Brain Cells Most Vulnerable To Alzheimers Disease Identified By Scientists
Findings Could Lead to Targeted Treatments to Boost Brains Resilience
A major mystery in Alzheimers disease research is why some brain cells succumb to the creeping pathology of the disease years before symptoms first appear, while others seem impervious to the degeneration surrounding them until the diseases final stages.
An image of human brain samples used to study why some brain cells are more vulnerable to Alzheimers disease than others. Image by Rana Eser, UCSF Grinberg lab
Now, in a study published Jan. 10, 2021, in Nature Neuroscience, a team of molecular biologists and neuropathologists from the UCSF Weill Institute for Neurosciences have joined forces to identify for the first time the neurons that are among the first victims of the disease accumulating toxic tangles and dying off earlier than neighboring cells.
We know which neurons are first to die in other neurodegenerative diseases like Parkinsons disease and ALS, but not Alzheimers, said co-senior author Martin Kampmann, PhD, an associate professor in the UCSF Institute for Neurodegenerative Diseases and Chan Zuckerberg Biohub Investigator. If we understood why these neurons are so vulnerable, maybe we could identify interventions that could make them, and the brain as a whole, more resilient to the disease.
Disclosures: The authors declare no competing interests.
Diagnosis Of Dementia Due To Alzheimer’s Disease
- Obtaining a medical and family history from the individual, including psychiatric history and history of cognitive and behavioral changes.
- Asking a family member to provide input about changes in thinking skills and behavior.
- Conducting problem-solving, memory and other cognitive tests, as well as physical and neurologic examinations.
- Having the individual undergo blood tests and brain imaging to rule out other potential causes of dementia symptoms, such as a tumor or certain vitamin deficiencies.
- In some circumstances, using PET imaging of the brain to find out if the individual has high levels of beta-amyloid, a hallmark of Alzheimer’s normal levels would suggest Alzheimer’s is not the cause of dementia.
- In some circumstances, using lumbar puncture to determine the levels of beta-amyloid and certain types of tau in CSF normal levels would suggest Alzheimer’s is not the cause of dementia.
Causes Of Vascular Dementia
Vascular dementia is caused by reduced blood flow to the brain, which damages and eventually kills brain cells.
This can happen as a result of:
- narrowing and blockage of the small blood vessels inside the brain
- a single stroke, where the blood supply to part of the brain is suddenly cut off
- lots of “mini strokes” that cause tiny but widespread damage to the brain
Not everyone who has a stroke will go on to develop vascular dementia.
Read more about vascular dementia.
Don’t Miss: Smelling Farts Dementia
Avoidable Use Of Health Care And Long
6.5.1 Preventable hospitalizations
Preventable hospitalizations are one common measure of health care quality. Preventable hospitalizations are hospitalizations for conditions that could have been avoided with better access to, or quality of, preventive and primary care. Unplanned hospital readmissions within 30 days are another type of hospitalization that potentially could have been avoided with appropriate post-discharge care. In 2013, 21% of hospitalizations for fee-for-service Medicare enrollees with Alzheimer’s or other dementias were either for unplanned readmissions within 30 days or for an ambulatory care sensitive condition . The total cost to Medicare of these potentially preventable hospitalizations was $4.7 billion . Of people with dementia who had at least one hospitalization, 18% were readmitted within 30 days. Of those who were readmitted within 30 days, 27% were readmitted two or more times. Ten percent of Medicare enrollees had at least one hospitalization for an ambulatory care-sensitive condition, and 14% of total hospitalizations for Medicare enrollees with Alzheimer’s or other dementias were for ambulatory care sensitive conditions.
FIGURE 16
| 15,417 | 46,252 |
Manage Or Better Yet Entirely Avoid Other Diseases
So if you have another disease, you want to make sure youre treating that disease under the guidance of your physician. Research studies suggests that avoiding or managing other disease helps reduce the risk of mental decline. Many diseases that we might consider to be outside of the brain can still have an impact on brain health for example, you might want to read our article on high blood pressure and your brain.
You May Like: Does Prevagen Work For Dementia
Diagnosis Of Alzheimer Disease
-
Safety and supportive measures
-
Drugs that may improve mental function
Treatment of Alzheimer disease involves general measures to provide safety and support, as for all dementias. Also, certain drugs can help for a while. The person with Alzheimer disease, family members, other caregivers, and the health care practitioners involved should discuss and decide on the best strategy for that person.
Pain and any other disorders or health problems are treated. Such treatment may help maintain function in people with dementia.
Exercise 150 Minutes Of Aerobic And 2x/week Strength Training
Physical activity has been shown to be really important for the health of your brain. The recommendations are 150 minutes of aerobic exercise weekly. It could be walking briskly, jogging, or cycling each week.
But dont forget about your muscle strength. Its important to improve the strength of your muscles as well. That helps your bones and your body in general, so its recommended to practice strength training a couple of times a week.
Don’t Miss: Does Bobby Knight Have Dementia
Data Suggest Potential Target For Alzheimer’s Disease Treatments
Researchers from Weill Cornell Medical College and Columbia University College of Physicians Surgeons have discovered at least one way in which beta-amyloid, the protein that forms stubborn plaques in the brains of Alzheimer’s disease patients, can kill nerve cells.
Nerve cell death is a hallmark of the memory-robbing disorder, and is thought to be the cause of personality changes and other neurological changes that occur with the disease.
According to a report in the April 16 issue of the journal Science, beta-amyloid, a protein long known to accumulate in plaques in the brains of Alzheimer’s patients, binds to a protein known as ABAD .
Finding a way to inhibit this interaction may help prevent nerve cell death, and possibly help prevent the symptoms of Alzheimer’s disease, according to the research team led by Dr. Hao Wu, Professor of Biochemistry at Weill Cornell Medical College and Weill Cornell Graduate School of Medical Sciences in New York Dr. Shirley ShiDu Yan, Associate Professor of Clinical Pathology at Columbia University College of Physicians Surgeons in New York and Dr. Joyce Lustbader, Senior Research Scientist in Obstetrics and Gynecology at Columbia PS.
The crystal complex is the first demonstration that beta-amyloid peptide binds to a protein called ABAD and accumulates inside the mitochondria in brain cells, said Dr. Lustbader.
The next step is to test the peptide directly in transgenic mice with Alzheimer’s disease-like symptoms, the researchers said.
Trends In The Prevalence And Incidence Of Alzheimer’s Dementia Over Time
A growing number of studies indicate that the prevalence, – and incidence, , – of Alzheimer’s and other dementias in the United States and other higher-income Western countries may have declined in the past 25 years,, , – though results are mixed., , , These declines have been attributed to increasing levels of education and improved control of cardiovascular risk factors., , , , , Such findings are promising and suggest that identifying and reducing risk factors for Alzheimer’s and other dementias may be effective. Although these findings indicate that a person’s risk of dementia at any given age may be decreasing slightly, the total number of people with Alzheimer’s or other dementias in the United States and other high-income Western countries is expected to continue to increase dramatically because of the increase in the number of people at the oldest ages.
3.7.1 Looking to the future: Aging of the baby boom generation
- By 2025, the number of people age 65 and older with Alzheimer’s dementia is projected to reach 7.1 million â almost a 22% increase from the 5.8 million age 65 and older affected in 2020.,
- By 2050, the number of people age 65 and older with Alzheimer’s dementia is projected to reach 13.8 million, barring the development of medical breakthroughs to prevent, slow or cure Alzheimer’s disease.,
FIGURE 5
Also Check: Alzheimer’s Neurotransmitters Affected
Microglia In Alzheimers Disease
There is an extensive number of studies indicating that inflammatory pathways are altered in AD owing to exacerbated immune response . The observation that inflammatory processes may promote neuronal loss and cognitive decline , together with evidence associating polymorphic variations of inflammatory cytokines with AD , argue for a potential role of microglia in AD pathogenesis. Microglia are one of the first immune cells that get activated and recruited to the site of injury during an inflammatory response. Understanding how they are involved in AD could not only help decipher the cellular and molecular mechanisms underlying neurodegeneration, but could also open up new avenues for therapeutic interventions. One of the first ground-breaking findings implicating microglia in AD date from studies in the early 1990s showing that these immune cells are highly engaged in the formation of A plaques in the brains of AD patients . More recently, data from studies utilizing animal models of AD have also demonstrated the presence of activated microglia at sites of A deposition, suggesting that these glial cells might physically interact with A and regulate their levels in the brain .
What Is Cognitive Reserve Could It Help Reduce The Risk Of Dementia
To help define cognitive reserve we will draw an analogy between car tires. Cognitive reserve is like having more tread on the car tires. Cheap tires are thinner and wear out faster and expensive tires that have more tread, last longer.
Some studiessuggest that lifetime exposures including educational and occupational attainment, and leisure activities in late life, can increase this reserve. So, cognitive reserve holds out the promise of interventions that could slow cognitive aging or reduce the risk of dementia.
Lets look at it this way: if my brain has more cognitive reserve I may be able to compensate for the ravages of Alzheimers disease for a longer period of time.
We have intuition that cognitive reserve is important but to actually study it in a fair way across large groups of people is very difficult. We would need a way to measure or score cognitive reserve and theres not a clear way to do that.
If the key to Alzheimers disease were how strong your legs are, we have a very easy way to measure how strong everybodys legs are. But such an approach is lacking for cognitive reserve. This makes the understanding of the importance of cognitive reserve difficult to fully assess. This is one of the reasons why the brain is so hard to study.
Keeping your brain active is good and may delay or slow down the symptoms of dementia.
Read Also: Alzheimer’s Awareness Ribbon
Where Does Mif Strike
Dawson cautions that while parthanatos is known to cause cell death in many brain conditions, MIFs ability to chop up DNA has so far been definitively linked only with strokewhen the MIF gene was disabled in mice, the damage caused by a stroke was dramatically reduced. Were interested in finding out whether MIF is also involved in Parkinsons, Alzheimers, and other neurodegenerative diseases, he says, and that if so, and if an inhibitor of MIF proves successful in testing, it could have implications for treating many conditions.
The research group reports that in work to be published they have also identified a few chemical compounds that block MIFs action in the lab-grown cells, protecting them from parthanatos. Ted Dawson says the group plans to test these compounds in animals and modify them to maximize their safety and effectiveness.
Errors In Dna Inside Brain Cells May Build Up At A Faster Rate In People With Alzheimers Disease
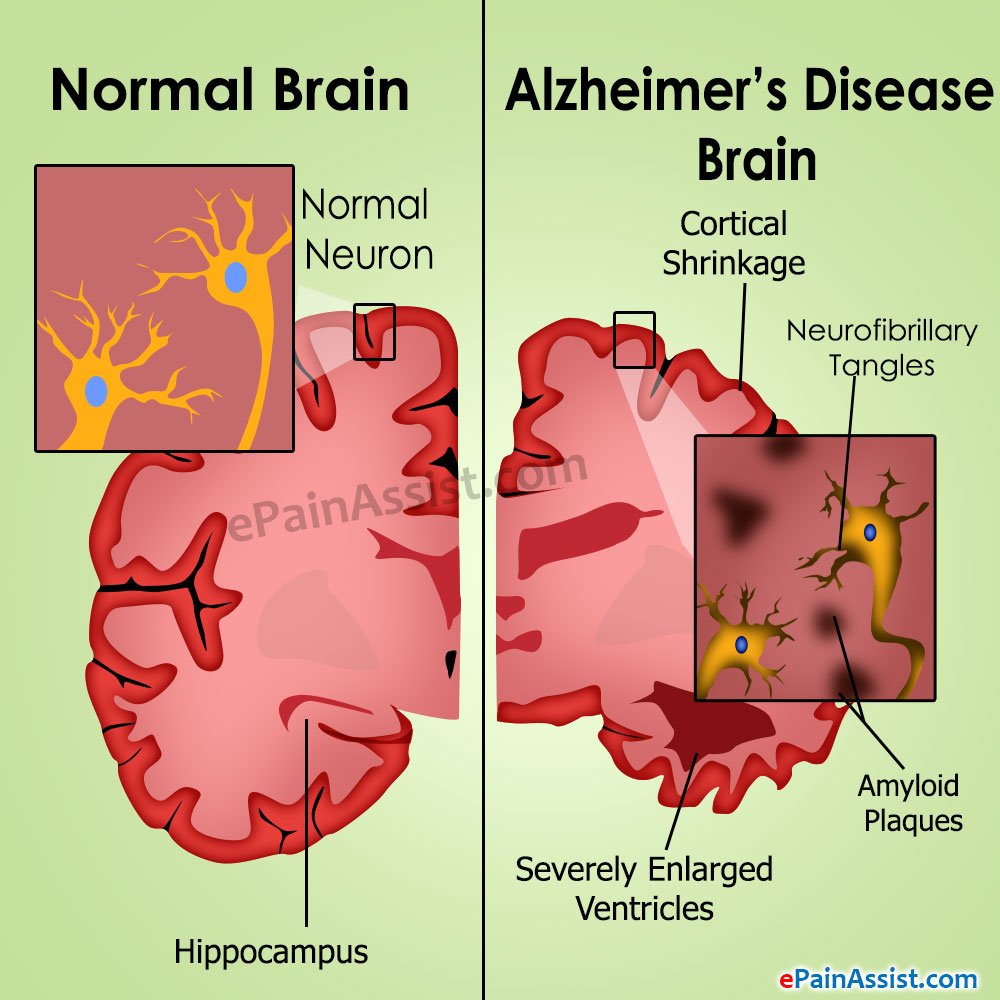
A new study from Brigham and Womens Hospital and Boston Childrens Hospital discovered that patients with Alzheimers disease had a higher number of somatic mutations in their brain cells, and that these mutations differ from people who do not have Alzheimers disease.
Researchers found that changes accumulated in the brain cells of patients with Alzheimers disease at a faster rate, potentially explaining why brain cells die and revealing new pathways to target for treatment.
As we age, errors in DNA inside brain cells can accumulate. But in patients with Alzheimers disease, these errors known as somatic mutations may build up at a faster rate. A new study by investigators from Brigham and Womens Hospital and Boston Childrens Hospital found that patients with Alzheimers disease have a greater number of somatic mutations in their brain cells and that these mutations differed from people without Alzheimers disease. The teams results are published in Nature.
As we age, neurons are known to accumulate somatic mutations. In AD neurons, however, we see more mutations and DNA alterations, said lead author Michael B. Miller, MD, PhD, of the Department of Pathology at the Brigham. Our results suggest that AD neurons experience genomic damage that causes immense stress on cells and creates dysfunction among them. These findings may explain why many brain cells die during AD.
Read Also: Do Dementia Patients Tell The Truth
How Do You Know When An Alzheimer’s Patient Is Dying
In the final stages of Alzheimers disease, neuronal damage and muscle weakness cause patients to lose the ability to coordinate even simple movements. Eventually, they are unable to walk, communicate, control bladder or bowel movements, or feed themselves without significant assistance and careful supervision.
Signs that a patient with Alzheimer’s disease is close to the end of their life include:
- Inability to speak
- Inability to eat or drink because they cant swallow
- Inability to move from a bed to a chair or change their position
- Bedsores or pressure ulcers caused by sitting or lying in the same position for too long
- Unprovoked seizures
- Cold hands, feet, arms, and legs
- Restlessness
- Sleeping for longer periods of time
- Breathing changes such as shallow breaths or periods without breathing for a few seconds
The final stages of Alzheimer’s disease can be emotionally and physically challenging, not only for patients, but also for their family members and caregivers.
Early In Alzheimer Disease
Symptoms develop gradually, so for a while, many people continue to enjoy much of what they enjoyed before developing Alzheimer disease.
Symptoms usually begin subtly. People whose disease develops while they are still employed may not do as well in their jobs. In people who are retired and not very active, the changes may not be as noticeable.
The first and most noticeable symptom may be
-
Forgetting recent events because forming new memories is difficult
-
Sometimes changes in personality
Early in the disease, people become less able to use good judgment and think abstractly. Speech patterns may change slightly. People may use simpler words, a general word or many words rather than a specific word, or use words incorrectly. They may be unable to find the right word.
People with Alzheimer disease have difficulty interpreting visual and audio cues. Thus, they may become disoriented and confused. Such disorientation may make driving a car difficult. They may get lost on their way to the store. People may be able to function socially but may behave unusually. For example, they may forget the name of a recent visitor, and their emotions may change unpredictably and rapidly.
Many people with Alzheimer disease often have insomnia. They have trouble falling or staying asleep. Some people become confused about day and night.
At some point, psychotic behavior develops in many people with Alzheimer disease.
You May Like: Quality Of Life Alzheimer’s Disease
Total Cost Of Health Care And Long
Table reports the average annual per-person payments for health care and long-term care services for Medicare beneficiaries age 65 and older with and without Alzheimer’s or other dementias. Total per-person health care and long-term care payments in 2019 from all sources for Medicare beneficiaries with Alzheimer’s or other dementias were over three times as great as payments for other Medicare beneficiaries in the same age group .,
| Payment Source | ||
|---|---|---|
| 2,395 | ||
| TOTAL* Payments from sources do not equal total payments exactly due to the effects of population weighting. Payments for all beneficiaries with Alzheimer’s or other dementias include payments for community-dwelling and facility-dwelling beneficiaries. | 50,201 | 14,326 |
- * Payments from sources do not equal total payments exactly due to the effects of population weighting. Payments for all beneficiaries with Alzheimer’s or other dementias include payments for community-dwelling and facility-dwelling beneficiaries.
- Created from unpublished data from the Medicare Current Beneficiary Survey for 2011.
Neuronal Loss In Alzheimers Disease Brains Correlates With Dementia Not With Plaques And Tangles
Because neurons in the human cortex seem not to be significantly replaced after birth , it is conceivable that neuronal loss can lead to irreversible cognitive changes. Nevertheless, a large wealth of data has associated cognitive decline with progressive cortical mass atrophy, not necessarily linked to cell death. implicate synapse degeneration, whereas report neurofibrillary tangle accumulation. However, some studies have suggested that distribution and severity of tangle accumulation closely follows the progress of neuronal loss . Furthermore, others have attributed atrophy to a set of events besides neuronal loss, such as cell shrinkage, reduced dendritic extent, and synaptic loss .
We here report a significant reduction of neurons in the demented Alzheimers disease group in both frontal and posterior cortical regions when compared with asymptomatic subjects with Alzheimers disease. These results indicate that cognitive impairment correlates with lower neuronal numbers in the cerebral cortex, but not to amyloid- and neurofibrillary tangles, as brains from asymptomatic subjects with Alzheimers disease did not show any difference compared with control subjects. It has been proposed that the Alzheimers disease syndrome includes cognitive impairment of higher-order functions, and that a pronounced, widespread loss of cortical neurons takes place in these cases our quantitative data support this idea.
Read Also: Bob Knight Alzheimer’s