Can Amyloid Plaques Be Dissolved Or Reduced
This question has been the focus of drug development for many years. BrightFocus has funded the work of scientists who have shown various methods of clearing away plaques. For example, Dr. Matthew Campbell has experimented with temporarily disrupting the blood-brain barrier to clear out existing plaques. After many heartbreaking clinical trial failures, there is growing concern among the scientific and medical communities that clearing plaques may not be sufficient to treat the disease. This is a very active area of research.
Why Do Protein Deposits Form In The First Place
Researchers want to know why these protein aggregates form in the first place, how they distribute in the brain, how their signalling works, and how they and their precursors cause neurodegeneration.
A range of theories have been put forward to explain what kickstarts damaging protein aggregation. In the case of Alzheimers, this includes problems with the way oxygen is metabolised in brain cells and the movement of internal cell contents. The brains response to inflammation, and its systems for clearing waste could also play a role.
One main theory is that once amyloid-ß begins to accumulate, it then promotes the build-up of tau. But the relationship is not simple, because tau also has a role in influencing the toxic effects of amyloid-ß.
Although some genetic risk factors for dementias have been identified, particularly for Alzheimers disease , we still dont know how these act to influence protein aggregation and cause degeneration. This is a key area of research focus, and knowing the answers to these questions is crucial to the prevention and treatment of dementia.
Inactivating Cofilin 1 Impairs Dendritic Spines
Phosphorylation, or the addition of a phosphoryl group, to cofilin 1, however, renders the protein inactive.
The researchers observed how exposure to beta-amyloid peptides in cultured brain cells led to more phosphorylated cofilin 1. This reduced the dynamism of actin filaments and, in turn, impaired the ability of dendritic spines to receive signals.
Further investigation revealed that an enzyme called Rho-associated protein kinase could be a target for reducing cofilin 1 phosphorylation. The enzyme activates and deactivates other molecules through phosphorylation.
Tests with a drug called Fasudil that blocks ROCK showed that it reversed the effects that the team observed in the actin filaments.
He suggests that further research into drugs that specifically stop that phosphorylation of cofilin 1 in brain cells could be a promising avenue for finding new Alzheimers disease treatments.
We have not come up with an action mechanism, but we confirmed that the inhibition of the phosphorylation pathway of cofilin 1 prevents exposure to beta-amyloid peptides from causing the deactivation of the protein and the consequent effect on the cytoskeleton of the dendritic spines.
José Martínez-Hernández, Ph.D.
Read Also: Smelling Farts Prevents Cancer
When To See A Doctor
If you have concerns about your memory or thinking skills, you should talk to your doctor for a thorough assessment of whether your symptoms are due to Alzheimers disease or other reasons including Parkinsons disease, tumor, stroke, infections, side effects of other medications, or a non-Alzheimers dementia.
Some of these conditions, unlike with Alzheimers, can possibly be reversible and treatable. However, if a patient has been diagnosed with the disease, undergoing treatment during the early stages of Alzheimers does not only give them some more time to function independently, but it can also help their family plan for the future, avoid possible safety issues, and widen their support system.
Patients are often diagnosed during the mild stage of Alzheimers disease. If you are having concerns involving memory problems and thinking skills that you are beginning to notice in a family member or friend, talk to them about these concerns and ask if you can accompany them to the doctors office.
A Step Closer To Understanding How Brain Cells Die In Alzheimer’s Disease
New research from the Australian Institute for Bioengineering and Nanotechnology at the University of Queensland has brought us a step closer to understanding how protein clumps called amyloid plaques contribute to the death of brain cells in Alzheimers disease.
The research, published in the highly regarded journal Stem Cell Reports, shows that an increased production of plaques surprisingly does not lead to an increase in brain cell death, suggesting that they dont kill neurons directly or, if they do, they dont work alone.
Currently, Alzheimers disease effects around a quarter of a million Australians, accounting for more than two-thirds of all dementia cases.
One of the major hallmarks of Alzheimers disease is the accumulation of the so-called beta-amyloid plaques. These plaques are formed when a type of protein in the brain, called amyloid precursor protein , is broken down into smaller fragments. These fragments, which are called beta-amyloid, then clump together to form plaques.
It is widely thought that these amyloid plaques contribute to the death of neurons in people with Alzheimers, either directly, or by causing another protein, called tau, to form toxic neurofibrillary tangles. Thus, reducing amyloid plaques has been the focus of many efforts to treat the condition.
People with Down syndrome have an extra copy of chromosome 21, and therefore carry an extra copy of the amyloid precursor protein gene, says lead author Dr Dmitry Ovchinnikov.
Don’t Miss: Does Neil Diamond Have Alzheimer’s
Neurons Lost In Alzheimer’s Created Anew From Stem Cells
04 March 2011
Scientists have transformed a human embryonic stem cell into a type of neuron that is vital for retrieving memories, but dies during the early stages of Alzheimer’s disease, according to a new study.
Now, researchers can grow and study these neurons in a lab dishes to find out why they die, said Christopher Bissonnette, who conducted the work at Northwestern University Feinberg School of Medicine in Chicago.
Researchers can also test drugs for their ability to block the death of these neurons, and thus could delay the onset of memory deficits seen in Alzheimer’s disease, Bissonnette said.
“This would not be a cure for Alzheimer’s,” because it wouldn’t stop the processes that killed the patient’s initial population of these neurons, Bissonnette told MyHealthNewsDaily. “But it would hopefully reverse the memory deficits and symptoms” of the disease.
The study was published today in the journal Stem Cells.
Hope for transplantation
In Alzheimer’s disease, memory abilities fade not because the brain can no longer store memories, but because it has problems retrieving them. That’s largely due to the loss of a small number of neurons, called basal forebrain cholinergic neurons, early in Alzheimer’s, the study said.
Once these neurons are gone, memory rapidly deteriorates, said study researcher Dr. John Kessler, professor of stem cell biology at Northwestern University.
Addressing the questions
Still, questions about these neurons remain, Kessler said.
Loss Of Neuronal Connections And Cell Death
In Alzheimers disease, as neurons are injured and die throughout the brain, connections between networks of neurons may break down, and many brain regions begin to shrink. By the final stages of Alzheimers, this processcalled brain atrophyis widespread, causing significant loss of brain volume.
Learn more about Alzheimer’s disease from MedlinePlus.
You May Like: What Is The Difference Between Dementia And Senility
See First Alzheimers Blood Test Rolled Out For Clinical Use In Us
The most difficult question to answer, according to Llorens-Martín, is what happens to the few new neurons that are born in the brains of people with neurodegeneration. What is failing in the environment that is making these neurons die prematurely or making it very difficult for them to get connected appropriately? she says. It is known that systemic changes occur in in blood, for example, in Alzheimers disease patients several decades before the appearance of the cognitive impairments, she says. Its possible that those changes in the systemic environment or the environment of the brain are somehow decreasing the neurogenic potential of the hippocampus, she adds.
We know that neurogenesis is critical for learning and memory, and we know that the level of neurogenesis decreases with age no matter what, even in normal aging, says Lazarov. And if we maintain greater level of neurogenesis . . . we would be able to maintain greater hippocampal plasticity and intact hippocampal function. This may delay Alzheimers disease greatly.
Medications To Maintain Mental Function In Alzheimer’s Disease
Several medications are approved by the U.S. Food and Drug Administration to treat symptoms of Alzheimers. Donepezil, rivastigmine, and galantamine are used to treat the symptoms of mild to moderate Alzheimers. Donepezil, memantine, the rivastigmine patch, and a combination medication of memantine and donepezil are used to treat moderate to severe Alzheimers symptoms. All of these drugs work by regulating neurotransmitters, the chemicals that transmit messages between neurons. They may help reduce symptoms and help with certain behavioral problems. However, these drugs dont change the underlying disease process. They are effective for some but not all people and may help only for a limited time.
You May Like: Does Meredith Grey Have Alzheimer’s
Support For Families And Alzheimer’s Disease Caregivers
Caring for a person with Alzheimers can have significant physical, emotional, and financial costs. The demands of day-to-day care, changes in family roles, and decisions about placement in a care facility can be difficult. NIA supports efforts to evaluate programs, strategies, approaches, and other research to improve the quality of care and life for those living with dementia and their caregivers.
Becoming well-informed about the disease is one important long-term strategy. Programs that teach families about the various stages of Alzheimers and about ways to deal with difficult behaviors and other caregiving challenges can help.
Good coping skills, a strong support network, and respite care are other things that may help caregivers handle the stress of caring for a loved one with Alzheimers. For example, staying physically active provides physical and emotional benefits.
Some caregivers have found that joining a support group is a critical lifeline. These support groups enable caregivers to find respite, express concerns, share experiences, get tips, and receive emotional comfort. Many organizations sponsor in-person and online support groups, including groups for people with early-stage Alzheimers and their families.
Read about this topic in Spanish. Lea sobre este tema en español.
What Happens To The Brain In Alzheimers Disease
The healthy human brain contains tens of billions of neuronsspecialized cells that process and transmit information via electrical and chemical signals. They send messages between different parts of the brain, and from the brain to the muscles and organs of the body. Alzheimers disease disrupts this communication among neurons, resulting in loss of function and cell death.
Recommended Reading: Does Smelling Farts Help Prevent Dementia
How Is Alzheimer’s Different From Other Forms Of Dementia
Alzheimer’s disease is distinguished from other forms of dementia by characteristic changes in the brain that are visible only upon microscopic examination during autopsy. Brains affected by Alzheimer’s disease often show presence of the following:
-
Fiber tangles within nerve cells
-
Clusters of degenerating nerve endings
Another characteristic of Alzheimer’s disease is the reduced production of certain brain chemicals necessary for communication between nerve cells, especially acetylcholine, as well as norepinephrine, serotonin, and somatostatin.
Models Connect Neurogenesis And Disease
In their latest paper, Arber and colleagues show that neurogenesis in induced pluripotent stem cells looks similar to what happens in the human brain, meaning that stem cell models could help address the question of cause or effect. And if indeed defects in neurogenesis are driving neurodegeneration, a new avenue to intervention opens up.
We diagnose people at seventy years old or seventy-five years old. Thats too late to intervene, says Caghan Kizil, a neuroscientist at the German Center for Neurodegenerative Diseases. But we know that the molecular or pathological onset starts much earlier, he adds, and that means theres a chance scientists and physicians could stall the process, perhaps by tweaking neurogenesis.
Also Check: Does Smelling Farts Help Prevent Dementia
Signs And Symptoms Of Alzheimer’s Disease
Memory problems are typically one of the first signs of cognitive impairment related to Alzheimers. Some people with memory problems have a condition called mild cognitive impairment . With MCI, people have more memory problems than normal for their age, but their symptoms do not interfere with their everyday lives. Movement difficulties and problems with the sense of smell have also been linked to MCI. Older people with MCI are at greater risk for developing Alzheimers, but not all of them do so. Some may even revert to normal cognition.
The first symptoms of Alzheimers vary from person to person. For many, decline in nonmemory aspects of cognition, such as word-finding, vision/spatial issues, and impaired reasoning or judgment may signal the very early stages of the disease. Researchers are studying biomarkers to detect early changes in the brains of people with MCI and in cognitively normal people who may be at greater risk for Alzheimers. More research is needed before these techniques can be used broadly and routinely to diagnose Alzheimers in a health care providers office.
New Treatment For Chronic Diseases
Neurons are nerve cells which are adapted to transmit electrical impulses from one place to another in the human body.
They are the core components of the brain, spinal cord and peripheral nerves .
The research team, with members from the Universities of Bristol, Zurich and Auckland, first modelled equations to explain how neurons respond to electrical stimuli from other nerves before designing the chips.
Tests of the bionic neurons proved they could precisely mimic real, living neurons responding to a range of stimulations.
Read Also: What Shampoos Cause Alzheimer’s Disease And Cancer
Do Brain Cells Die As We Age
With normal aging, we dont find that neurons die in massive numbers. While with Alzheimers disease, the neurons or brain cells die in large numbers in certain areas of the brain.
This is the end product of the process of Alzheimers disease. Alzheimers causes neuron death. And this neuron death manifests as memory, thinking, and behavior changes.
But your brain is so resilient that it is able to adapt for many decades to this cell death.
Neuroscientists believe that when the very first signs of memory, thinking or behavior changes appear in an Alzheimers patient, their neuron loss is approximately 70% in certain areas of the brain.
This 70% loss represents a massive number of dead neurons in brain regions that are earliest affected by Alzheimers disease.
It is a truly remarkable process. Your brain is fighting and largely maintaining cognitive skills until you reach some sort of critical point. It is at this juncture, where a very large percentage of neurons are missing from the brain regions critical for memory formation, that Alzheimers becomes evident.
It is one of the most impressive things, that our brain is able to fight this process, and do a pretty good job of fighting for so long.
What causes this cell death? Alzheimers affects two proteins, beta-amyloid and tau. It causes tangle and plaque formation, brain inflammation, lost connections, and neuronal death.
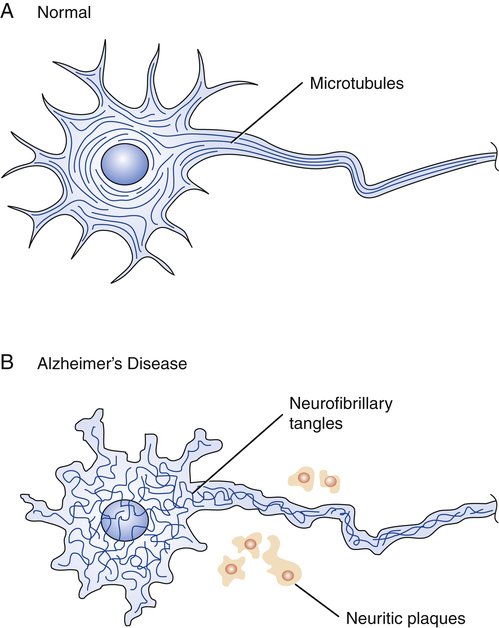
What Causes Neurofibrillary Tangles To Form
Tangles form when tau is misfolded in a very specific way. In Alzheimers disease, the tau forms a C-shape in the core of the tangle with a loose end sticking out randomly. In Picks disease, the core forms a J-shape instead. Once a tangle has been started, more tau proteins are recruited to make it longer. There is likely a molecule responsible for shaping tau into these forms, but it has not yet been identified.
Don’t Miss: Does Medicare Cover Nursing Home Care For Dementia
Medications To Treat The Underlying Alzheimer’s Disease Process
Aducanumab is the first disease-modifying therapy approved by the FDA to treat Alzheimers disease. The medication helps to reduce amyloid deposits in the brain and may help slow the progression of Alzheimers, although it has not yet been shown to affect clinical outcomes such as progression of cognitive decline or dementia. A doctor or specialist will likely perform tests, such as a PET scan or analysis of cerebrospinal fluid, to look for evidence of amyloid plaques and help decide if the treatment is right for the patient.
Aducanumab was approved through the FDAs Accelerated Approval Program. This process requires an additional study after approval to confirm the anticipated clinical benefit. If the follow-up trial fails to verify clinical benefit, the FDA may withdraw approval of the drug. Results of the phase 4 clinical trial for aducanumab are expected to be available by early 2030.
Several other disease-modifying medications are being tested in people with mild cognitive impairment or early Alzheimers as potential treatments.
See What Do New Neurons In The Brains Of Adults Actually Do
Since then, work in animal models and people has indicated that adult hippocampal neurogenesis plays an important role in memory formation and that decreases in neurogenesis accompany aging, as well as cognitive loss and the development of Alzheimers disease, which affects 10 percent of Americans older than 65. But scientists are still figuring out at what point in disease onset or progression adult hippocampal neurogenesis plays a role and whether or not tweaking neurogenesis could help treat or prevent the disease.
You May Like: Meredith Grey Alzheimer\’s Trial
Alzheimers Disease Destroys Brain Connections
Alzheimers is an irreversible brain disease that gets worse over time. It is the most common cause of dementia.
The disease erodes the ability to remember, think, and perform simple tasks, until people with Alzheimers can no longer care for themselves. Most individuals begin to experience symptoms in their mid-60s.
According to the National Institute on Aging, experts believe that there are more than 5.5 million people living with Alzheimers disease in the United States.
Different forms of dementia have different hallmarks. In Alzheimers disease, the distinguishing features include a toxic buildup of beta-amyloid and another protein called tau and the loss of connections between neurons.
Neurons transmit information in the brain and carry signals from the brain to other parts of the body, such as organs and muscles.
The billions of neurons in the brain communicate with each other by sending and receiving chemical messages across specialized structures known as synapses. These structures come and go and strengthen and weaken, depending on experience.
The brain stores long-term information by changing the chemistry and structure of synapses. Scientists believe that the dynamic, fluctuating nature of synapses underpins memory and learning.
When information, in the form of chemical messengers, travels across a synapse from one brain cell to another, branching structures called dendrites bring the signals into the receiving neuron.