Lewy Body Dementia: A Common Yet Underdiagnosed Dementia
While its not a household word yet, Lewy body dementia is not a rare disease. It affects an estimated 1.4 million individuals and their families in the United States. Because LBD symptoms can closely resemble other more commonly known disorders like Alzheimers disease and Parkinsons, it is often underdiagnosed or misdiagnosed. In fact, many doctors or other medical professionals still are not familiar with LBD.
Caring For Someone With Lewy Body Dementia
Caring for someone with LBD, or any form of dementia, is hugely challenging. Just as LBD can impact every aspect of a person, caring for someone with the disease can impact every aspect of your daily life. Youll likely face tests of stamina, problem solving, and resiliency. However, your caregiving journey can also be an intensely rewarding experience as long as you take care of yourself and get the support that you need.
Unwrapping The Puzzle Of Dementia
Too often we underestimate the power of a touch, a smile, a kind word, a listening ear, an honest compliment, or the smallest act of caring, all of which have the potential to turn a life around.
As heartbreaking as dementia can be, it is far from cut and dry.
So much research has been done, and we know so much more today than yesterday. For one, again, the fact that it isnt just what happens as we get older.
Don’t Miss: What Is The Color For Dementia
What Are The Causes Of Lewy Body Dementia
The precise cause of LBD is unknown, but scientists are learning more about its biology and genetics. For example, we know that an accumulation of Lewy bodies is associated with a loss of certain neurons in the brain that produce two important chemicals that act as messengers between brain cells . One of these messengers, acetylcholine, is important for memory and learning. The other, dopamine, plays an important role in behavior, cognition, movement, motivation, sleep, and mood.
Scientists are also learning about risk factors for LBD. A risk factor is something that may increase the chance of developing a disease. Some risk factors can be controlled while others cannot. Age is considered the greatest risk factor. No specific lifestyle factor has been proven to increase one’s risk for LBD.
Other known risk factors for LBD include certain diseases and health conditions, particularly Parkinson’s disease and REM sleep behavior disorder, which have been linked to a higher risk of LBD.
Having a family member with LBD also may increase a person’s risk, though LBD is not considered a genetic disease. Variants in three genes APOE, SNCA, and GBA have been associated with an increased risk, but in most cases, the cause is unknown.
Symptoms In The Later Stages Of Dementia With Lewy Bodies

DLB generally;progresses;over a period of several years. In the later stages of the disease, the person may:
- start to have more problems with their day-to-day memory
- become much more easily upset or distressed, resulting in agitation, restlessness, or shouting out
- walk more slowly and;less steadily, causing a higher risk;of;falling and serious injury
- have speech and swallowing problems that may lead to chest infections or a risk of choking
- have problems with eating and drinking ;chewing and swallowing may become more difficult, and the persons stomach and gut may not move food around the body properly, leading to a loss of appetite as well as nausea and discomfort.
Treatment and support for dementia with Lewy bodies
There is currently no cure for DLB, but there are both drug and non-drug treatments that can support the person to live well.;
Read Also: Senile Dementia Of Alzheimer\’s Type
Dlb Parkinsons Disease And Parkinsons Disease Dementia
DLB is closely related to Parkinsons disease. Lewy bodies also cause the damage that leads to movement problems in Parkinsons. People with Parkinsons are more likely to go on to develop dementia, which is known as Parkinsons disease dementia .
DLB and PDD can affect people in very similar ways. If dementia symptoms appear before or at the same time as people start to have movement problems, a diagnosis of DLB is likely to be given. If movement problems are present for a year or more before signs of dementia appear, a diagnosis of PDD is likely to be given.
Differences Between Pdd And Dlb
So, how are PDD and DLB different from each other? That depends on whom you ask. Some clinicians feel that these two conditions are simply different versions of the same disorder. In fact, some professionals use the terms interchangeably. Yet, according to currently agreed-upon diagnostic guidelines, there are some differences.
Read Also: Do People With Dementia Dream
Tests For Dementia With Lewy Bodies
There’s no single test for dementia with Lewy bodies.
The following may be needed to make a diagnosis:
- an assessment of symptoms for example, whether there are typical symptoms of dementia with Lewy bodies
- an assessment of mental abilities this will usually involve a number of tasks and questions
- blood tests to rule out conditions with similar symptoms
- brain scans, such as an MRI scan, CT scan or a SPECT scan these can detect signs of dementia or other problems with the brain
Treatment Of Behavior And Mood Problems In Lewy Body Dementia
Behavioral and mood problems in people with LBD can arise from hallucinations, delusions, pain, illness, stress, or anxiety. They may also be the result of frustration, fear, or feeling overwhelmed. The person may resist care or lash out verbally or physically.
Medications are appropriate if the behavior interferes with the person’s care or the safety of the person or others. If medication is used, then the lowest possible dose for the shortest period of time is recommended.
The first step is to visit a doctor to see if a medical condition unrelated to LBD is causing the problem. Injuries, fever, urinary tract or pulmonary infections, pressure ulcers , and constipation can worsen behavioral problems and increase confusion.
Certain medications, such as anticholinergics and antihistamines may also cause behavioral problems. For example, some medications for sleep problems, pain, bladder control, and LBD-related movement symptoms can cause confusion, agitation, hallucinations, and delusions. Similarly, some anti-anxiety medicines can actually increase anxiety in people with LBD. Review your medications with your doctor to determine if any changes are needed.
Antidepressants can be used to treat depression and anxiety, which are common in LBD. Many of them are often well tolerated by people with LBD.
Recommended Reading: What Shampoos Cause Alzheimer’s Disease And Cancer
Parkinsons Alzheimers And Lewy Body Dementia
Since Lewy body dementia is commonly misdiagnosed for both Parkinsons and Alzheimers, it is helpful to understand how these diseases overlap.
| Overlapping symptoms of Parkinsons, Alzheimers, and Lewy body dementia | |
| Parkinsons and Lewy body dementia | Alzheimers and Lewy body dementia |
Some of the motor symptoms found in bothParkinsons and Lewy body patients include:
|
Some of the cognitive symptoms found in bothAlzheimers and Lewy bodys patients include:
|
How Exactly Is Lewy Body Dementia Related To Alzheimers Disease And Parkinsons Disease
Lewy body dementia is a broad, general term for dementia in which lewy bodies are present in the brain. Dementia with lewy bodies and Parkinsons disease dementia are two related clinical disorders that make up the general broader category of Lewy body dementia. Sometimes LBD is first diagnosed as Parkinsons disease or Alzheimers disease based on its symptoms.
- Parkinsons disease dementia : You might be diagnosed with Parkinsons disease if you start out with a movement disorder typical to Parkinsons but then have your diagnosis changed to PDD when dementia symptoms develop.
- Alzheimers disease : You might start out with memory or cognitive disorder that leads to a diagnosis of AD. Over time, other distinctive symptoms begin to appear and your diagnosis is then changed to dementia with lewy bodies. Distinctive symptoms of LBD include the changes in attention, alertness and cognitive ability; changes in walking and movement; visual hallucinations; REM sleep behavior disorder and severe sensitivity to some antipsychotics used to treat hallucinations.
Recommended Reading: Neil Diamond Alzheimer’s
Behavioral And Mood Symptoms Of Lewy Body Dementia
Changes in behavior and mood are possible in LBD and may worsen as the persons thinking abilities decline. These changes may include:
- Depression
- Apathy, or a lack of interest in normal daily activities or events and less social interaction
- Anxiety and related behaviors, such as asking the same questions over and over or being angry or fearful when a loved one is not present
- Agitation, or restlessness, and related behaviors, such as pacing, hand wringing, an inability to get settled, constant repeating of words or phrases, or irritability
- Delusions, or strongly held false beliefs or opinions not based on evidence. For example, a person may think his or her spouse is having an affair or that relatives long dead are still living.
- Paranoia, or an extreme, irrational distrust of others, such as suspicion that people are taking or hiding things
Caregiver Burden Grief And Well
It is important to understand caregiver burden and overall well-being in LBD due to the repercussions chronic stress and burden have on both caregiver and patient health outcomes. The LBDA caregiver survey found that over 90% of LBD patients were unable to perform certain IADLs, such as shopping and cooking, and over 60% needed help with more basic activities of daily living. Caregiver respondents reported medium to high levels of burden, with the most frequent burden items including fear of the future for their loved one, stress related to being a caregiver with other personal responsibilities, social life interference, and uncertainty. Spousal caregivers had higher burden scores than non-spousal caregivers. The factors most likely to contribute to caregiver burden were sleep and mood disturbances .
When patients with DLB and AD who have similar cognitive deficits are compared, the DLB group exhibits more behavioral features with a higher frequency of hallucinations, apathy, and appetite changes based on the NPI. The DLB group caregivers endorse higher caregiver distress compared to AD caregivers, and high distress is associated with delusions, hallucinations, anxiety, and apathy. In this study, no association was reported between caregiver distress and performance on a functional scale, although the DLB group fared worse on activities of daily living and IADL scales .
Recommended Reading: Dementia Ribbon Colour
What Other Things Help
There are various ways to help a person with DLB. Speech therapy may help improve communication between people with DLB and others. Physical therapy may help strengthen and stretch stiff muscles and help to prevent falls.
Research has shown that;physical exercise helps to enhance brain health and improves mood and general fitness. A balanced diet, enough;sleep, and limited alcohol intake are other important ways to promote good brain health. Other illnesses that affect the brain, such as diabetes, high blood pressure, and high cholesterol, should also be treated if present.
Why Is Dementia Progressive
Dementia is not a single condition. It is caused by different physical diseases of the brain, for example Alzheimers disease, vascular dementia, DLB and FTD.
In the early stage of all types of dementia only a small part of the brain is damaged. In this stage,;a person has fewer symptoms as only the abilities that depend on the damaged part of the brain are affected. These early symptoms are usually relatively minor. This is why mild dementia is used as an alternative term for the early stage.
Each type of dementia affects a different area of the brain in the early stages. This is why symptoms vary between the different types. For example, memory loss is common in early-stage Alzheimers but is very uncommon in early-stage FTD. As dementia progresses into the middle and later stages, the symptoms of the different dementia types tend to become more similar. This is because more of the brain is affected as dementia progresses.
Over time, the disease causing the dementia spreads to other parts of the brain. This leads to more symptoms because more of the brain is unable to work properly. At the same time, already-damaged areas of the brain become even more affected, causing symptoms the person already has to get worse. Eventually most parts of the brain are badly damaged by the disease. This causes major changes in all aspects of memory, thinking, language, emotions and behaviour, as well as physical problems.
Read Also: How To Deal With Dementia Accusations
What Is The Link Between Parkinsons And Lewy Body Dementia
Being Patient: Are Parkinsons disease and Lewy body dementia related?
Dag Aarsland:;Yes, theyre related in terms of symptoms and the brain changes. Many scientists consider Parkinsons and Lewy body dementia as a continuum of disease rather than two separate diseases. But there are very active and lively discussions about that. There are arguments for separating and combining them, but there are many similarities.
Being Patient: Do you group Lewy body dementia with Parkinsons disease in your research?
Dag Aarsland:;From a research point-of-view, we try to separate them. We identify the specifics and categorize patients in different groups and study them carefully in order to see how they relate. In clinical practice, its different. I also see patients with Parkinsons and unfortunately, many of them develop dementia and hallucinations or memory problems. In clinical practice, its very much the same challenges for patients, carers and the doctor in terms of findings and the right therapy.
Can Imaging Tests Diagnose Lewy Body Dementia
Imaging tests, such as computed tomography or magnetic resonance imaging , are done to rule out other causes of dementia such as brain tumors, brain bleeds, stroke, hydrocephalus or other structural causes. Imaging studies for Lewy body dementia are usually normal. The only way to make an absolute diagnosis of LBD is by examining the brain at autopsy.
Also Check: Dementia Ribbon Colors
Outlook For Dementia With Lewy Bodies
How quickly dementia with Lewy bodies gets worse varies from person to person.
Home-based help will usually be needed, and some people will eventually need care in a nursing home.
The average survival time after diagnosis is similar to that of Alzheimers disease around 6 to 12 years. But this is highly variable and some people live much longer than this.
If you or a loved one has been diagnosed with dementia, remember that youre not alone. The NHS and social services, as well as voluntary organisations, can provide advice and support for you and your family.
You May Like: Dementia Neurotransmitter
Alzheimers And Dementia With Lewy Bodies
Pssstwe can write an original essay just for you.
Any subject. Any type of essay.
Well even meet a 3-hour deadline.
121 writers online
Alzheimers and Dementia with Lewy bodies are two separate but similar conditions. Alzheimers affects the brains ability to store new information in the form of memories which accounts for the conditions characteristic memory loss. DLB, on the other hand, targets a different set of cognitive functions specifically problem-solving and reasoning. Although there are tests that can be conducted to more conclusively determine the presence of these conditions, in general, both Alzheimers and DLB are diagnosed through observation and tracking the progression of an individuals symptoms.
Also Check: Do Parkinsons And Alzheimers Go Together
What Affects The Speed Of Progression
The speed at which dementia progresses varies a lot from person to person because of factors such as:
- the type of dementia for example, Alzheimers disease tends to progress more slowly than the other types
- a persons age for example, Alzheimers disease generally progresses more slowly in older people than in younger people;
- other long-term health problems dementia tends to progress more quickly if the person is living with other conditions, such as heart disease, diabetes or high blood pressure, particularly if these are not well managed
- delirium a medical condition that starts suddenly .
There is no way to be sure how quickly a persons dementia will progress. Some people with dementia will need support very soon after their diagnosis. In contrast, others will stay independent for several years.
Signs And Symptoms Of Lewy Body Dementia

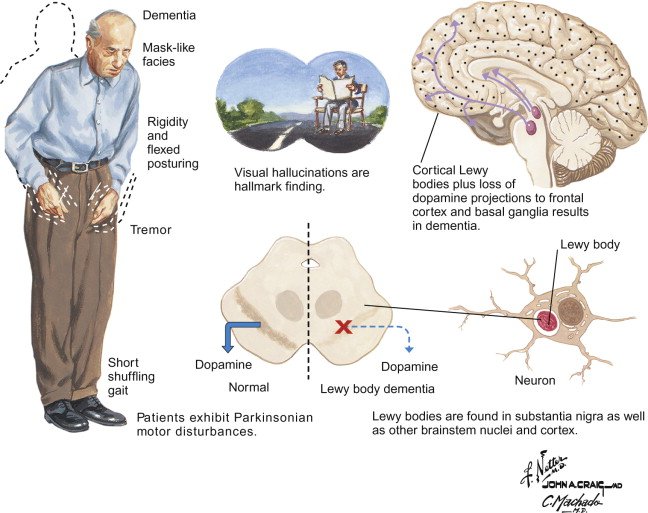
As with Alzheimers disease or Parkinsons disease, the symptoms of Lewy body dementia worsen over time, with intellectual and motor functions deteriorating, typically over several years. Despite the overlaps, however, there are symptoms that indicate the disorder is indeed LBD and not another condition.
While patients with LBD lose cognitive function, they are less prone to the short-term memory loss associated with Alzheimers disease. More commonly, they experience greater problems with executive functions of planning, decision-making, and organization, as well as difficulties with visual perception, such as judging and navigating distances. This can cause you to fall or faint frequently or become lost in familiar settings. Lewy body dementia can also cause sleep disturbances, including insomnia and daytime sleepiness.
If you have Lewy body dementia, you will also exhibit at least two of four core features:
Changes or fluctuations in awareness and concentration.;You swing from a state of alertness to appearing drowsy, confused, or staring into space. These episodes can be unpredictable and last anywhere from a few seconds to several hours.
Spontaneous Parkinsons-like motor symptoms,;such as slowness of movement, rigid muscles, tremor, lack of facial expression, or abnormal gait.
Recurrent visual hallucinations or delusions,;such as seeing shapes, colors, people, or animals that arent there or conversing with deceased loved ones.
Also Check: Does Smelling Farts Help Prevent Dementia
How Is Lewy Body Dementia Treated
There arent any drugs that may stop or reverse Lewy body dementia (LBD, and research is still ongoing. Medications to relieve symptoms include:
- Acetyl cholinesterase inhibitors: These work by increasing the levels of a chemical called acetylcholine in the brain, which improve the ability of the brain cells to send signals to each other