What Does Sundowners Look Like
Sundowners syndrome presents in different ways for each patient, though there are some predictable patterns of changing behavior. To give you a better idea what this condition might look like, here is a hypothetical case of sundowners in a patient with Alzheimer’s disease:
Every case of sundowners is different, but it often follows a similar pattern in which symptoms worsen as the day turns to night, with patients becoming increasingly agitated and more difficult to manage.
Set Good Sleep Habits
Getting enough rest at night is another way to alleviate the symptoms of Sun Downs Syndrome. Experiencing Sun Downs Syndrome can make it harder to get to sleep at night and having less sleep can make it harder to function during the day.
Its an endless loop that affects the quality of life for your loved one .
What Triggers Sundown Syndrome
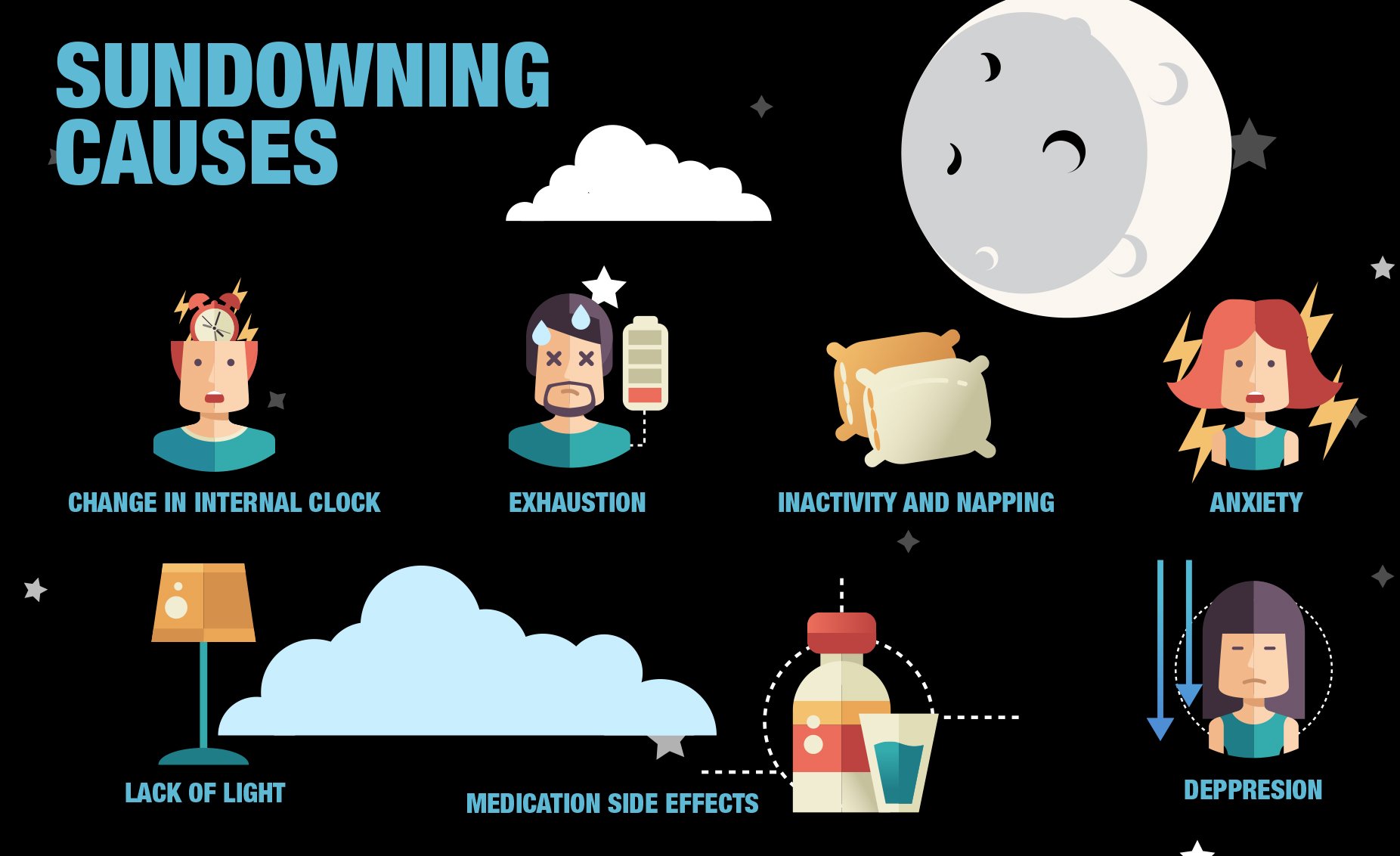
While the cause is unknown, researchers suggest several possible triggers:
- End-of-day activityA flurry of activity toward the end of the day may lead to anxiety and confusion.
- FatigueEnd-of-day exhaustion, or a lack of things to do late in the day, may also be a contributor.
- Low lightAs the sun goes down, the quality of available light may diminish and shadows may increase, making it more difficult for someone with poor eyesight to see. This may increase confusion and agitation.
- Internal imbalanceHormonal imbalances or possible disruptions in the internal biological clock, which regulates cognition between waking and sleeping hours, may trigger sundowning.
- WinterIn some cases, the onset of winters shorter days amplifies sundowning. Seasonal affective disorder, a common depression associated with shorter hours of daylight, may also exacerbate sundowning.
- Infection. In older adults, a urinary tract infection may cause symptoms similar to those of sundowning.
Also Check: What Is The Difference Between Dementia And Senility
Practical Tips On Preventing Sundowning
- Follow a routine during the day that contains activities the person enjoys
- Going outside for a walk or visiting some shops is good exercise
- Limit the persons intake of caffeinated drinks. Consider stopping the person from drinking alcohol altogether. Caffeine-free tea, coffee and cola are available, as is alcohol-free beer and wine
- Try and limit the persons naps during the day to encourage them to sleep well at night instead
- Close the curtains and turn the lights on before dusk begins, to ease the transition into nighttime
- If possible, cover mirrors or glass doors. Reflections can be confusing for someone with dementia
- Once you are in for the evening, speak in short sentences and give simple instructions to the person, to try and limit their confusion
- Avoid large meals in the evening as this can disrupt sleep patterns
- Introduce an evening routine with activities the person enjoys, such as: watching a favourite programme, listening to music, stroking a pet etc. However, try to keep television or radio stations set to something calming and relatively quietsudden loud noises or people shouting can be distressing for a person with dementia.
Sundowning
Understanding And Minimizing Sundowners Syndrome
The long list of symptoms associated with Alzheimers disease and other forms of dementia often includes baffling mood and behavior changes. One particularly disruptive group of symptoms that may arise in the middle and later stages of Alzheimers affects patients at a certain time each day. Known as sundowners syndrome, or sundowning, it involves a pattern of sadness, agitation, fear, delusions and hallucinations that occurs in dementia patients in the late afternoon, evening and at night. This increased confusion around twilight can be distressing for both patients and caregivers alike.
Recommended Reading: What Is The Difference Between Dementia And Senility
Tips For Managing Sundowning
There is not a simple cure for sundowning behaviour. The best thing that you can do is find ways of managing your relatives sundowning when it happens, and taking steps to prevent the agitation that they feel in the afternoon and evening. If your relative is feeling very restless or agitated, there are simple things that you can do to comfort them.
Mutsai Hove Bird recommends the following ways of managing sundowning.
What Are The Signs & Symptoms Of Sundowners Syndrome
Symptoms range in severity and tend to begin in early to late evening and may continue throughout the night. These symptoms include:
- Sudden mood swings
- Disruption of a persons body clock
- Presence of an infection such as a urinary tract infection
- Difficulty separating reality from dreams
- Disruption of regular daily schedule
Read Also: Smelling Your Own Farts Prevents Cancer
What Is The Cause
Doctors arent sure why sundowning happens but many people who experience it have trouble sleeping at night. In turn, fatigue is a common cause, other factors may include:
- An upset in the internal body clock, causing a biological mix-up between day and night.
- As dusk falls, a decrease in lighting and increased shadows, can cause people with dementia to misinterpret what they see and as a result become confused and afraid.
- People with dementia may simply be reacting to signs of tiredness and frustration from caregivers who are exhausted from their day.
- They may have trouble separating dreams from reality, which can be very disorienting.
Coping And Getting Help
Its important to remember that sundown syndrome is not something your loved one can control. Theyre not purposely becoming agitated, angry, or afraid.
If your loved one is experiencing sundown syndrome:
- Try to remain calm and avoid arguing. Instead, validate their feelings and let them know youre listening.
- Offer reassurance and let them know theyre safe and everything is OK.
- Distract and redirect them to favorite activities, such as listening to soothing music, having a snack, or going for a walk.
Dont be afraid to ask for help. Call your loved ones doctor if the signs become too frequent or difficult to manage. A doctor may be able to pinpoint additional triggers or offer different management techniques.
If youd like to explore additional care options, such as memory care, for your family member or loved one, our Senior Living Advisors are available to help.
Canevelli M, et al. . Sundowning in dementia: Clinical relevance, pathophysiological determinants, and therapeutic approaches. Frontiers in Medicine
Understanding and Minimizing Symptoms of Sundown Syndrome posted by Dana Larsen
Nall, R. . Whats to know about Sundowners syndrome? Medical News Today.
You May Like: Does Meredith Grey Have Alzheimer’s
Sundowning In Elderly Dementia Patients: Causes Symptoms And Remedies
Written byEmily LunardoPublished onOctober 11, 2016
Sundowning is commonly seen in dementia patients. The term refers to changes in behavior that occur in the evening when the sun sets. Patients may become more agitated, aggressive, or confused as the night comes. This is often seen in more severe cases of dementia as the disease progresses. Sundowning may be a result of disturbances to the patients 24-hour body clock, loss of daytime routine, insufficient or disturbed sleep, too little or too much light, prescribed medication, and excessive disturbing noise.
A study has uncovered a possible explanation why some patients are susceptible to sundowning. Lead author of the study Tracy Bedrosian said, There have been a few clinical studies documenting sundowning, but until now there hasnt been research in animals to see whats going on in the brain to explain this.
The study showed that aged mice showed much more activity and anxiety-like behaviors before their normal bedtime, compared to middle-aged mice similarly to sundowning in humans.
In these aged mice, the researchers detected changes in the brain parts responsible for attention, emotions, arousal, and other behaviors associated with sundowning in people.
The researchers also found greater expression of the enzyme acetylcholinesterase prior to bedtime high levels of this enzyme are associated with anxiety.
Seeking Treatment Is Important
It is important to seek help from experts and assistance from friends and family. Managing sundown syndrome requires flexibility and creativity as well as a lot of patience and empathy. Often it takes trial and error to discover triggers in your senior before you can find solutions. Every person with dementia reacts differently to triggers and treatment, so you will have to try one thing at a time.
Also Check: What Color Ribbon Is Alzheimer’s
At Sundown The Demons Get Riled Up
Many people enjoy the sunset. Sunsets are picturesque, and they usher in the beginning of evening after a day of labor. Families congregate in the early evening around dinner, chatting and sharing in their daytime activities. For the most part, we look forward to sunsets that transition us from our relatively hectic daytime goings-on to unwinding with family, dinner and subdued pastimes or hobbies, before eventually relaxing into sleep.
It is naturally not so for those who experience sundown syndrome. For them, sunsets and the evening hours can be associated with heightened dread and scorching anxiety, as opposed to the calm and relief many of us feel.
Sundowning syndrome throughout the day
Follow A Chilled Evening Routine

Routines are not a preserve for daytime when you are dealing with a person with dementia. You can also have one in the evening to help ease the transition process.
Here you can include activities like stroking a pet, reading a book if it is possible, listening to soothing music, etc.
If you are watching TV or listening to the radio, set this to a program that is relatively quiet and calming.
People shouting or loud noises can distress individuals who have dementia.
If the above tips do not generate the results you desire, it may be time to seek help from a professional doctor.
He or she will check out the individual with dementia to offer appropriate solutions.
For instance, the medic might have to change medicines that an individual is taking so that he or she only takes drugs that help in relaxation and do not cause more confusion.
Don’t Miss: Scientists Say Smelling Farts Prevents Cancer
The Behavior Of A Person With Sundowning
So, what do you do? I asked, with both my empathy and interest piqued to the utmost. Although I was more or less familiar with the range of behaviors of a person with sundowning, this was the first time I got a first-hand report with this much graphic detail.
We did all the things that we were told and read about. We put her on a regimented routine so that she would find her rhythm and be hardly ever faced with big surprises. We tried to infuse into that routine as much brisk activity in the mornings as she could tolerate, so that come the late afternoons, she would be fully worked out.
How did that work?
Better, I suppose, than had we not done it. And because of her sleeplessness and agitated nights, we eliminated all naps during the day and avoided like the plague coffee and other stimulants, particularly alcohol, since she used to like her drink.
Medicine To Treat Sundowning
When dealing with sundowning and dementia, it is okay to be curious about whether any drugs that make these symptoms better.
This is because caregivers at times go through extremely overwhelming sessions where any interpersonal strategies they try do not seem to work.
Prescriptions are available, but a person with dementia should only use this as a matter of last resort. You must try everything else first before you go down the drug route.
A situation where it may be necessary to use medication is where there is a high degree of agitation that is running out of control and the caregiver cannot manage this effectively.
Medicine can help reduce distress so that the person who has dementia gets fast relief from their upset.
Examples of drugs that the doctor can prescribe include antipsychotic medicine which in as much as they can be effective, they can also carry certain risks.
This is why it is important to be very cautious when administering any type of drug to a person undergoing sundowning.
Also Check: Does Andrea Mitchell Have Dementia
Tips For Preventing Sundowning
There are a number of steps that you can take to prevent sundowning. Because there are many factors that contribute to sundowning, not all of these tips will work for everyone. It is best to keep a record of what does and does not work for your relative.
Mutsai suggested the following tips for trying to prevent sundowning.
Tips To Reduce Sundowning In Elderly
If you a caregiver of a dementia patient suffering from sundowning, there are some things you can do to improve care and effectively handle this type of behavior. Heres what you can try to cope with sundowning:
- Give the patient something meaningful to do in the evening.
- Set up a relaxing activity in the late afternoon/early evening.
- Think about the patients day. Can their behavior be explained by something they may need like food or water? Are they in pain or do they have to use the bathroom? Addressing these needs can help prevent sundowning.
- Minimize the patients daytime naps if they are having difficulties falling asleep.
- Have the patient exercise as it can improve sleep.
- Improve their sleeping environment eliminate caffeine, ensure the room is cool enough and dark.
- Keep appropriate lighting a room that is too dark can cause distress.
Emily Lunardo studied medical sociology at York University with a strong focus on the social determinants of health and mental illness. She is a registered Zumba instructor, as well as a Canfit Pro trainer, who teaches fitness classes on a weekly basis. Emily practices healthy habits in her own life as well as helps others with their own personal health goals. Emily joined Bel Marra Health as a health writer in 2013.
You May Like: Margaret Thatcher Dementia
What Signs Should I Look Out For
The symptoms of sundowning typically occur between the hours of 4:30 p.m. to 11 p.m. and may be worse during the fall and winter months when the daylight hours are shorter.
As a caregiver, some signs to look out for include:
- Signs of fatigue or unmet needs, pain or discomfort
- Agitation, anger or irritability
- High levels of anxiety
- Pacing or wandering
The duration of these symptoms can stop abruptly, change and fade over time, which can be very difficult for caregivers to manage. If you are caring for a loved one experiencing sundowning, you may wonder how to cope with these symptoms.
Prescribed Medication Wearing Off
If your relative takes prescribed medication at a fixed point in the day, it may wear off in the afternoon or evening.
It is important to remember that a person with dementia being distressed is not necessarily sundowning behaviour. They may be trying to communicate a specific need to you, such as pain or constipation.
Recommended Reading: What Color Ribbon Is Alzheimer’s
Hell For Caregivers Of Sundowning Individuals
Thats when Linda began to tear-up. Its like at precisely that time of day, the devil gets into her, and she starts acting up in quite terrifying ways.
When I asked her to expand on that, she said, She all of a sudden becomes agitated and argumentative -even combative. She says crazy things like some bad people are coming after her, and she starts pacing back and forth throughout the living room.
It gets worse, she continued. The nighttime routine is absolute hell for whoever is caring for her. She yells out curse words incessantly and lashes out, and no one can get any sleep for she will be restless and ranting about people of some fifty years ago.
Sundowning Signs And Symptoms

The medical community reminds us that the difference between a sign and a symptom is that your doctor can detect a sign, such as the very first flicker of memory loss or confusion, whereas you tell the doctor what symptoms you have experienced, for example being unsteady on your feet, or enduring frequent headaches.
The symptoms of sundowning are as follows:
- Mood swings, paranoia delusions of being watched, a suspicious deportment
- Disorientation, insecurity, and being argumentative and demanding
- Becoming combative or aggressive, hurling insults, and occasionally lashing out at caregivers
Don’t Miss: Alzheimer’s Ribbon Color
How To Help Someone Who Is Sundowning
Look for patterns. Note the things that seem to trigger it, and then do your best to avoid or limit those triggers.
Keep a daily routine. Set regular times for waking up, meals, and going to sleep. Help them get regular exercise, such as walking, in the early part of the day. Try to schedule their appointments, outings, visits, and bath time in the earlier part of the day, when they are likely to feel their best.
Limit or avoid things that affect sleep.
- Donât let your loved one smoke or drink alcohol.
- Give them sweets and caffeine only in the morning. Offer healthy food and drink later in the day.
- Make a big lunch, and keep their evening meal smaller and simple.
- Avoid letting your loved one nap or exercise later than 4 hours before bedtime. If they absolutely need to nap, try to keep it brief and early in the day.
Keep things calm in the evening.
- Close curtains and blinds and turn on lights. Darkness and shadows can make them more upset.
- Fix the room temperature so they’re comfortable.
- Tell other family members or visitors not to make too much noise.
- Put on relaxing music, read, play cards, or go for a walk to wind down.
- Make sure their sleeping area is comfortable and safe.
- Turn loud, distracting noises, such as phones, stereos, or TVs, down or off.
Sundowning May Be Worsened By Specific Stimuli
Certain factors may exacerbate the effects of sundowning among those with dementia, the Mayo Clinic explains. Fatigue or disruption of one’s usual sleep schedule, for example, may put an added strain on the body’s internal clock, as can low lighting and increased shadows.
Additionally, the presence of a urinary tract infection may trigger more pronounced sundowning symptoms. This can become a hurdle to wellness in geriatric dementia patients, who are far more prone than their younger counterparts to develop such an infection.
For more health news sent directly to your inbox, .
Recommended Reading: What Is Vascular Dementia Life Expectancy