The 7 Stages Of Alzheimers Disease
To be suffering from Alzheimers disease is first to present memory loss and disorders that are important enough to impact everyday life even what we call mild Alzheimer.
This does not happen overnight also, it is important to note the frequency and intensity of symptoms or disorders. There is a difference between a small occasional problem and a problem or disorder whose frequency and intensity increase steadily.
Other Causes Of Alzheimers Symptoms
Other conditions can mimic early Alzheimers symptoms, such as:
Central nervous system and other degenerative disorders, including head injuries, brain tumors, stroke, epilepsy, Picks Disease, Parkinsons disease, and Huntingtons disease.
Metabolic ailments, such as hypothyroidism, hypoglycemia, malnutrition, vitamin deficiencies, dehydration, and kidney or liver failure.
Substance-induced conditions, such as drug interactions, medication side-effects, alcohol and drug abuse.
Psychological factors, such as depression, emotional trauma, chronic stress, psychosis, chronic sleep deprivation, and delirium.
Infections, such as meningitis, encephalitis, and syphilis.
Stages : Very Severe Decline
Stage seven is the final stage of Alzheimers. Because the disease is a terminal illness, people in stage seven are nearing death. In stage seven of the disease, people lose the ability to communicate or respond to their environment. While they may still be able to utter words and phrases, they have no insight into their condition and need assistance with all activities of daily living. In the final stages of Alzheimers, people may lose their ability to swallow.
Need Alzheimers Care?
You May Like: Alzheimer’s Purple Color Code
Health Environmental And Lifestyle Factors
Research suggests that a host of factors beyond genetics may play a role in the development and course of Alzheimers. There is a great deal of interest, for example, in the relationship between cognitive decline and vascular conditions such as heart disease, stroke, and high blood pressure, as well as conditions such as diabetes and obesity. Ongoing research will help us understand whether and how reducing risk factors for these conditions may also reduce the risk of Alzheimers.
A nutritious diet, physical activity, social engagement, and mentally stimulating pursuits have all been associated with helping people stay healthy as they age. These factors might also help reduce the risk of cognitive decline and Alzheimers. Researchers are testing some of these possibilities in clinical trials.
Racial And Ethnic Differences In The Prevalence Of Alzheimer’s And Other Dementias
Although there are more non-Hispanic whites living with Alzheimer’s and other dementias than any other racial or ethnic group in the United States , older black/African Americans and Hispanics/Latinos are disproportionately more likely than older whites to have Alzheimer’s or other dementias., , – Most studies indicate that older black/African Americans are about twice as likely to have Alzheimer’s or other dementias as older whites., , Some studies indicate older Hispanics/Latinos are about one and one-half times as likely to have Alzheimer’s or other dementias as older whites.,, , However, Hispanics/Latinos comprise a very diverse group in terms of cultural history, genetic ancestry and health profiles, and there is evidence that prevalence may differ from one specific Hispanic/Latino ethnic group to another .,
There is evidence that missed diagnoses of Alzheimer’s and other dementias are more common among older black/African Americans and Hispanics/Latinos than among older whites., Based on data for Medicare beneficiaries age 65 and older, it has been estimated that Alzheimer’s or another dementia had been diagnosed in 10.3% of whites, 12.2% of Hispanics/Latinos and 13.8% of black/African Americans. Although rates of diagnosis were higher among black/African Americans than among whites, according to prevalence studies that detect all people who have dementia irrespective of their use of the health care system, the rates should be even higher for black/African Americans.
Also Check: Alzheimer Disease Life Expectancy After Diagnosis
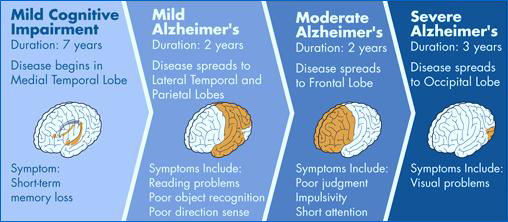
The Stages Of Alzheimers Disease
The only certainty when diagnosed with Alzheimer’s disease is that a seniors condition will progressively worsen. The national Alzheimers Association has developed a very useful staging system to use as a frame of reference when coping with AD.
Alzheimer’s disease constantly keeps doctors, family members and caregivers on their toes. It is instinctive for humans to want a roadmap or some sort of guide to help get us through a journey or a difficult situation. We strive to know what lies ahead to help ensure that we are adequately prepared. Following a serious medical diagnosis like Alzheimers disease , it is only natural to explore the subject with some research. What can we expect and when can we expect it?
Keep in mind that the following staging system is not foolproof, but it can give caregivers a general idea of where their aging loved one falls along the Alzheimers disease spectrum. Seniors with Alzheimers are not guaranteed to follow these stages in a direct line. No matter how much we would like to know exactly what stage someone is in and what symptoms will develop next, we cannot. No two Alzheimers patients are exactly the same. To make matters even more complex, a patients symptoms often vary from day to day. Today, a loved one may seem like they are in stage five, and tomorrow their behaviors and symptoms may align more closely with stage four or stage six.
Preclinical Alzheimers Or No Impairment
You may only know about your risk of Alzheimers disease due to your family history. Or, your doctor may identify biomarkers that indicate your risk.
If youre at risk of Alzheimers, your doctor will interview you about memory problems. However, there will be no noticeable symptoms during the first stage, which can last for years or decades.
Abnormal accumulation of a type of protein called tau in the fluid around your brain and spinal cord is associated with the development of Alzheimers disease. Changes in the levels of this protein can occur about 15 years before symptoms start.
Caregiver support: Someone in this stage is fully independent. They may not even know they have the disease.
Recommended Reading: Prevagen For Dementia
Low Resource Health Settings
More than half of all people with dementia are from low and middle-income countries. Alzheimers disease, other dementias, and non-communicable diseases are expected to continue to be a burden on health systems throughout sub-Saharan Africa, as country populations age and communicable disease mortality and morbidity go down . The number of people with Alzheimer’s disease and dementia in general is estimated to increase far more rapidly in the upper middle, lower middle and low-income countries than in the high-income countries . There is a general lack of awareness of the disease among the population, therefore patients don’t seek for medical care and do not get the treatment they need. Hence, it is under-recognised, underdisclosed, undertreated, and undermanaged, particularly in LMICs. The living environment also often poses little cognitive challenge because families may not understand their relatives behaviour . Many of the cognitive and functional assessment tools used in LMICs were originally developed and validated in High Income Countries. There is a need to adapt it to be used more effectively in LMICs .
Stage : Very Severe Cognitive Decline
This severe late stage of AD is the sad time when a patients speech becomes unrecognizable, urinary and bowel incontinence set in, eating unassisted is difficult, if not impossible, and swallowing can be impaired . Seniors in the advanced stage usually need assistance and support with walking, sitting, standing up and transfers. If a patient is able to stand up at this stage, it is likely that they are very unsteady on their feet. They should be closely monitored as falls can be a dangerous complication. A dementia patients needs become so great in these later stages that it is vital for caregivers to seek out assistance, either in the form of in-home care, a memory care facility or even hospice care.
Family caregivers often become frantic when their loved ones refuse to eat later on in the disease. There is little we can do to ameliorate their symptoms, so we resort to providing food as a way of offering comfort and showing we care. However, this can be risky as the patient becomes frailer. Dysphagia can easily result in aspiration of food particles and saliva into the lungs, which may develop into pneumoniaa dangerous and often deadly infection. As neurological damage progresses, patients may not know what to do with food that is put in their mouths or be able to coordinate the complex movements involved in chewing and swallowing. Those at the end of life may refuse to eat altogether because their organs are shutting down and can no longer process food.
Also Check: What’s The Difference Between Dementia And Alzheimer’s And Senility
Facts About Alzheimer Disease
Alzheimer disease is becoming more common as the general population gets older and lives longer. Alzheimer disease usually affects people older than 65. A small number of people have early-onset Alzheimer disease, which starts when they are in their 30s or 40s.
People live for an average of 8 years after their symptoms appear. But the disease can progress quickly in some people and slowly in others. Some people live as long as 20 years with the disease.
No one knows what causes Alzheimer disease. Genes, environment, lifestyle, and overall health may all play a role.
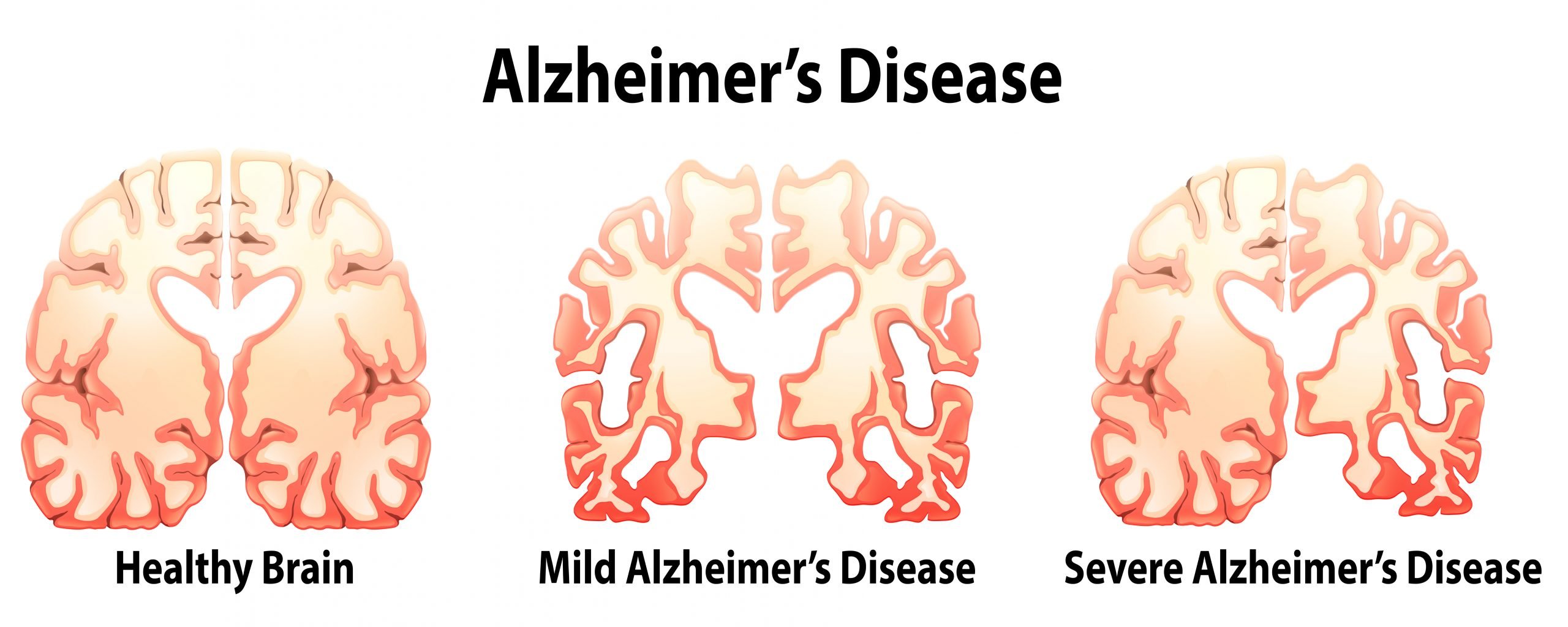
Brain Changes Associated With Alzheimer’s Disease
A healthy adult brain has about 100 billion neurons, each with long, branching extensions. These extensions enable individual neurons to form connections with other neurons. At such connections, called synapses, information flows in tiny bursts of chemicals that are released by one neuron and detected by another neuron. The brain contains about 100 trillion synapses. They allow signals to travel rapidly through the brain’s neuronal circuits, creating the cellular basis of memories, thoughts, sensations, emotions, movements and skills.
The accumulation of the protein fragment beta-amyloid outside neurons and the accumulation of an abnormal form of the protein tau inside neurons are two of several brain changes associated with Alzheimer’s.
Plaques and smaller accumulations of beta-amyloid called oligomers may contribute to the damage and death of neurons by interfering with neuron-to-neuron communication at synapses. Tau tangles block the transport of nutrients and other essential molecules inside neurons. Although the complete sequence of events is unclear, beta-amyloid may begin accumulating before abnormal tau, and increasing beta-amyloid accumulation is associated with subsequent increases in tau.,
Recommended Reading: Alzheimer’s Neurotransmitters Affected
Stage : Very Severe Alzheimers
Stage seven is the end stage of Alzheimers. As a terminal illness, people in this stage are approaching death, and will require around-the-clock assistance with all daily activities. At this stage, a person has usually lost most of their ability to communicate or respond to their environment. They will likely have trouble walking, sitting up or even holding their head up. People in this last stage will typically require assistance to perform all daily activities, including eating, bathing and using the bathroom.
Common Difficulties of Very Severe Alzheimers
- Little memory of recent events, personal history or childhood
- Further loss of bodily control, including inability to walk
- Diminished speech or ability to communicate
- Requiring additional assistance for daily living, including bathing and using the bathroom
- Noticeable personality changes and behavioral problems
- Confusion of environment and overall surroundings
Alzheimers progression typically occurs over the course of four to 20 years, gradually worsening over time. The life expectancy of a person with Alzheimers varies greatly. On average, a person with the disease has between three and 11 years following diagnosis, however it is possible to live for 20 years or more with the disease. Although there is currently no prevention or cure, the more our loved ones can learn about the stages and symptoms of Alzheimers, the more they will know what to expect and how best to provide help and support.
Trends In Dementia Caregiving
There is some indication that families are now better at managing the care they provide to relatives with dementia than in the past. From 1999 to 2015, dementia caregivers were significantly less likely to report physical difficulties and financial difficulties related to care provision. In addition, use of respite care by dementia caregivers increased substantially . However, as noted earlier, more work is needed to ensure that interventions for dementia caregivers are available and accessible to those who need them. A 2016 study of the Older Americans Act’s National Family Caregiver Support Program found that over half of Area Agencies on Aging did not offer evidence-based family caregiver interventions.
FIGURE 11
Also Check: Alzheimers Dement
How To Minimize Urinary Incontinence
There are many ways to minimize urinary incontinence. The solution for each individual will depend on the cause, or causes, in their unique case.
A multi-pronged approach, tailor-fit to their situation, will likely be most effective.
Locate the Toilet
Placing signs, or a trail of masking tape on the floor, to help the person find the toilet may help.
Sometimes pictures are easier for the person to understand than written words.
Keep the light on in the bathroom, or place a portable commode, or urinal, at the bedside to help someone who has trouble finding the bathroom during the night.
Replace Troublesome Clothing
Elastic waistbands can make toileting easier for those who have difficulty managing buttons or zippers.
Watch for Non-Verbal Clues
Pay attention to the persons non-verbal communication. Even if they cant always articulate that they need the bathroom, people often show outward behavioral signs.
Common signs of needing the restroom include:
- Fidgeting with or removing clothing
- Pacing, wandering or going in and out of different rooms
- Peering around frantically
Toileting Plan
One of the best ways to minimize incontinence is to develop a personalized toileting plan based on the persons needs.
Initially, the plan may be as simple and informal as reminding the person to use the bathroom before leaving the house.
Over time, the frequency and amount of oversight or assistance may increase.
Remind or assist them regularly just before they are likely to need it.
Example:
Moderate Dementia Or Moderately Severe Decline
Stage 5 lasts about 1 1/2 years and requires a lot of support. Those who dont have enough support often experience feelings of anger and suspicion.
People in this stage will remember their own names and close family members, but major events, weather conditions, or their current address can be difficult to recall. Theyll also show some confusion regarding time or place and have difficulty counting backward.
Caregiver support: People will need assistance with daily tasks and can no longer live independently. Personal hygiene and eating wont be an issue yet, but they may have trouble picking the right clothing for the weather or taking care of finances.
Recommended Reading: How To Get A Person With Dementia To Shower
Alzheimers Disease Vs Mild Cognitive Impairment
Early dementia, also known as mild cognitive impairment , involves problems with memory, language, or other cognitive functions. But unlike those with full-blown Alzheimers, people with MCI are still able to function in their daily lives without relying on others.
According to the Alzheimers Association, about 15 to 20 percent of people over the age of 65 experience mild cognitive impairment. Many people with MCI eventually develop Alzheimers disease or another type of dementia. However, others plateau at a relatively mild stage of decline and are able to live independently. Some people with mild cognitive impairment even return to normal.
Symptoms of MCI include:
- Frequently losing or misplacing things.
- Frequently forgetting conversations, appointments, or events.
- Difficulty remembering the names of new acquaintances.
- Difficulty following the flow of a conversation.
It is not yet fully understood why MCI progresses to Alzheimers disease in some, while remaining stable in others. The course is difficult to predict, but in general, the greater the degree of memory impairment, the greater the risk of developing Alzheimers down the line.
Stage : Moderately Severe Decline
Your loved one might start to lose track of where they are and what time it is. They might have trouble remembering their address, phone number, or where they went to school. They could get confused about what kind of clothes to wear for the day or season.
You can help by laying out their clothing in the morning. It can help them dress by themselves and keep a sense of independence.
If they repeat the same question, answer with an even, reassuring voice. They might be asking the question less to get an answer and more to just know you’re there.
Even if your loved one can’t remember facts and details, they might still be able to tell a story. Invite them to use their imagination at those times.
Don’t Miss: Purple Ribbon Alzheimer’s
Medications To Maintain Mental Function In Alzheimer’s Disease
Several medications are approved by the U.S. Food and Drug Administration to treat symptoms of Alzheimers. Donepezil, rivastigmine, and galantamine are used to treat the symptoms of mild to moderate Alzheimers. Donepezil, memantine, the rivastigmine patch, and a combination medication of memantine and donepezil are used to treat moderate to severe Alzheimers symptoms. All of these drugs work by regulating neurotransmitters, the chemicals that transmit messages between neurons. They may help reduce symptoms and help with certain behavioral problems. However, these drugs dont change the underlying disease process. They are effective for some but not all people and may help only for a limited time.
A Word About Progression
Alzheimers typically progresses slowly and transitions from mild to severe symptoms. The rate of progression varies widely between people. People with Alzheimers live an average of 4 to 8 years after their diagnosis, but some people live more than 20 years.
The risk of progressing to a higher stage increases with age. For example, in a
Also Check: Ribbon Color For Dementia