What Makes Dementia Different From Mental Illnesses
Mental disorders and dementia may look similar, but they have distinct characteristics. For example, schizophrenia and bipolar disorder can mimic dementia symptoms. Similarly, Alzheimers disease or other forms of dementia may be mistaken for a mental illness. It is for this reason that a physicians diagnosis is so important.
Dementia refers to a range of cognitive decline in some individuals caused by aging. We can associate a wide range of symptoms with this term, from minor difficulties to severe impairments. There are over 5 million people with Alzheimers disease in the United States.Some of the most common dementia symptoms are:
- Loss of memory
- Challenges in proper public behavior
Dont Mental Illnesses Also Affect Our Brains
Researchers believe individuals with mental illnesses, including schizophrenia, may experience disruptions in neurotransmitters such as dopamine, norepinephrine, and glutamate. Cocaine addicts sometimes exhibit symptoms like schizophrenia, suggesting that dopamine plays a crucial role in schizophrenia.
Scientists link mental illness to problems with how neurons communicate in the brain . They, for example, associate depression with a decrease in serotonin level, and they base several psychiatric medications on this finding. Besides serotonin changes, there can be changes in other neurotransmitters in depression, thus complicating the cause of the mental condition.
Researchers are using multidisciplinary research to understand mental illness. Psychology, neuroscience, and psychiatry all investigate different aspects of the connection between the biology of the brain and mental illness.
Did You Know Dementia Is A Mental Illness
- 9:35 pm
This post was provided by our partners at Second Wind Dreams. I hesitated at first when I read it, but she makes some great points that the aging community, doctors, and practitioners should take into consideration.
Words matter and, in the same way, the diagnostic classification does too.
According to the Diagnostic and Statistical Manual, used by clinicians to diagnose people with mental illness, dementia and the different types of dementia are listed there. In the latest DSM-5, the term dementia is replaced with neurocognitive disorder. Thank goodness for that because the word dementia is derived from a Latin word meaning mad or insane. The change to neurocognitive disorderis an effort to distance the condition from any stigma attached to the word dementia. Really?
According to experts, dementia is expected to remain in common use as it is widely understood . Some may say that diagnostic classification really doesnt matter but being categorized as a mental illness has resulted in deep-seated misperceptions of the disease.
Insurance coverage has always lagged for people with mental illness and once again, dementia is collateral damage in this case. Yet, it costs more to care for a person with dementia than it does to care for an older adult with a chronic disease. Reimbursement for the care of a person with dementia continues to lag behind hurting everyone from caregivers and the person with dementia.
Recommended Reading: Senility Vs Dementia Vs Alzheimer’s
Mental Illness Vs Dementia In The Elderly
When people think of dementia, its common to think of it as a mental illness due to the effects the condition has on the brain. However, there are distinctions that should be made between dementia and mental illness in order to properly diagnose the individual. While dementia does affect mental health, it is not a mental illness, but a disorder of the brain that causes memory loss and trouble with communicating.
Proper diagnosis of mental illness or dementia in the elderly is vital in order ensure that appropriate treatment is provided as soon as possible. Misdiagnosis of mental illness in seniors can occur easily since symptoms are so similar to dementia, like confusion and erratic behavior.
In Addition To The Aforementioned Causes Of Reversible Or Pseudo

These include:
- Older age more so for many people above the age of 65. Even still, dementia is not considered normal at any age, and it can present in people well before they hit 65.
- A family history of dementia It doesnt automatically mean someone will get it. In contrast, there are people who develop dementia when there is no family history of the condition.
- Downs syndrome aging combined with the syndrome often results in many developing a form of dementia that is, or is like, Alzheimers by middle age.
- Heavy alcohol use defined by the National Institute on Alcohol Abuse as consuming 4 or more drinks per day for men, and 3 or more per day for women.
- Cardiovascular issues including high cholesterol and blood pressure. These risks can often be reduced with a healthy diet and regular exercise.
- Untreated depression risk can be reduced by working with a mental health professional to treat the depression.
- Obstructive sleep apnea a treatable condition.
- Smoking
Also Check: Alzheimers Awareness Ribbons
How The Dsm Is Used
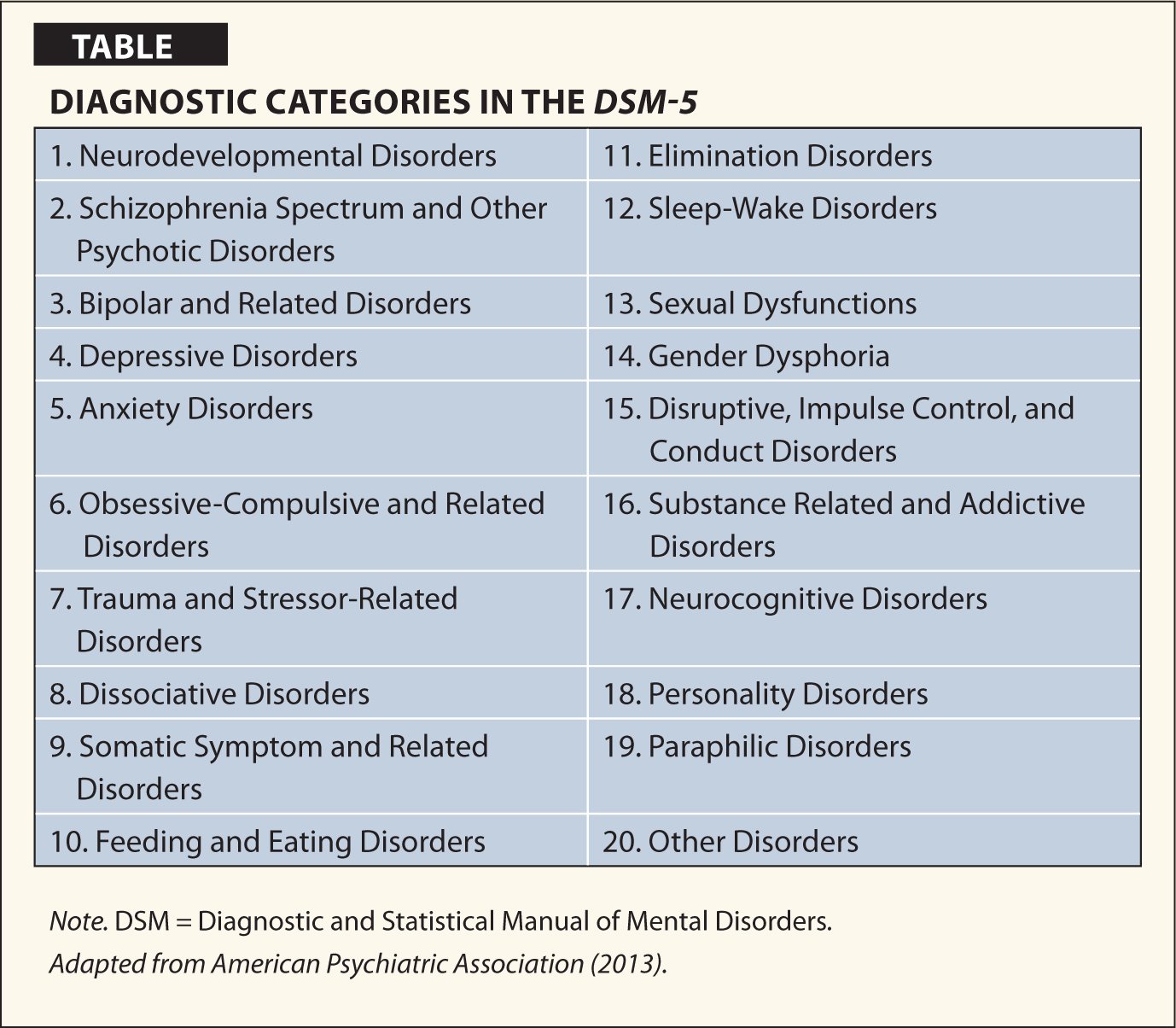
The DSM features descriptions of mental health conditions ranging from anxiety and mood disorders to substance-related and personality disorders, dividing them into categories such as major depressive disorder, generalized anxiety disorder, and narcissisticpersonality disorder. These disorders are grouped into chapters based on shared features, e.g., Feeding and Eating Disorders Depressive Disorders Schizophrenia Spectrum and Other Psychotic Disorders.
For each disorder category, the manual includes a set of diagnostic criterialists of symptoms and guidelines that psychiatrists, psychotherapists, and other health professionals use to determine whether a patient or client meets the criteria for one or more diagnostic categories. For diagnosis of major depressive disorder, for example, the current DSM states that a person shows at least five of a list of nine symptoms within the same two-week period. It also requires that the symptoms cause clinically significant distress or impairment in social, occupational, or other important areas of functioning, along with other stipulations.
Updates to these diagnostic categories and criteria are made through a years-long research and revision process that involves groups of experts focusing on distinct areas of the manual.
Mental Illness And Dementia: Similarities And Differences
In many ways, mental illness can manifest the same symptoms of dementia, and vice versa. While there are a lot of similarities between the two, there are also some pretty critical differences. If you have a loved one in hospice in San Francisco and elsewhere who is suffering from one of the two, youll want to read on. To recognize Mental Illness Awareness Week , we will use this blog to explain the similarities and differences between mental illness and dementia.
Each year, millions of Americans live with a mental health condition, but its important to remember that mental illness affects everyone either in a direct or indirect way through friends, family or coworkers, according to the National Alliance on Mental Illness . Despite the reach and prevalence of mental illness, though, stigma and misunderstanding are still widespread. Couple that misunderstanding with the fact that mental illness can imitate the symptoms of dementia, and vice versa, and you have a serious, pervasive problem in this country.
Also Check: Can Prevagen Help Dementia
Changes Introduced By Dsm
The Diagnostic and Statistical Manual of Mental Disorder, Fifth Edition , contains revisions of the diagnostic criteria and nomenclature for dementia and other cognitive disorders. The name of the diagnostic category has been changed the section entitled delirium, dementia and amnestic and other cognitive disorders in the fourth edition and subsequent text revision is now neurocognitive disorders, or NCDs. The dementias, if the clinician prefers, can still be referred to by their traditional names . All the diagnostic entities found in the prior section are subsumed under the new NCD rubric, and therefore cognitive impairments that are not severe enough to qualify for a diagnosis of dementia are now also defined as belonging to the category of NCDs. They are no longer referred to by the descriptor not otherwise specified found in DSM-IV.
Under the previous classification system, cognitive impairments not meeting the criteria for dementia were labeled cognitive disorder NOS, or perhaps age-related cognitive decline. The non-DSM term mild cognitive impairment has also been in widespread use in the elderly population, despite its limited clinical value. Patients identified as having MCI are known to progress to dementia at a higher rate than age-matched patients without MCI, but there are currently no therapeutic interventions to delay or prevent progression, nor are there any reliable predictors of which patients with MCI will develop dementia.
Application Of Dementia/ncd Diagnostic Criteria
Data were collected as part of the LonDownS study of people with DS over the age of 16 living in England and Wales using a validated assessment. The full battery has been published elsewhere and includes a mixture of direct and informant measures of cognition and adaptive abilities as well as demographic and physical health data.
One-hundred and sixty-five participants were selected from the older adult LonDownS cohort by the study co-ordinator using stratified random sampling to ensure a mix of ages and clinical dementia status. Data from the younger adult cohort were not used in this study due to the low prevalence of dementia in people with DS before 35: the average age of dementia diagnosis in DS is currently around 55 years old. Diagnosis of DS was confirmed genetically using saliva or blood samples. Pre-existing dementia diagnosis was based on the medical history provided during the assessment.
Fifty-three participants had existing clinical diagnoses of dementia, 69 were female, 151 were of white ethnicity, 41 were APO4 carriers. Further demographic data is available in Table .
Table 1 Demographic data.
Read Also: Karen Vieth Edgar Knight
Neurocognitive Disorders Due To Parkinsons Disease
These disorders are diagnosed when there is gradual cognitive decline in thepresence of a well-established diagnosis of Parkinsons disease. Over thecourse of their disease, approximately 75% of individuals withParkinsons disease will develop a major neurocognitive disorder. The pattern of cognitive deficits isvariable but often affects the executive, memory, and visuospatial domains, with aslowing of information processing that suggests a subcorticalpicture. Associated features include psychiatric symptoms such as depressed oranxious mood, apathy, hallucinations, delusions, or personality change, as well asrapid eye movement sleep behavior disorder and excessive daytimesleepiness.
Medicalization And Financial Conflicts Of Interest
There was extensive analysis and comment on DSM-IV in the years leading up to the 2013 publication of DSM-5. It was alleged that the way the categories of DSM-IV were structured, as well as the substantial expansion of the number of categories within it, represented increasing medicalization of human nature, very possibly attributable to disease mongering by psychiatrists and pharmaceutical companies, the power and influence of the latter having grown dramatically in recent decades. In 2005, then APA President Steven Sharfstein released a statement in which he conceded that psychiatrists had “allowed the biopsychosocial model to become the bio-bio-bio model”. It was reported that of the authors who selected and defined the DSM-IV psychiatric disorders, roughly half had financial relationships with the pharmaceutical industry during the period 1989â2004, raising the prospect of a direct conflict of interest. The same article concluded that the connections between panel members and the drug companies were particularly strong involving those diagnoses where drugs are the first line of treatment, such as schizophrenia and mood disorders, where 100% of the panel members had financial ties with the pharmaceutical industry.
Recommended Reading: Alzheimer Ribbon
Is There Anything You Can Do To Help A Person With Dementia
Its natural to feel irritated the tenth time you answer a question, but people with dementia pick up on your feeling and absorb it. Communicate in a calm, reassuring way to dementia patients. Create distractions with fun activities they enjoy.
Dementia will bring losses and changes to everyone you love, but you do not have to bear them alone: get friends and family to help. Stay present and take joy in every moment. But more important is seeking professional help.
Our therapists can offer several options to assist with dementia. We offer you suggestions on how to improve the symptoms to lead a healthy life. Contact us today.
Cognitive Mental Disorder Perspective
In abnormal psychology, cognitive disorders are mental disorders that develop on the basis of cognitive mental disorder perspective. The cognitive mental disorder perspective is the theory that psychological disorders originate from an interruption, whether short or long, in our basic cognitive functions, i.e. memory processing, perception, problem solving and language. This perspective takes opposition to the psychodynamic mental disorder perspective, behavioral mental disorder perspective, sociocultural mental disorder perspective, interpersonal mental disorder perspective and neurological/biological mental disorder perspective. One pioneer of cognitive disorder perspective is Albert Ellis. In 1962, Ellis proposed that humans develop irrational beliefs/goals about the world and therefore, create disorders in cognitive abilities. Another pioneer of the cognitive disorder perspective is Aaron Beck. In 1967, Beck designed what is known as the “cognitive model” for emotional disorders, mainly depression. His model showed that a blending of negative cognitive functions about the self, the world, and possible selves lead to cognitive mental disorders.
Recommended Reading: Does Prevagen Help Dementia
The Gold Standard Of Brain Supplementation
Memory Health® was tested and proven in double-blind, placebo-controlled clinical trials, becoming the first supplement to receive a patent for the prevention and treatment of neurodegenerative disease, specifically Alzheimer’s and dementia. It has been clinically proven to improve cognitive functions and memory. Other tested benefits include improvement in sight, focus, clarity, and mood.
Implications For Forensic Psychiatry
What effects might the new conceptualization of neurocognitive disorders have on the practice of forensic psychiatry? One potential change for the better is that the severe, disabling cognitive disorders may more clearly be viewed as lying on a continuum with the less severe disorders that do not reach the threshold for a diagnosis of dementia. Separating the universe of cognitive disorders into dementia and cognitive disorder NOS ran the risk of obscuring commonalities between the two. Cognitive disorder NOS, like all NOS diagnoses, also could carry the implication that the professional making the diagnosis in reality does not know very much about what is going on with the patient. From a medicolegal perspective, the new classification system may prove useful in emphasizing that mild NCDs differ from major NCDs only in degree, not in kind.
From a medicolegal perspective, a diagnosis of mild NCD sounds more definitive and thus may carry more weight in the courtroom than the former cognitive disorder NOS. Only time will tell how widespread the use of the mild NCD diagnostic category in the courtroom will become and how persuasive testimony about the impact of mild NCD on the legal issue at hand will be.
Read Also: How Fast Does Ftd Progress
What Is Mixed Dementia
It is common for people with dementia to have more than one form of dementia. For example, many people with dementia have both Alzheimer’s disease and vascular dementia.
Researchers who have conducted autopsy studies have looked at the brains of people who had dementia, and have suggested that most people age 80 and older probably have mixed dementia caused by a combination of brain changes related to Alzheimer’s disease,vascular disease-related processes, or another condition that involves the loss of nerve cell function or structure and nerve cell death .
Scientists are investigating how the underlying disease processes in mixed dementia start and influence each other. Further knowledge gains in this area will help researchers better understand these conditions and develop more personalized prevention and treatment strategies.
Other conditions that cause dementia-like symptoms can be halted or even reversed with treatment. For example, normal pressure hydrocephalus, an abnormal buildup of cerebrospinal fluid in the brain, often resolves with treatment.
In addition, medical conditions such as stress, anxiety, depression, and delirium can cause serious memory problems that resemble dementia, as can side effects of certain medicines.
Researchers have also identified many other conditions that can cause dementia or dementia-like symptoms. These conditions include:
What Is Dementia Symptoms Types And Diagnosis
Dementia is the loss of cognitive functioning thinking, remembering, and reasoning to such an extent that it interferes with a person’s daily life and activities. Some people with dementia cannot control their emotions, and their personalities may change. Dementia ranges in severity from the mildest stage, when it is just beginning to affect a person’s functioning, to the most severe stage, when the person must depend completely on others for basic activities of living.
Dementia is more common as people grow older but it is not a normal part of aging. Many people live into their 90s and beyond without any signs of dementia.
There are several different forms of dementia, including Alzheimers disease. A persons symptoms can vary depending on the type.
Read Also: Does Prevagen Work For Dementia
Psychological And Psychosocial Therapies
Psychological therapies for dementia include some limited evidence for reminiscence therapy , some benefit for cognitive reframing for caretakers, unclear evidence for validation therapy and tentative evidence for mental exercises, such as cognitive stimulation programs for people with mild to moderate dementia. Offering personally tailored activities may help reduce challenging behavior and may improve quality of life. It is not clear if personally tailored activities have an impact on affect or improve for the quality of life for the caregiver.
Adult daycare centers as well as special care units in nursing homes often provide specialized care for dementia patients. Daycare centers offer supervision, recreation, meals, and limited health care to participants, as well as providing respite for caregivers. In addition, home care can provide one-to-one support and care in the home allowing for more individualized attention that is needed as the disorder progresses. Psychiatric nurses can make a distinctive contribution to people’s mental health.
Some London hospitals found that using color, designs, pictures and lights helped people with dementia adjust to being at the hospital. These adjustments to the layout of the dementia wings at these hospitals helped patients by preventing confusion.
Cognitive training
Personally tailored activities