Symptoms For Dementia Sufferers
Alzheimers may also co-exist with psychotic conditions. Older adults who have schizophrenia are just as likely to develop AD as those who have no severe mental illness. They are also at a higher risk for depression, translating to a possible trifecta of co-occurring mental disorders. Symptoms of these disorders include:
- Extreme sadness
How Is Schizophrenia Treated
With early diagnosis, proper treatment and psychosocial therapy, most people with schizophrenia can lead productive and fulfilling lives. Treatment for schizophrenia may include
- Medication: Medications dont cure schizophrenia, but they help relieve the most troubling symptoms. Medications include
- Older antipsychotics such as chlorpromazine , haloperidol , etc.
- Newer antipsychotics such as risperidone , iloperidone , clozapine , etc. Clozapine is used to treat schizophrenia that is resistant to other treatments.
Schizophrenia As The Graveyard Of Neuropathologists
Many believe that schizophrenia and related disorders result from alterations in brain circuits . Yet, this probably correct assumption lacks a concrete factual demonstration hundreds of unverified neuropathological claims non-withstanding and is in stark contrast with the relative wealth of information on the neuropathology of AD because virtually nothing claimed about histopathological observations in schizophrenia has survived efforts at independent verification or corroboration. This justifies Stevens admonition about schizophrenia being the graveyard of neuropathologists , which unfortunately continues to be the case decades since its enunciation. In fact, arguably the only widely accepted, consistent morphological alterations have been found by in vivo imaging, that consist in a reduction in gray matter, enlargement of the ventricles of the brain, and focal alterations in the white matter . This is hardly specific, much less pathognomonic, and is perhaps consistent with the increasingly popular syndromatic as opposed to a unique, or sole disease view of the disorder , which would be consistent with the lack of a truly unique and unanimously agreeable cellular and molecular neuropathology. Be that as it may, it justifies the still vaguely articulated perception that schizophrenia is a disease of the cerebral cortex .
Table 1. A simplified list of selected similarities and key differences between Alzheimers disease and schizophrenia.
Read Also: Is Senility The Same As Dementia
Positive Symptoms Of Schizophrenia
In this case, the word positive doesnât mean good. It refers to added thoughts or actions that arenât based in reality. Theyâre sometimes called psychotic symptoms and can include:
- Delusions: These are false, mixed, and sometimes strange beliefs that arenât based in reality and that the person refuses to give up, even when shown the facts. For example, a person with delusions may believe that people can hear their thoughts, that they are God or the devil, or that people are putting thoughts into their head or plotting against them.
- Hallucinations: These involve sensations that arenât real. Hearing voices is the most common hallucination in people with schizophrenia. The voices may comment on the personâs behavior, insult them, or give commands. Less common types include seeing things that arenât there, smelling strange odors, having a funny taste in your mouth, and feeling sensations on your skin even though nothing is touching your body.
- Catatonia: In this condition, the person may stop speaking, and their body may be fixed in a single position for a very long time.
Causes Of Neurocognitive Disorder
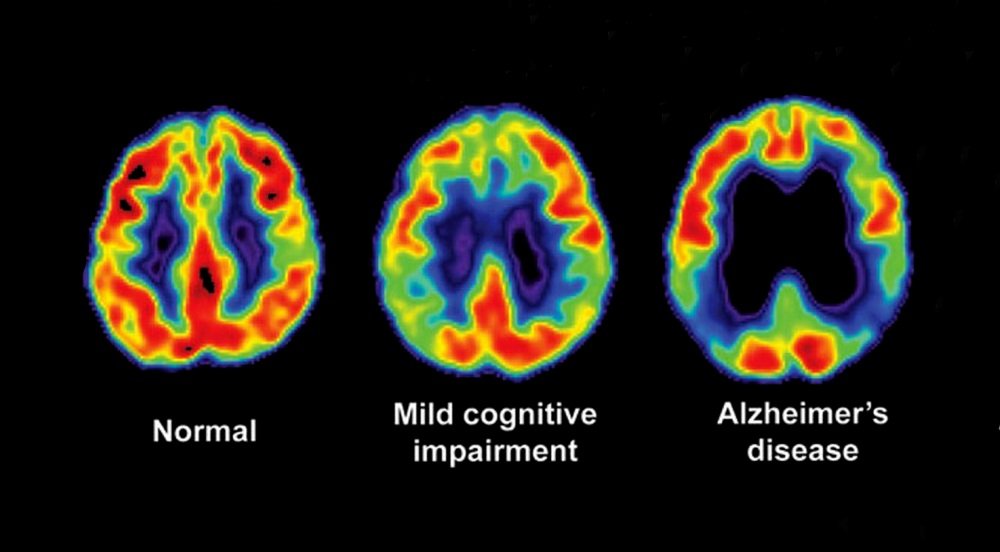
A number of underlying conditions can cause neurocognitive disorder, such as:
- Alzheimers disease. This degenerative brain condition gradually affects a persons memory, ability to think, and ability to function independently.
- Vascular dementia. A restriction in blood flow to certain regions of the brain causes a .
- Dementia with Lewy bodies. Abnormal protein deposits in nerve cells can cause neurocognitive disorder.
- Parkinsons disease. Its common for people living with this condition to develop neurocognitive disorder.
- Creutzfeldt-Jakob disease. Sometimes called mad cow disease, this very rare degenerative condition causes unique changes in brain tissue, which can cause neurocognitive disorder.
- Wernicke-Korsakoff syndrome. A brain disorder caused by severe vitamin B deficiency resulting from alcohol misuse.
The two most common causes of neurocognitive disorder are Alzheimers disease and vascular dementia.
You May Like: Dementia Ribbon Color
Prognosis Of Dementia In Schizophrenia
Dementia shortens the lifespan. At any given age, people who have dementia are two to four times more likely to die than those who do not have the disease . The median survival time of people with dementia has been investigated in cohort studies and case series in various settings, and it ranges from 3 to 9 years . However, longitudinal comparisons of the course of cognitive and functional decline have been very few in the subpopulation with dementia in schizophrenia. Reference MayerMayer found that many of Kraepelins patients with paraphrenic psychoses showed unequivocal signs of dementia later in the course of illness. Reference HoldenHolden observed that people with late paraphrenia had significantly worse outcomes when they developed dementia.
As mentioned earlier, Reference Goldberg, Hyde and KleinmanGoldberg et al stated that schizophrenia can be regarded as a static encephalopathy. Some studies suggest that the progressive cognitive decline experienced by people with poor-outcome schizophrenia is not a linear process across the lifespan, and the rate of decline may accelerate after the age of 65 .
Again, more studies are needed, on both the survival rates and prognosis of people with schizophrenia once they develop dementia .
BOX 8 Prognosis
Dementia shortens life more than schizophrenia
The median survival for people with dementia is 39 years, and it decreases significantly with age
Healthy Aging And Disease: Alzheimer’s Schizophrenia May Come From Similar Weak Spots In The Brain
The brain has a weak spot for disease, according to new research published in the Proceedings of the National Academy of Sciences.
Researchers from the University of Oxford used magnetic resonance imaging scans to observe brain structure in 484 healthy people between ages 8 and 85. This approach made it so they could study age-related changes, or patterns, in the brain. And the scans revealed a sort-of brain network within grey matter that, although it developed later than the rest of the brain, is the first to degenerate, or declinate, as people age. Grey brain matter is often referred to when discussing age-related brain degeneration, yet this study is the first to show its more vulnerable than other networks. In other words, a weak spot.
Our results show that the same specific parts of the brain not only develop more slowly, but also degenerate faster than other parts, said Dr. Gwenaëlle Douaud, lead study author of Oxford Universitys Centre for Functional Magnetic Resonance Imaging of the Brain, in a press release. These complex regions, which combine information coming from various senses, seem to be more vulnerable than the rest of the brain to both schizophrenia and Alzheimer’s, even though these two diseases have different origins and appear at very different, almost opposite, times of life.
Source: Douaud G, et al. A common brain network links development, aging, and vulnerability to disease. PNAS. 2014.
Don’t Miss: Does Alzheimer’s Cause Dementia
Patterns Of Regional White Matter Deficits In Ad Mci And Sz
Five samples were analyzed to test the above hypothesesthe ADNI samples for AD and MCI and 3 SZ samplesa discovery sample from Baltimore, MD a replication sample from Beijing, China and a replication sample from the worldwide meta-sample from ENIGMA, which is the largest white matter imaging sample in SZ. Each sample had its own healthy controls. Details on sample size, demographic , and imaging information are in the Methods section and supplementary information. White matter microstructures were measured by FA of DTI. The ranks of regional FA effect sizes between patients and controls for each cohort are shown in and supplementary table S4. In AD, the largest effect sizes were in the fornix followed by the splenium of the corpus callosum . In MCI, the largest effect sizes were in the SCC and FX . In the 3 SZ cohorts, patients showed the largest effect sizes in the anterior corona radiata , anterior limb of the internal capsule , FX, and body of the corpus callosum . The regional patient-control effect sizes in the discovery and replication cohorts were significantly correlated with those reported by ENIGMA .
Trouble Keeping A Job
Symptoms like hallucinations, delusions, and scattered thinking can make it hard to hold a job. People with schizophrenia are six to seven times more likely to be unemployed than those without this condition.
Working is important for many reasons. Not only does having a job let you support yourself, it also gives you a feeling of self-worth.
You’ll be more likely to find and keep a job if you can get on a treatment to manage your symptoms. If you already work, you may qualify for job accommodations — things that make it easier to do your work — under the Americans with Disabilities Act .
Helpful accommodations for schizophrenia include:
- A flexible schedule
- Counseling
Don’t Miss: What Color Is The Alzheimer’s Ribbon
Increased Risk Of Dementia In Individuals With Schizophrenia
The finding of no familial coaggregation between schizophrenia and Alzheimer’s dementia is conflicting with the growing body of literature emerging of an intriguing relationship between schizophrenia in the individual and the development of dementia . However, whereas most of the studies investigating coaggregation used Alzheimer’s dementia as the main outcome measure, the studies investigating schizophrenia in the individuals themselves used all-cause dementia .
The Western Mind And The Concept Of Dementia
At certain stages of civilization, each culture develops an elaborate concept of thenature of the mind and how it relates to the worlds of spirit andfleshi.e., the organs, or bodily systems, which uphold theworkings of the mind.1 The Westernconcept of the mind has its roots in Antiquity, but it was only in the XVIII centurythat it crystallized into a coherent theory.2 Accordingly, the mind is conceived as a tripartite entitycomposed of conation, cognition, and affectivity. Together, these compartmentsentail the fundamental structure of the human psyche, consisting, respectively, ofthe inclination to act upon the world , the means to attend to, store andoperate upon relevant information in the environment , and the endowment of ideational and exteroceptiveevents with personal relevance, which is typically accompanied by changes inviscero-autonomic activity . Thisconcept has explicitly-or, more often, implicitly-framed all aspects of present-dayneurological and psychiatric thought.
You May Like: Can Dehydration Cause Anxiety Attacks
Don’t Miss: Difference Between Dementia And Senility
Cognitive Impairment In Schizophrenia
A number of meta-analyses have examined the extent of cognitive impairment in people with schizophrenia . Large effect sizes , representing robust evidence of impairment, have been reported across a multitude of cognitive domains, including current IQ, category fluency, verbal memory, abstract thinking, language, sustained attention and response inhibition. Symbol coding tasks yielded some of the most robust evidence, with very large effect sizes. However, Reference Hyde, Nawroz and GoldbergHyde et al performed a cross-sectional study to assess cognitive performance in schizophrenia across a wide age range. A comparison of scores on cognitive measures recorded for five age-derived cohorts showed no evidence of accelerated decline on the Mini-Mental State Examination , the Dementia Rating Scale, list learning, semantic fluency or perseverative errors on the Wisconsin Card Sorting Test.
Does Schizophrenia Get Worse As You Age
For some people, schizophrenia symptoms and episodes may grow worse with time or age, particularly if they avoid treatment or professional help. However, when schizophrenia manifests at a younger age, symptoms and behavior are generally more extreme than with later-onset schizophrenia. That means if schizophrenia symptoms develop later in life, theyre generally less severe than when they develop at a younger age.
The most important thing to remember is that schizophrenia doesnt necessarily get worse with age. Preliminary research has found that individuals living with schizophrenia dont experience cognitive decline any faster than the general population. Psychosocial function may even improve with age, and most individuals experience improved quality of life as they grow older.
For people committed to recovery and following a medication regimen, a long-term balanced lifestyle is possible with preventative treatment, even as they grow older.
Are you or someone you care about struggling with symptoms of schizophrenia? Find out if PCH is the right place to find the help and hope youre looking for. Is PCH Right for You?
Also Check: Alzheimer’s Aphasia
More Than A Quarter Had A Dementia Diagnosis By Age 66
byKara Grant, Enterprise & Investigative Writer, MedPage Today March 10, 2021
Prevalence of dementia by the time of Medicare eligibility was significantly elevated among individuals with schizophrenia, a retrospective cohort study found.
Using data from a national sample of Medicare recipients, the prevalence of diagnosed dementia by age 66 was 25 times greater for patients with schizophrenia, at 27.9% versus 1.3% in individuals without a history of serious mental illness , reported T. Scott Stroup, MD, MPH, of Columbia University in New York City, and colleagues.
By age 80, prevalence in these groups increased to 70.2% and 11.3%, respectively, according to the findings in JAMA Psychiatry.
In those without a prior history of dementia, the annual incidence of dementia diagnoses at age 66 was 52.5 per 1,000 person-years among the schizophrenia group, but only 4.5 per 1,000 person-years among those without a past SMI. By 80, incidence of dementia diagnosis increased to 216.2 per 1,000 person-years for those with schizophrenia and to 32.3 per 1,000 person-years for the comparator group.
“When aging and other risk factors for dementia start accumulating, might cross a threshold for dementia diagnosis much sooner,” Stroup told MedPage Today.
Stroup’s group acknowledged that the study’s most significant limitation was that clinical diagnoses could not be individually confirmed or validated.
Disclosures
Primary Source
JAMA Psychiatry
Signs And Symptoms Of Paranoid Schizophrenia
Signs and symptoms of paranoid schizophrenia include:
- Auditory hallucinations hearing things that are not there
- Delusions false beliefs
- Anxiety this may appear in periods of high levels of anxiety
- Anger may start mild but range in severity. Anger can raise blood pressure, heart rate, and adrenaline.
- Detachment either physically or emotionally detached from others
- Aggression and violence aggression may contribute to violent outbursts
- Quarrels
- Condescension patient may believe they know stuff that others do not, so they come off as patronizing
- Suicidal thoughts and behavior patient may say phrases such as I wish I was never born, or go out of their way to find weapons or pills to kill themselves with. Early warning signs of suicide include social withdrawal, mood swings, obsession with dying or violence, feeling trapped or desperate, illicit drug usage, changes in eating or sleeping patterns, getting ones affairs in order, and saying goodbye to people in a specific way.
You May Like: Does Celine Dion Have An Eating Disorder
Recommended Reading: Does Diet Coke Cause Memory Loss
Protein Linked To Alzheimers May Also Play A Role In Schizophrenia
A specific protein implicated in the cognitive decline of Alzheimers disease also appears to play a role in genetic predisposition to schizophrenia, meaning that a drug that targets that protein could treat a variety of neuropsychiatric disorders, according to a new study published October 18 in the journal Molecular Psychiatry.
Yale researchers have been studying the role that the STEP protein plays in healthy functioning of synapses the connections between brain cells. Excessive amounts of STEP protein are found in the brains of humans and animal models of Alzheimers disease, Parkinsons disease, fragile X syndrome, and schizophrenia. The increase in STEP leads to a disruption of synaptic function and contributes to the cognitive deficits present in these disorders.
The research was led by Yales Paul Lombroso, the Elizabeth Mears and House Jameson Professor in the Child Study Center and professor of neurobiology and psychiatry, and Kristen Brennand at the Icahn School of Medicine at Mount Sinai.
While the drug used in the earlier Alzheimers experiments has proven difficult to develop for clinical use, Lombroso said he and colleagues at Yale are developing new STEP inhibitors and, if successful, these may have more practical therapeutic value.
These findings suggest that a STEP inhibitor, when discovered, may be the basis of a new drug that can treat a number of neuropsychiatric disorders, Lombroso said.
Related
Replication Of Elevated White Matter Rvi
The ENIGMA SZ pattern of regional white matter deficits was significantly correlated with the pattern for white matter deficits in AD . The RVI-AD and RVI-SZ in SZ patients were highly correlated . Therefore, despite the very different age ranges, etiologies, and neuropathologies, the white matter deficit patterns in SZ patients showed significantly elevated similarity to white matter deficit patterns observed in AD patients across the samples.
On white matter tract level : A. Significant correlation of regional deficit patterns across the 22 major white matter tracts for Alzheimers disease and schizophrenia . B. No such correlation was observed between MCI and SZ. Similarly, on individual SZ patient level : C. regional vulnerability index for AD and RVI for SZ showed a robust correlation in SZ patients D: correlation between RVI for MCI and RVI for SZ in SZ patients. Note: MCI, mild cognitive impairment.
You May Like: Where To Buy Jelly Drops For Dementia Patients
Frontotemporal Dementia Manifested As Schizophrenia With Decreased Heterochromatin On Chromosome 1
Philippos Gourzis
1Department of Psychiatry, School of Medicine and University Hospital of Patras, University of Patras, 26504 Rio, Patras, Greece
2Department of Neurology, School of Medicine and University Hospital of Patras, University of Patras, 26504 Rio, Patras, Greece
3Department of Chemistry, Laboratory of Biochemistry, University of Patras, 26504 Rio, Patras, Greece
4Department of Genetics, Alexandra Hospital, 10671 Athens, Greece
Academic Editor:
Abstract
1. Introduction
Frontotemporal dementia is a mainly presenile degenerative disorder marked by progressive behavioural changes and cognitive impairment, characterized by progressive atrophy of both frontal and anterior temporal lobes . The disease has now been proved as the second most common type of presenile dementia, with a correlation ratio of about one case of FTD to four of Alzheimers disease . An autosomal dominant pattern of inheritance is found in 1027% of all FTD patients , with several genetic defects identified in some, but not all, hereditary cases of FTD .
Differentiation between FTD, primary psychiatric disorders, AD, and other dementias is crucial for case management and determining prognosis. Identification of factors relating to etiology, age of onset, and clinical presentation of FTD could help expand our understanding of the pathogenesis of the disorder, and probably enhance accurate clinical diagnosis .
2. Case Presentation