Late Stage Alzheimers: What To Expect
Alzheimers disease affects every aspect of personality and behavior. Patients become forgetful. They struggle to talk, lose control of their emotions, and neglect basic tasks. By the time they enter late stage Alzheimers, they will no longer be able to function on their own. Whereas before they retained some limited autonomy, now patients depend entirely on their family. Motor skills become fatally compromised, placing even greater demands on caregivers. While there will still be moments of happiness, families must be prepared for the hard choices they face in order to ensure their loved ones physical and emotional wellbeing.
Mild Alzheimers Or Moderate Decline
Stage 4 lasts about 2 years and marks the beginning of diagnosable Alzheimers disease. You or your loved one will have more trouble with complex but everyday tasks. Mood changes like withdrawal and denial are more evident. Decreased emotional response is also frequent, especially in challenging situations.
New signs of decline that appear in stage 4 may include:
- losing memory of personal history
- trouble with handling finances and bills
- inability to count backward from 100 by 7s
A clinician will also look for a decline in areas mentioned in stage 3, but theres often no change since then.
Caregiver support: Itll still be possible for someone to recall weather conditions, important events, and addresses. But they may ask for help with other tasks like writing checks, ordering food, and buying groceries.
Dying From Dementia With Late
The death of your loved one can be a hard concept to wrap your head around and accept. But knowing what to expect can help you when your loved one has late-stage dementia. It might help to understand what’s coming in the future so you can prepare emotionally and practically.
This article explains how dementia progresses and what happens during late-stage dementia.
Read Also: Senile Dementia Treatments
What To Expect At The End Of Life
The way people with Alzheimerâs disease die is different from person to person, but thereâs a basic pattern to the process. They slowly lose the ability to control basic body functions, such as eating, drinking, and toileting. After a while, their body shuts down.
They canât move much on their own. They donât want to eat or drink, and they lose weight. They often get seriously dehydrated. It can get hard for them to cough up fluid from their chest. In the last stages, many people with dementia get pneumonia.
Some other common signs that someone with Alzheimerâs disease is close to the end of their life include:
- They speak very few or no words.
- Theyâre not able to do very basic activities such as eat, move from a bed to a chair, or change their position in a bed or chair.
- They canât swallow well.
- They get sores because they sit or lie in the same position for too long. These are called bedsores or pressure ulcers.
Where To Care For A Person In The Last Stages Of Dementia
When your loved one moves into the last stages of Dementia, you have a number of options for his or her care. The best time to decide about where they should spend the last months of their life should occur during the earlier stages when the patient can still participate in the decision. Moving dementia patients in the later stages can have significant challenges for both patients and caregivers. Dementia patients can receive support in the following settings:
Traditional home Your lovedone can continue to live in his or her own home as long as they receiveappropriate care services and the proper medical equipment is available for use
Assisted living The same asabove but in a building where the patient has a private appointment, and memorycare and other services are provided
Nursing home Onky appropriateif the patient has other accompanying health issues
Those experiencing late-stage Dementia often have more frequent hospital stays, but staying for a long time in a hospital setting is generally unfeasible. When dementia patients have entered the terminal phase of their lives, their caregivers can elect to obtain hospice services, either in the home or at a stand-alone hospice facility, to keep their loved ones as comfortable as possible.
Read Also: Ribbon Color For Alzheimer’s
How Can I Support Someone With Dementia Towards The End Of Life
Knowing the person will make it easier to provide person-centred care that is focused on what they need and want. It can help to know about their likes, dislikes and their wishes for how they want to be cared for. If the person isnt able to tell you about themselves, speak to their family, friends or other people who know them well.
Its a good idea to find out if the person has a copy of This is me , a document that records information about themselves. If you cant speak to the person, ask those close to them if they have a copy. They may have these details recorded in their care plan.
There are many ways to support someone with dementia at the end of life.
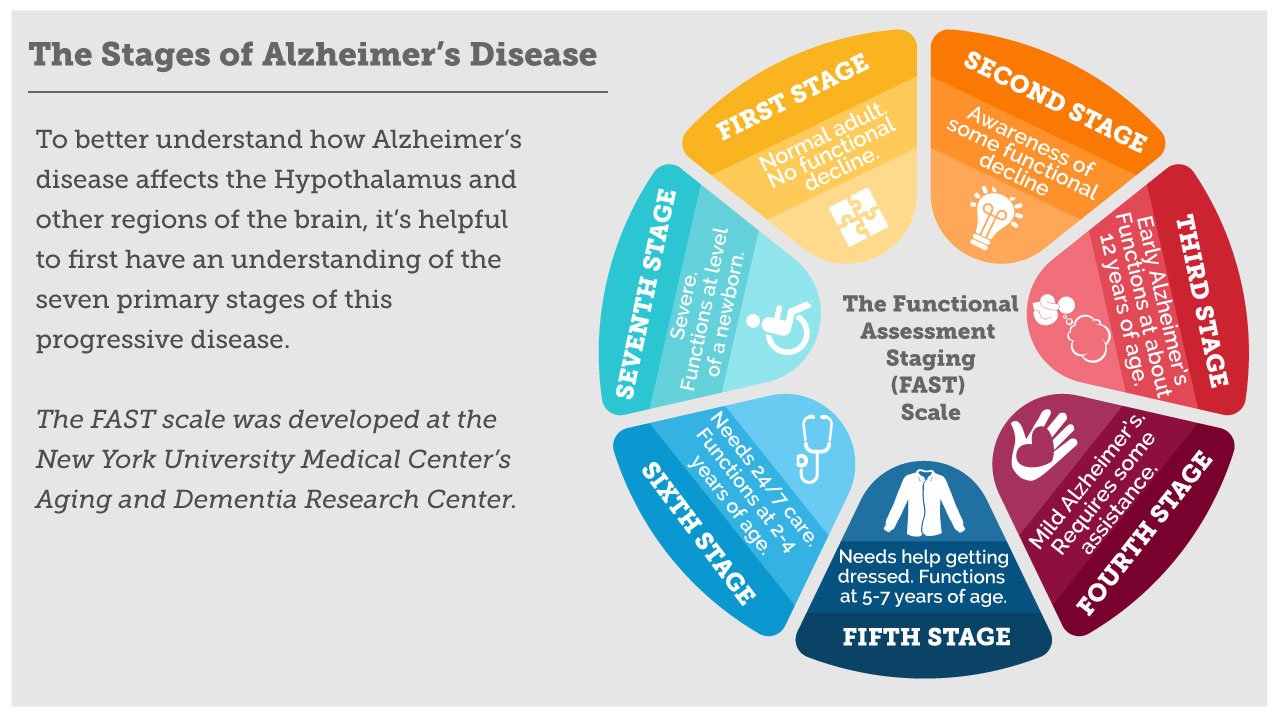
Stages Of Alzheimer Disease
The stages of Alzheimer disease usually follow a progressive pattern. But each person moves through the disease stages in his or her own way. Knowing these stages helps healthcare providers and family members make decisions about how to care for someone who has Alzheimer disease.
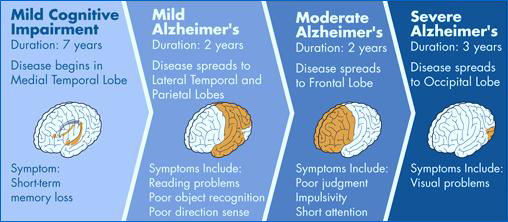
Preclinical stage. Changes in the brain begin years before a person shows any signs of the disease. This time period is called preclinical Alzheimer disease and it can last for years.
Mild, early stage. Symptoms at this stage include mild forgetfulness. This may seem like the mild forgetfulness that often comes with aging. But it may also include problems with concentration.
A person may still live independently at this stage, but may have problems:
-
Remembering a name
-
Staying organized
-
Managing money
The person may be aware of memory lapses and their friends, family or neighbors may also notice these difficulties.
Moderate, middle stage. This is typically the longest stage, usually lasting many years. At this stage, symptoms include:
-
Increasing trouble remembering events
-
Problems learning new things
-
Trouble with planning complicated events, like a dinner
-
Trouble remembering their own name, but not details about their own life, such as address and phone number
-
Problems with reading, writing, and working with numbers
As the disease progresses, the person may:
Physical changes may occur as well. Some people have sleep problems. Wandering away from home is often a concern.
Recommended Reading: How To Change Diaper Of Dementia Patient
Support For People With Dementia And Carers
UCL covid-19 decision aid – a tool to support carers of people living with dementia to make difficult decisions during covid-19
Alzheimers Society end of life care information for patients and families
Alzheimers Society information and fact sheets on all aspects of dementia including what is dementia, types of dementia and living well with dementia
Alzheimer Scotland specialist services for patients and carers
Dementia UK expert one-on-one advice and support to families living with dementia via Admiral Nurses
Behavioral And Cognitive Symptoms Of Dementia
Behavioral Symptoms
Michelle Niedens, L.S.C.S.W., in The Neuropsychiatric Symptoms of Alzheimers, states that 80% of individuals with dementia will experience neuropsychiatric symptoms.
Personality changes such as anxiety, depression or irritability are common in the early stages of the disease. Later, agitation, physical or verbal outbursts, pacing and restlessness are more common.
Behavioral symptoms have been identified as the most challenging and distressing for caregivers and family members. They are oftentimes the determining factor in deciding to move a family member with Alzheimers into a structured living environment.
Cognitive Symptoms
Cognitive symptoms start out mild in the early stages of Alzheimers and gradually worsen as each stage progresses. In the late stages of Alzheimers, the person with the disease is no longer able to form new memories or access old ones. Language abilities become worse until the person is no longer able to communicate. Judgment and reasoning skills continue to diminish and eventually, the person with dementia loses the ability to reason altogether.
Also Check: Smelling Farts Dementia
Resiliency In End Stage Alzheimers
But Fazio said that not all hope has to be lost in this final stage. As researchers learn more about the disease, theyre discovering that end stage Alzheimers can look very different for each individual and a lot may have to do with environmental factors.
Theres research saying what are some of the environmental factors that can make people more functional later into the disease, he said. Both social and physical approaches can support someone into being more functional .
He notes these environmental factors revolve around a person-centered approach, which hes focused on in his own research.
How can I help perform to the best of their ability for as long as possible? Fazio said. Its a new area of research, and being talked about in the psycho-social world. Theres a lot of different things youd see about the impact of this disease negative things like stress and burden. Now you see the research community shifting, and saying, how can we look at a more comprehensive view of this disease? We know theres stress and burden, impairment, that people are progressive. Yet we also see theyre showing resiliency and improved quality of life. How can we learn from that and replicate it?
How To Find Help For Caregiving
As the person moves through the stages of Alzheimer’s, he or she will need more care. You may not be able to meet all his or her needs at home anymore. It’s important to know your limits, take care of yourself, and to seek help whenever you need it. Learn more about getting help with Alzheimer’s caregiving and finding ways to care for yourself. If caring for the person has become too much for you, you can also learn more about finding long-term care for a person with Alzheimer’s.
Don’t Miss: Does Prevagen Help Dementia
Stage : Severe Decline
As Alzheimer’s progresses, your loved one might recognize faces but forget names. They might also mistake a person for someone else, for instance, think their wife is their mother. Delusions might set in, such as thinking they need to go to work even though they no longer have a job.
You might need to help them go to the bathroom.
It might be hard to talk, but you can still connect with them through the senses. Many people with Alzheimer’s love hearing music, being read to, or looking over old photos.
At this stage, your loved one might struggle to:
- Feed themselves
- Changes in their sleeping patterns
Getting Prepared For A Death
Care staff need to know the persons wishes for their death: where they would prefer to be when they die, who should be present, how pain might be treated, and so on. A persons spiritual and cultural needs are important throughout their life, but may take on a particular significance at the end of their life. We can only support a person nearing death properly if we know this information and have recorded it accurately so they have the best possible, and personalised, end-of-life care
Ensuring that a person is as physically comfortable as possible when they are dying also takes preparation. Is a hospital-style bed available, for example, if it is needed? Is a suitable mattress to hand? How can dignity best be maintained if all personal care is provided at a persons bedside? Does the persons room need to be altered in any way, for example fitting new lighting?
Relatives also need to be prepared. For family, having a good relationship with care staff may be a critical part of the lead-in to this dying phase. You also need to know family members wishes at this time. For example, do they want to be present for the death if possible?
Also Check: What Is The 7th Stage Of Alzheimer’s
Support For Dementia Caregivers At The End Of Life
Caring for people with Alzheimers or other dementias at home can be demanding and stressful for the family caregiver. Depression is a problem for some family caregivers, as is fatigue, because many feel they are always on call. Family caregivers may have to cut back on work hours or leave work altogether because of their caregiving responsibilities.
Many family members taking care of a person with advanced dementia at home feel relief when death happensfor themselves and for the person who died. It is important to realize such feelings are normal. Hospicewhether used at home or in a facility gives family caregivers needed support near the end of life, as well as help with their grief, both before and after their family member dies.
Offer Touch And Human Contact
Sit with the person, hold their hand and talk to them as if they can still hear you. Hearing can be the last sense that a person loses at death. This shows that you care and shows respect. If family are at their loved ones bedside, stay with the person when the relative has a break, and again hold the persons hand.
The care team would need to plan how you can provide this kind of one-to-one support.
Don’t Miss: What Color Is Alzheimer’s Ribbon
Provide Physical Comfort And Care
Assess the person to ensure they are not in discomfort or restless, and offer the kind of care described in the above section . Reduce any interventions to only what is necessary, for example change the persons position every few hours or when they need changing.
Give regular mouth care. This can be done hourly to prevent the persons mouth from becoming dry. Apply Vaseline to keep lips moist.
Give eye care, for example use a soft piece of wet clean gauze to prevent the persons eyes from looking sticky.
How To Ensure The Person Eats Well
In the later stages of Alzheimers disease, many people lose interest in food and caregivers may notice changes in how or when they eat. They may not be aware of mealtimes, know when they’ve had enough food, or remember to cook. If they are not eating enough different kinds of foods, they may not be getting the nutrients they need to stay healthy.
Here are some suggestions to help a person with late-stage Alzheimer’s eat better. Remember that these are just tipstry different things and see what works best for the person:
- Serve bigger portions at breakfast because it’s the first meal of the day.
- Offer several smaller meals throughout the day.
- Serve meals at the same time each day.
- Make the eating area quiet. Turn off the TV or radio.
- Control between-meal snacks. Lock the refrigerator door and food cabinets if necessary.
- If the person has dentures, make sure they fit. Loose dentures or dentures with bumps or cracks may cause choking or pain, making it harder to eat. Remove poorly fitting dentures until the person can get some that fit.
- Let the person’s doctor know if they lose a lot of weight, for example, if he or she loses 10 pounds in a month.
You can also try different ways of preparing the person’s plate. For example:
If the person needs help eating, you might try to:
When choosing foods to eat and liquids to drink, these suggestions might help:
Don’t Miss: Dementia Color Ribbon
Final Signs And What To Do
If it has been established that the person is now dying and they become restless, this is often referred to as terminal restlessness. It is important to recognise restlessness and report it to a doctor or nurse immediately. Restlessness could be due to pain or high temperature and needs to be relieved.
If you notice the person is restless and you think they are uncomfortable, you could try helping them move into a more comfortable position. If this does not help, seek advice as they may need pain relief. Likewise, if you notice the person is hot to touch then they may need to be cooled down by a fan or cool flannel on their forehead and given rectal paracetamol by the nurse. They may also need medication to relieve the restlessness if the above does not help.
As death approaches the persons breathing pattern can change. This is caused by the person going into unconsciousness. It is often called Cheyne-Stoke breathing. The person may have periods where they have regular breathing, then stop breathing for a few seconds. Breathing usually gets faster and there can be long gaps in between. The person who is dying is unaware of this but family members may find this quite distressing. It is important that you or another senior member of staff explain to the relatives that this is what is to be expected and that the person is unaware. It is natural.
Why Do Dementia Patients Stop Talking
There are many signs that can tell you death is near for a dementia payment. Even though you may be prepared for the end, it is never easy. The ten signs that death is near include:
Don’t Miss: Is Senility The Same As Dementia
What To Do About Swallowing Problems
As Alzheimer’s disease progresses to later stages, the person may no longer be able to chew and swallow easily. This is a serious problem. Difficulty with swallowing may lead to choking or cause food or liquid to go into the lungs, which is known as aspiration. This can cause pneumonia, which can lead to death.
The following suggestions may help with swallowing:
- Make sure to cut food into small pieces and that it is soft enough for the person to eat.
- Grind or blend food to make it easier to eat.
- Offer soft foods, such as yogurt, applesauce, mashed avocado, sweet potatoes, and bananas.
- Don’t use a straw, which may cause more swallowing problems. Instead, have the person drink small sips from a cup.
- Offer drinks of different temperatures warm, cold, and room temperatureto see which might be easiest for the person to drink.
- Don’t hurry the person. He or she needs time to chew and swallow each mouthful before taking another bite.
- Encourage the person to feed themselves as much as possible during meals. If the person needs support, try using overhand, underhand, or direct hand feeding approaches.
- Don’t feed a person who is drowsy or lying down. He or she should be in an upright, seated position during the meal and for at least 20 minutes after the meal.
- Say “swallow” to remind him or her to swallow.
- Find out if the person’s pills can be crushed or taken in another form.