reversible.
In addition, an early diagnosis provides people with more opportunities to participate in clinical trials or other research studies testing possible new treatments for Alzheimers.
Read Also: Alzheimers Awareness Symbol
Do Brain Cells Die As We Age
With normal aging, we dont find that neurons die in massive numbers. While with Alzheimers disease, the neurons or brain cells die in large numbers in certain areas of the brain.
This is the end product of the process of Alzheimers disease. Alzheimers causes neuron death. And this neuron death manifests as memory, thinking, and behavior changes.
But your brain is so resilient that it is able to adapt for many decades to this cell death.
Neuroscientists believe that when the very first signs of memory, thinking or behavior changes appear in an Alzheimers patient, their neuron loss is approximately 70% in certain areas of the brain.
This 70% loss represents a massive number of dead neurons in brain regions that are earliest affected by Alzheimers disease.
It is a truly remarkable process. Your brain is fighting and largely maintaining cognitive skills until you reach some sort of critical point. It is at this juncture, where a very large percentage of neurons are missing from the brain regions critical for memory formation, that Alzheimers becomes evident.
It is one of the most impressive things, that our brain is able to fight this process, and do a pretty good job of fighting for so long.
What causes this cell death? Alzheimers affects two proteins, beta-amyloid and tau. It causes tangle and plaque formation, brain inflammation, lost connections, and neuronal death.
Utility Of Fdg Pet In The Study Of Ad
The Pattern of FDG Hypometabolism Is an Endophenotype of AD
A substantial body of work over many years has identified a FDG-PET endophenotype of AD that is, a characteristic or signature ensemble of limbic and association regions that are typically hypometabolic in clinically established AD patients . The anatomy of the AD signature includes posterior midline cortices of the parietal and posterior cingulate gyri, the inferior parietal lobule, posterolateral portions of the temporal lobe, as well as the hippocampus and medial temporal cortices. Metabolic deficits in AD gradually worsen throughout the course of the disease. Bilateral asymmetry is common at early stages, more advanced disease usually involves prefrontal association areas, and in due course even primary cortices may be affected. Interestingly, the regions initially hypometabolic in AD are anatomically and functionally interconnected and form part of the large-scale distributed brain network known as the default mode network . We now know in addition that these regions are highly vulnerable to amyloid- deposition .
FDG Hypometabolism Is Related to Other AD Biomarkers and to Genes
FDG PET Is a Valid AD Biomarker
Recommended Reading: Alzheimer’s Purple Color Code
What Is Alzheimers Disease
Scientists continue to unravel the complex brain changes involved in the onset and progression of Alzheimers disease. It seems likely that damage to the brain starts a decade or more before memory and other cognitive problems appear. During this preclinical stage of Alzheimers disease, people seem to be symptom-free, but toxic changes are taking place in the brain. Abnormal deposits of proteins form amyloid plaques and tau tangles throughout the brain, and once-healthy neurons stop functioning, lose connections with other neurons, and die.
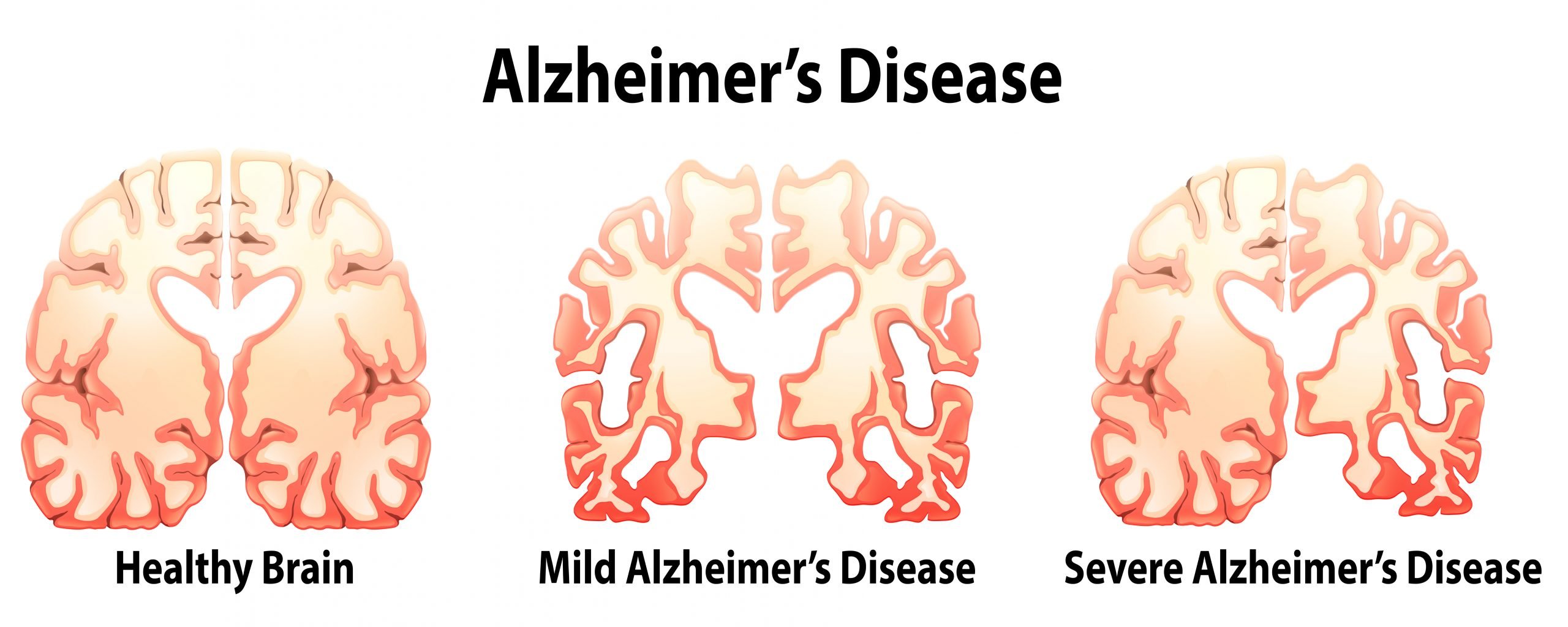
The damage initially appears to take place in the hippocampus, the part of the brain essential in forming memories. As more neurons die, additional parts of the brain are affected, and they begin to shrink. By the final stage of Alzheimers, damage is widespread, and brain tissue has shrunk significantly. Read more about what happens to the brain in Alzheimers »
Utility Of Structural Mri In The Study Of Ad
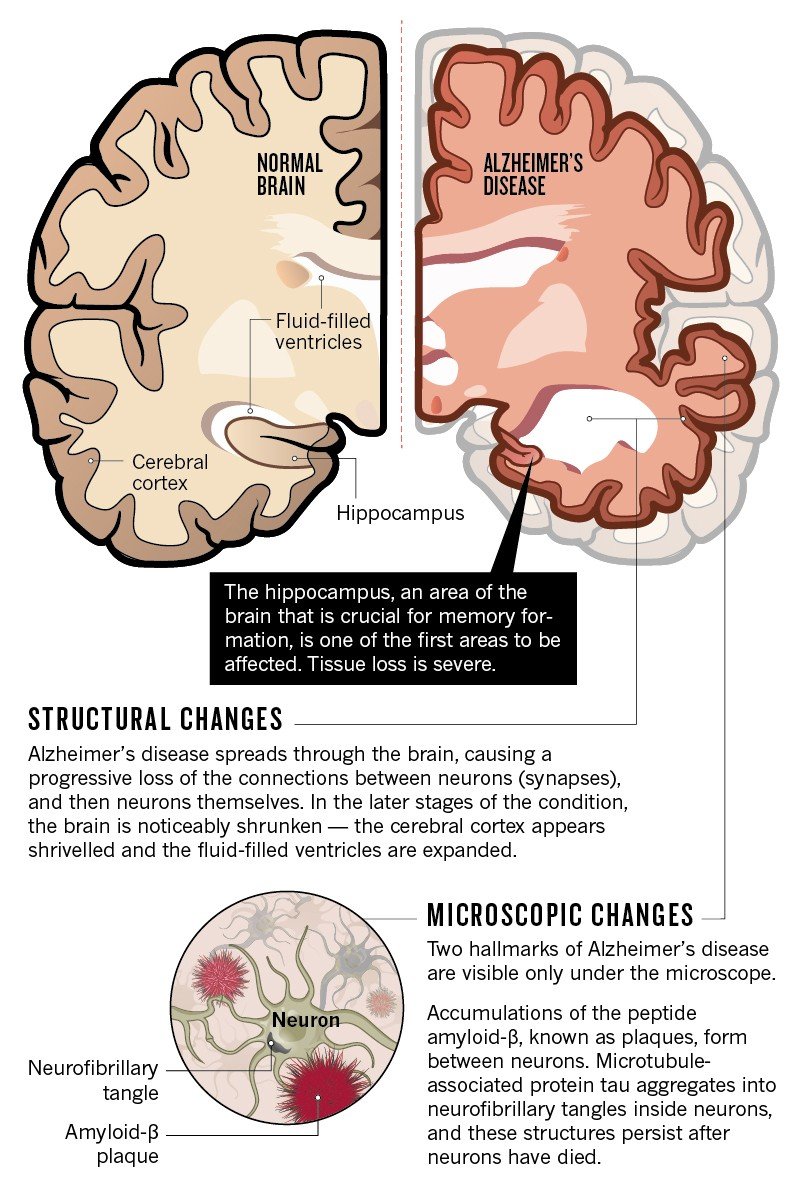
Atrophy in AD
Progressive cerebral atrophy is a characteristic feature of neurodegeneration that can be visualized in life with MRI . The major contributors to atrophy are thought to be dendritic and neuronal losses. Studies of regional MRI volumes have shown these are closely related to neuronal counts at autopsy . The pattern of loss differs between diseases reflecting selective neuronal vulnerability and/or regional disease expression. AD is characterized by an insidious onset and inexorable progression of atrophy that is first manifest in the medial temporal lobe . The entorhinal cortex is typically the earliest site of atrophy, closely followed by the hippocampus, amygdala, and parahippocampus . Other structures within the limbic lobe such as the posterior cingulate are also affected early on. These losses then spread to involve the temporal neocortex and then all neocortical association areas usually in a symmetrical fashion. This sequence of progression of atrophy on MRI most closely fits histopathological studies that have derived stages for the spread of neurofibrillary tangles . Nonetheless, a significant minority of AD cases have atypical presentations and in these cases the pattern of atrophy accords with clinical phenotype: with language presentations particularly having left temporal atrophy and visual variants having posterior cortical atrophy.
Measuring Progression in AD with Structural MRI
Availability and Utility of Structural MRI
Also Check: Neurotransmitters Involved In Alzheimer’s
Medicines For Behavior Problems
Other medicines may be tried to treat anxiety, agitated or hostile behavior, sleep problems, frightening or disruptive false beliefs , suspicion of others , or hallucinations .
Before deciding to use medicine for behavior problems, try to see what is causing the behavior. If you know the cause, you may be able to find better ways of dealing with that behavior. You may be able to avoid treatment with medicine and the side effects and costs that come with it.
Medicines generally are used only for behavior problems when other treatments have failed. They may be needed if:
- A behavior is severely disruptive or harmful to the person or to others.
- Efforts to manage or reduce disruptive behavior by making changes in the person’s environment or routines have failed.
- The behavior is making the situation intolerable for the caregiver.
- The person has trouble telling the difference between what is and is not real . Psychosis means the person has false beliefs or hears or sees things that aren’t there .
What Are Tau Tangles
Tau tangles or neurofibrillary tangles are clumps of a protein called tau and happen inside the neurons, inside brain nerve cells that are important for memory.
Tau protein is abundant in neurons and helps stabilize their axons. Thus, tau is important for normal neuron function.
During Alzheimers disease tau changes and clumps together, like the amyloid beta. But in this case the clumps happen inside the cells.
These clumps are called tangles because the tau protein looks like a helix similar to DNA but its a single helix. And these helices tangle up like a hairball.
Don’t Miss: Color For Dementia Awareness
Basics Of Structural Mri As Applied To Ad
MRI utilizes the fact that protons have angular momentum which is polarized in a magnetic field. This means that a pulse of radiofrequency can alter the energy state of protons and, when the pulse is turned off, the protons will, on returning to their energy stage, emit a radiofrequency signal. By a combination of different gradients and pulses, sequences can be designed to be sensitive to different tissue characteristics. In broad terms structural MRI in AD can be divided into assessing atrophy and changes in tissue characteristics which cause signal alterations on certain sequences such as white matter hyperintensities on T2-weighted MRI as a result of vascular damage. A number of MR sequences that are sensitive to microstructural change have shown alterations in AD. These sequences are already important research tools however, they have not yet found a place in routine clinical practice in AD and they will not be considered further here.
Research On Alzheimers Continues
Alzheimers treatment can help improve the quality of life for people with the disease and slow its progress but the quest for new treatments continues worldwide.
The aim is to develop medications that target the brain changes that Alzheimers causes, but more research funding is needed to achieve that goal.
You can review the Alzheimers Associations Treatment Horizon webpage for more information about treatment of the disease.
What changes have you witnessed in a loved one going through the stages of Alzheimers? What can you tell others to help them cope through these stages? Wed like to hear your stories and suggestions in the comments below.
Related Articles:
Read Also: Does Ben Carson Have Dementia
Medicines For Behaviour Problems
Other medicines may be tried to treat anxiety, agitated or hostile behaviour, sleep problems, frightening or disruptive false beliefs , suspicion of others , or hallucinations .
Before deciding to use medicine for behaviour problems, try to see what is causing the behaviour. If you know the cause, you may be able to find better ways of dealing with that behaviour. You may be able to avoid treatment with medicine and the side effects and costs that come with it.
Medicines generally are used only for behaviour problems when other treatments have failed. They may be needed if:
- A behaviour is severely disruptive or harmful to the person or to others.
- Efforts to manage or reduce disruptive behaviour by making changes in the person’s environment or routines have failed.
- The behaviour is making the situation intolerable for the caregiver.
- The person has trouble telling the difference between what is and is not real . Psychosis means the person has false beliefs or hears or sees things that aren’t there .