Quantitative Analysis Of Putative Biomarkers In The Csf And The Serum
Among the 13 putative proteins of interest identified in the CSF, 10 of them were subsequently analyzed through quantitative method in the CSF and the serum of AD and control patients. This quantification was performed on an enlarged cohort, composed of 55 individuals , characterized clinically and biologically for CSF biomarkers: A42, tau, and p-tau . According to their clinical diagnosis, AD patients showed a decrease of CSF A142, together with an increase of CSF tau and p-tau . The ratio IATI was calculated for these patients and allowed for diagnostic discrimination of the two groups . Groups were homogeneous in terms of age, sex repartition, CRP, and CSF protein, and MMSE was decreased in AD group .
Figure 3. Clinical biochemical characterization of patients. The 55 patients of the enlarged cohort used for the second part of the study were characterized clinically and quantified for CSF biomarkers: A42, tau, and p-tau, using Fujirebio ELISA quantification kits . IATI ratio was calculated for every subject of the cohort. Outliers are indicated with black circle. Outliers are defined as a value that is smaller than the lower quartile minus three times the interquartile range, or larger than the upper quartile plus three times the interquartile range.
Table 2. CSF and serum quantification of predictors identified.
Rarer Causes Of Dementia
There are many rarer diseases and conditions that can lead to dementia, or dementia-like symptoms.
These conditions account for only 5% of dementia cases in the UK.
They include:
- problems with planning and reasoning
These symptoms are not severe enough to cause problems in everyday life.
MCI can be caused by an underlying illness, such as depression, anxiety or thyroid problems.
If the underlying illness is treated or managed, symptoms of MCI often disappear and cause no further problems.
But in some cases, people with MCI are at increased risk of going on to develop dementia, which is usually caused by Alzheimer’s disease.
Read more about how to prevent dementia.
Early Onset Alzheimers Disease
Although age is the main risk factor for Alzheimers disease, this is not just a condition that affects older adults.
According to the Alzheimers Association, early onset Alzheimers disease affects around 200,000 U.S. adults under the age of 65 years. Many people with this condition are in their 40s or 50s.
In many cases, doctors do not know why younger people develop this condition. Several rare genes can cause the condition. When there is a genetic cause, it is known as familial Alzheimers disease.
Recommended Reading: Senile Dementia Of The Alzheimer Type
You May Like: Pathophysiology Of Dementia Disease
Safety And Supportive Measures
Creating a safe and supportive environment can be very helpful.
Generally, the environment should be bright, cheerful, safe, stable, and designed to help with orientation. Some stimulation, such as a radio or television, is helpful, but excessive stimulation should be avoided.
Structure and routine help people with Alzheimer disease stay oriented and give them a sense of security and stability. Any change in surroundings, routines, or caregivers should be explained to people clearly and simply.
Following a daily routine for tasks such as bathing, eating, and sleeping helps people with Alzheimer disease remember. Following a regular routine at bedtime may help them sleep better.
Activities scheduled on a regular basis can help people feel independent and needed by focusing their attention on pleasurable or useful tasks. Such activities should include physical and mental activities. Activities should be broken down in small parts or simplified as the dementia worsens.
Anxiety Depression And Stress Post
The outbreak of COVID-19 is stressful for many people. People respond to stress in different ways and it is normal to experience a range of emotions, including fear, anxiety, and grief. Being isolated from others during the infection, the real risk of death, and the stress of hospitalization and critical care can trigger post-traumatic stress disorder. In addition, given the contagious nature of COVID-19, the individual is often not the only affected person in the family or circle of friends, some of whom may even have died. Some people may develop a mood or anxiety disorder. For information on post-COVID stress and coping, see the National Institute of Mental Healths resources at National Institute of Mental Health’s Director, Dr. Gordon In the News and NIMH Shareable Resources on Coping with COVID-19.
Read Also: Shampoos That Cause Alzheimer’s
So How Can Dementia Lead To Loss Of Movement
Dementia is not a disease in itself, more a collective term for a range of problems that gradually affect the brains ability to function as it once did. And that includes its ability to manage critical neurological functions of the body one of which is being able to move.
Depending on the type of degenerative condition someone is experiencing, damage caused to the brain happens in different ways. For people living with vascular and frontotemporal dementia, experts agree that muscle weakness and limb paralysis is often due to a series of mini, or large strokes in the brain. Both of these can massively impair someone with a range of physical as well as cognitive damage.
DID YOU KNOW? Doctors used to think that stroke and dementia were unrelated. But research has gone on to reveal that the two are very interlinked.
Quantitative Analysis Through Elisa And Electrochemiluminescence Assays
Quantitative multiplex or simplex methods were performed in both the CSF and serum of 55 patients , using either electrochemiluminescence or ELISA method. Quantification of FABP3, TIMP-1, MIP-1beta, and RANTES was performed using simplex detection MSD kit, while GRO-alpha, IL-8, MCP-1, MIP-3beta, and sTNFR-I were simultaneously measured using MSD custom V-Plex detection . Quantification of IGFBP-6, sIL-6R, IL-3, and MIP-1alpha was performed through simplex ELISA, purchased from Clinisciences. CSF samples were measured directly, without previous dilution. Depending on the cytokine measured, serum samples were diluted .
Also Check: Are Jigsaw Puzzles Good For Dementia
Ad Diagnosis And Cognitive Assessments
The diagnosis of MCI or mild dementia of AD type was based on neuropsychological and clinical evaluation made by a consensus conference of neuropsychologists, psychiatrists, and/or neurologists prior to inclusion into the study, as described elsewhere and detailed in Additional file : methods together with the performed cognitive assessments.
What Medications Are Available To Treat Dementia
Drugs approved for the most common form of dementia, Alzheimers disease, are discussed below. These drugs are also used to treat people with some of the other forms of dementia.
- cholinesterase inhibitors
- NMDA receptor antagonist memantine
These two classes of drugs affect different chemical processes in the brain. Both classes have been shown to provide some benefit in improving or stabilizing memory function in some patients. Although none of these drugs appear to stop the progression of the underlying disease, they may slow it down.
If other medical conditions are causing dementia or co-exist with dementia, the appropriate drugs used to treat those specific conditions are prescribed.
Also Check: Which Neurotransmitter Is Associated With Alzheimer’s
Acetylcholine Release And Inactivation
When cholinergic neurons are depolarized, ACh is exocytosed from synaptic vesicles and released into the synaptic cleft, where it can activate both muscarinic and nicotinic receptors. ACh present at the synaptic cleft is rapidly inactivated by the enzyme acetylcholinesterase , releasing choline and acetate . Cholinergic neurons secrete AChE into the synaptic cleft, where the enzyme is normally associated with the plasma membrane . Neurotransmitters other than ACh are normally reuptaken into the presynaptic neuron and then inactivated by specific enzymes. Thus, the mechanism of ACh inactivation is unique. Each molecule of AChE can hydrolyze 5000 molecules of ACh per second, which makes AChE one of the most kinetically efficient enzymes known . It has been demonstrated that AChE, in addition to metabolizing ACh, has a number of non-classical actions. For a review on non-classical actions of AChE, see .
AChE gene can generate multiple protein products due to mRNA splicing . These distinct transcripts exhibit unique expression in the various tissues, as well as different patterns of plasma membrane association . The main AChE transcript is expressed in muscles and brain. Other transcripts of AChE are expressed in developing blood cells .
You May Like: What Color Ribbon Is For Dementia
Bleeding In The Brain Weakened Blood Vessels And Blood Clots In Acute Infection
The SARS-CoV-2 virus attaches to a specific molecule on the surface of cells in the body. This molecule is concentrated in the lung cells but is also present on certain cells that line blood vessels in the body. The infection causes some arteries and veinsincluding those in the brainto become thin, weaken, and leak. Breaks in small blood vessels have caused bleeding in the brain in some people with COVID-19 infection. Studies in people who have died due to COVID-19 infection show leaky blood vessels in different areas of the brain that allow water and a host of other molecules as well as blood cells that are normally excluded from the brain to move from the blood stream into the brain. This leak, as well as the resulting inflammation around blood vessels, can cause multiple small areas of damage. COVID-19 also causes blood cells to clump and form clots in arteries and veins throughout the body. These blockages reduce or block the flow of blood, oxygen, and nutrients that cells need to function and can lead to a stroke or heart attack.
A stroke is a sudden interruption of continuous blood flow to the brain. A stroke occurs either when a blood vessel in the brain becomes blocked or narrowed or when a blood vessel bursts and spills blood into the brain. Strokes can damage brain cells and cause permanent disability. The blood clots and vascular damage from COVID-19 can cause strokes even in young healthy adults who do not have the common risk factors for stroke.
Also Check: Alzheimer’s Ribbon Color
What Are Possible Long
Researchers are following some known acute effects of the virus to determine their relationship to the post-acute complications of COVID-19 infection. These post-acute effects usually include fatigue in combination with a series of other symptoms. These may include trouble with concentration and memory, sleep disorders, fluctuating heart rate and alternating sense of feeling hot or cold, cough, shortness of breath, problems with sleep, inability to exercise to previous normal levels, feeling sick for a day or two after exercising , and pain in muscle, joints, and chest. It is not yet known how the infection leads to these persistent symptoms and why in some individuals and not others.
Zinc Finger Transcription Factors And Gene Regulation
Zinc is responsible for the DNA-binding ability of many transcription factors through a unique ability to form molecules known as zinc finger proteins. These ubiquitously expressed proteins directly regulate gene expression. They also appear to interface with RNA and function to facilitate protein-protein interactions. While several classes of ZnF proteins are known to exist, by far the most common form is the classical ZnF, consisting of 2 cysteine and 2 histidine or 1 cysteine and 3 histidine residues centralized around a zinc ion with a short b-hairpin and an a-helix incorporated into the structure. The conformation of ZnFs centers around the coordinated zinc ion and provides the molecule with the potential to form a finger-like structure that is capable of binding tightly with specific DNA sequence domains .
Other zinc finger transcription factors that are clearly involved in neuronal function include the thyroid hormone receptor that plays a role in neuronal growth and development, and both retinoic acid receptors and vitamin D receptors that participate in neuronal differentiation.
Also Check: What Color Is Alzheimers Ribbon
Don’t Miss: Did Margaret Thatcher Have Dementia
Pharmacological Effects Of Niacin
When supplemented at physiological amounts, nicotinic acid and nicotinammide are effective in treating traditional pellagra nonetheless, at higher concentrations, they display separate additional pharmacological activities, ranging from anti-dyslipidemic to anti-inflammatory action. The first evidence of lipid-altering effects of niacin dates back to 1955, when Altschul and co-workers reported the ability of 3000 mg/day nicotinic acid to reduce serum cholesterol in humans . An every growing body of experimental data points to beneficial effects of nicotinic acid as an anti-hyperlipidemic agent. It is now well established that nicotinic acid efficaciously: inhibits free fatty acid mobilization and lipolysis reduces hepatic triglyceride synthesis and very low density lipoprotein secretion inhibits VLDL conversion into low density lipoprotein increases serum high-density-lipoprotein levels triggers LDL conversion from small, dense particles to large, low density particles, reduces serum lipoprotein concentrations and increases apolipoprotein A1 .
In vitro and in vivo studies have also demonstrated that nicotinic acid exerts significant anti-inflammatory, anti-oxidant and anti-apoptotic activities in a variety of cells and tissues , thus being potentially beneficial for the management of several pathological conditions, including type-2 diabetes , obesity , atherosclerosis , kidney and lung injury , and hyperalgesia .
Acetylcholine Storage In Vesicles
ACh that is synthesized in the cytoplasm of cholinergic neurons is transported into synaptic vesicles by VAChT, which is located in the synaptic vesicle membrane . The gene encoding VAChT has been cloned and hydrophobic analysis indicates that the protein has twelve transmembrane domains . Each molecule of ACh transported by VAChT is in exchange for two vesicular protons, which leads to the fulfill of synaptic vesicles with the neurotransmitter . The vesicular transporter activity can be blocked by vesamicol, which is a non-competitive inhibitor .
VAChT carboxyl-terminus has many motifs important for cellular trafficking and for its localization to synaptic vesicle membranes . Interestingly, PKC can phosphorylate VAChT and regulate its vesicular localization . A VAChT knockdown mouse model, expressing about 68% less VAChT protein, shows major neuromuscular deficits. This data highlights the importance of the transporter to the peripheral nervous system. Furthermore, cognitive impairment can take place even due to a mild decrease in VAChT protein expression .
Also Check: Difference Between Senility And Dementia
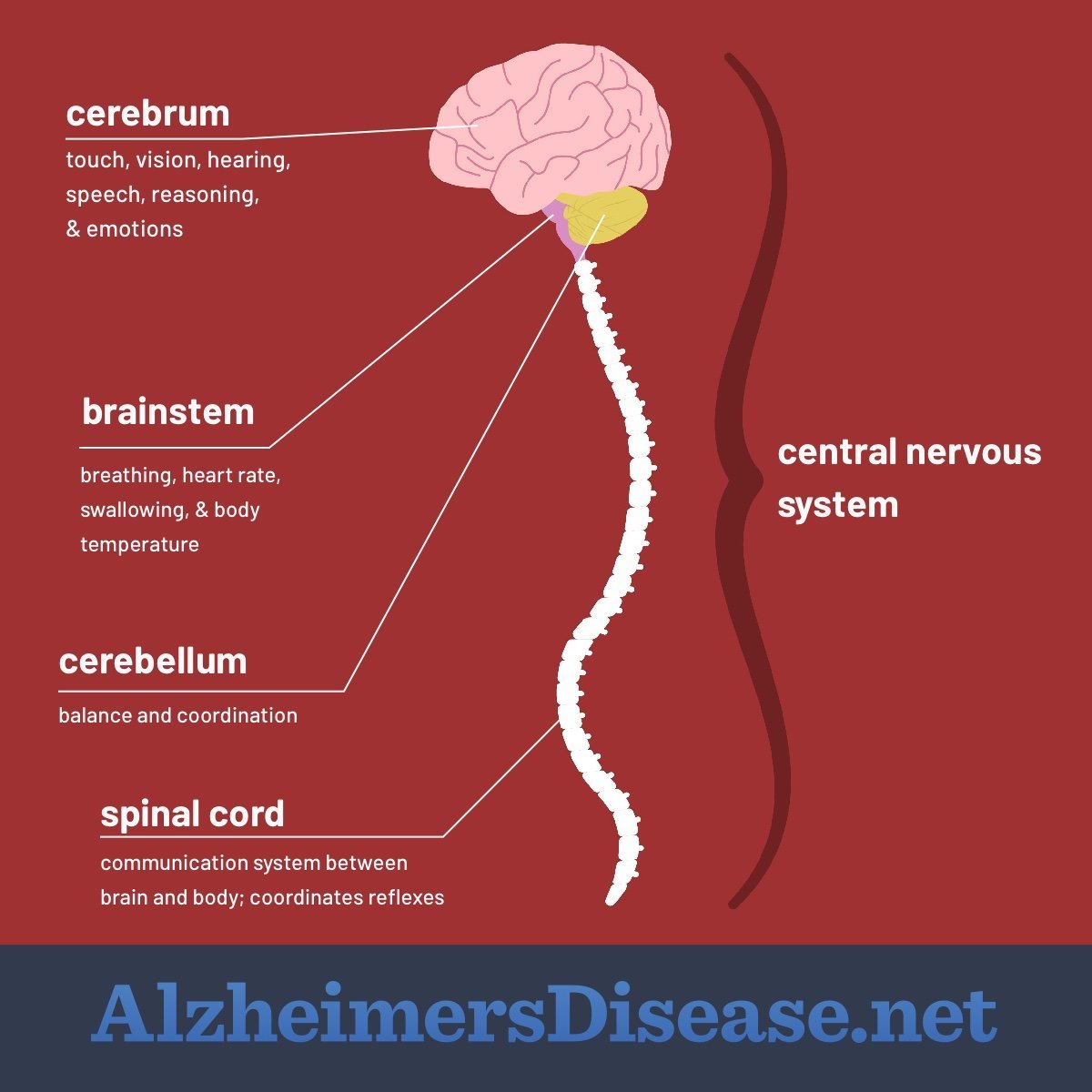
What Is The Central Nervous System
The central nervous system is made up of the brain and spinal cord. It is one of 2 parts of the nervous system. The other part is the peripheral nervous system, which consists of nerves that connect the brain and spinal cord to the rest of the body.
The central nervous system is the bodys processing centre. The brain controls most of the functions of the body, including awareness, movement, thinking, speech, and the 5 senses of seeing, hearing, feeling, tasting and smelling.
The spinal cord is an extension of the brain. It carries messages to and from the brain via the network of peripheral nerves connected to it.
Nerves also connect the spinal cord to a part of the brain called the brainstem.
What Is The Typical Recovery From Covid
Fortunately, people who have mild to moderate symptoms typically recover in a few days or weeks. However, some people who have had only mild or moderate symptoms of COVID-19 continue to experience dysfunction of body systemsparticularly in the lungs but also possibly affecting the liver, kidneys, heart, skin, and brain and nervous systemmonths after their infection. In rare cases, some individuals may develop new symptoms that stem from but were not present at the time of initial infection. People who require intensive care for Acute Respiratory Distress Syndrome, regardless of the cause, usually have a long period of recovery. Individuals with long-term effects, whether following mild or more severe COVID-19, have in some cases self-identified as having long COVID or long haul COVID. These long-term symptoms are included in the scientific term, Post Acute Sequelae of SARS-CoV-2 Infection .
Recommended Reading: Dementia Vs Senility
How Is Alzheimers Different From Other Forms Of Dementia
Alzheimers disease is distinguished from other forms of dementia by characteristic changes in the brain that are visible only upon microscopic examination during autopsy. Brains affected by Alzheimers disease often show presence of the following:
-
Fiber tangles within nerve cells
-
Clusters of degenerating nerve endings
Another characteristic of Alzheimers disease is the reduced production of certain brain chemicals necessary for communication between nerve cells, especially acetylcholine, as well as norepinephrine, serotonin, and somatostatin.
Read Also: Which Neurotransmitter Is Associated With Alzheimers
Behavior Disorders In Alzheimer Disease
Because people are less capable of controlling their behavior, they sometimes act inappropriately or disruptively . These actions are called behavior disorders.
Several effects of Alzheimer disease contribute to this behavior:
-
Because people with Alzheimer disease have forgotten the rules of proper behavior, they may act in socially inappropriate ways. When hot, they may undress in public. When they have sexual impulses, they may masturbate in public, use off-color or lewd language, or make sexual demands.
-
Because they have difficulty understanding what they see and hear, they may misinterpret an offer of help as a threat and may lash out. For example, when someone tries to help them undress, they may interpret it as an attack and try to protect themselves, sometimes by hitting.
-
Because their short-term memory is impaired, they cannot remember what they are told or have done. They repeat questions and conversations, demand constant attention, or ask for things they have already received. They may become agitated and upset when they do not get what they ask for.
-
Because they cannot express their needs clearly or at all, they may yell when in pain or wander when lonely or frightened. They may wander, yell, or call out when they cannot sleep.
Whether a particular behavior is considered disruptive depends on many factors, including how tolerant the caregiver is and what sort of situation the person with Alzheimer disease is living in.
Also Check: Etiology Of Alzheimers
How Does Smoking Affect The Nervous System
inaddictionaddictive disordersmental health issuesmind and brainnervous systemNeuroscience
Most peopleunderstand how smoking affects the lungs and heart, but what is less known isthe negative effect of smoking on the nervous system and brain.
In this article, we willdiscuss the effects of smoking on your nervous system as well as the benefitsof quitting smoking.
| How Does Smoking Affect the Brain? |