History Of The Clinical Syndrome
In 1817, James Parkinson wrote an essay where he recognized depression as one of the symptoms of the disease named after him.
He described a man who was once a confident with an active mind and cheerful disposition appearing dejected, emancipated and stopping.
Despite all this, the power of his mind and his senses remained unimpaired.
He remained attentive, was able to listen to conversations and had a desire to join in though he was struggling with speech, and he could even read and write.
Years later, in 1861, Vulpian and Charcot observed cognitive impairments in persons who have Parkinsons and Huntingtons diseases.
However, it was not until 1912, when Wilson became the first person to observe a distinction between dementia that involve subcortical structures, and other kinds of cognitive impairments.
Wilson described the impairment of Wilsons disease as one that showed the narrowing of mental horizons.
He went on further to state that the impairment did not include agnosia and apraxia. Wilson also compared this pattern to the one presents in Huntingtons disease.
As research went on by other experts on the subject, the concept of subcortical dementia was finally crystallized into a clinical entity in the mid-1970s.
Prognosis Of Cortical And Subcortical Dementia
The prognosis of cortical and subcortical dementia also significantly varies. Because different types of dementias fall under these two categories, multiple factors commonly affect prognosis.
Among these include general health, age of onset, and other illnesses that the person suffers from. These can affect not only prognosis but life expectancy as well.
What Is Subcortical Dementia
Dementia Consultant | Keynote Speaker | Freelance Writer | Dementia Trainer | Research Assistant
Subcortical dementia is a term that you dont see very often but I did come across it recently and wanted to better understand what it meant. To begin, lets take a look at a few definitions.
Subcortical is as it sounds meaning below the cortex relating to parts of the brain below the cortex. As a refresher, the cerebral cortex is the outermost layer of the brain its the wrinkly part that comes to mind when you picture the brain and is associated with the brains gray matter. Interestingly, cortex means bark in Latin. It plays an important role in many neural processes including memory, language, sensory perception, personality, motor function, processing sensory information, touch, thought processes, judgement, planning and organizing.
Recommended Reading: Does Meredith Grey Have Alzheimer’s
The Evolution Of The Concept
In 1872, at a time when dementia was a unitary concept, Huntington published On Chorea, describing the cognitive impairments in the disease that bears his name. In 1874 Meynert, whose interests were both clinical and neuroanatomical, published Psychiatry: A Clinical Treatise on Diseases of the Forebrain Based upon its Structure, Function and its Nutrition. In this book he sought to relate brain structure to function, and postulated that certain psychiatric symptoms resulted from an imbalance of blood flow between the subcortical and cortical structures. Meynert may have been mistaken in making his emphasis on blood flow, but if he had talked in neural terms instead, he would surely have pre-empted current thinking about the aetiology of subcortical dementia. In 1894 Binswanger introduced a vascular perspective and characterised encephalitis subcorticalis chronica progressiva, subsequently renamed subcortical arteriosclerotic encephalopathy by Olszewski in 1962.
Clinical And Neuropsychological Manifestations
In Alzheimer’s disease senile plaques and neurofibrillary tangles populate the cortex and there is generalised cortical atrophy, especially of the frontal and temporal lobes, with neuronal degeneration affecting particularly the outer three layers. The typical clinical findings include dyscalculia, dysphasias, dyspraxias and agnosias, and are said to be indicative of cortical dysfunction. However, features reflecting subcortical pathology, such as mild extrapyramidal signs, are common.
In the subcortical dementias, on the other hand, the lesions occur predominantly in the basal ganglia, the brainstem nuclei and the cerebellum , and the clinical picture is correspondingly different. In addition to the clinical features of the underlying disease process psychiatric disturbance, bradyphrenia, frontal executive dysfunction and impairment in memory characteristic of subcortical dementia may be present.
In terms of cognition, some evidence suggests that cortical dementia evolves differently from subcortical dementia. Stern et al evaluated cognitive changes over 1-3 years prior to the time dementia was diagnosed in 40 matched pairs of patients with Alzheimer’s disease and Parkinson’s disease. The study showed that the decline in naming on the Boston Naming Test and in performance on the Selective Reminding Test was more rapid in Parkinson’s disease than in Alzheimer’s disease, which Stern and colleagues felt was in keeping with different underlying pathological processes.
You May Like: What Color Ribbon Is Alzheimer’s
Looking At A Neurobehavioral Perspective Of This Dementia
Subcortical dementias have a common neurobehavioral change pattern even though the subcortical structures usually affect different areas of the subcortical pathology.
This is because of the disruption that happens to the frontal-subcortical systems. The clinical presentations include abnormalities in different areas like:
What Are The 5 Main Steps For Diagnostic Coding
What are the 5 main steps for diagnostic coding?
- Step 1: Search the Alphabetical Index for a diagnostic term.
- Step 2: Check the Tabular List.
- Step 3: Read the codes instructions.
- Step 4: If it is an injury or trauma, add a seventh character.
- Step 5: If glaucoma, you may need to add a seventh character.
What are the 7 steps a coder should follow?
- locate the diagnosis in patients health record.
- determine main term of stated diagnosis.
- find main term in alphabetic index.
- read and apply any notes or instructions.
- cross reference code found in alphabetic index.
- read and be guided by conventions and symbols.
- code to highest level of specificity.
What are the 8 steps to accurate coding?
- Identify the main terms.
- Locate the main term in the Alphabetical Index.
- Review any sub terms.
- Verify codes in the Tabular.
- Refer to any instructional notations in the Tabular.
- Assign codes to the highest level of specificity.
Read Also: What Color Is Alzheimer’s Ribbon
The Difference Between Cortical And Subcortical Dementia
The type of dementia may be classified as either cortical or subcortical depending on which part of the brain is the primary location of dementia.
Overview of the brain The cerebrum, is the largest and most highly developed part of the human brain, it accounts for about two-thirds of the brain mass and lies over and around most of the structures of the brain.
A deep groove that runs from front to back divides the brain into the left and right halves known as the two cerebral hemispheres. Each hemisphere is in turn divided into four lobes.
The surface of the cerebral hemispheres is covered by a thin layer known as the cerebral cortex or simply the cortex. It contains billions of brain cells called grey matter.
Underneath the cortex are bundles of nerve fibres known as white matter, which transport nerve signals between parts of the cortex and from the cortex to other parts of the brain.
Cortical dementia
The Legitimacy Of The Distinction
It is well-recognised that cortical abnormalities are frequently found in subcortical diseases and vice versa. Hughes et al looked at 100 cases of histologically confirmed Parkinson’s disease and found that in 17 there was coexistent neuropathological evidence of Alzheimer-type change. In fact, dementia had occurred in 44% of these patients and of these 29% had confirmed Alzheimer pathological change. Cortical change has also been documented in Huntington’s disease and progressive supranuclear palsy. In Alzheimer’s disease, Whitehouse et al demonstrated loss of cholinergic neurons in the subcortical nucleus basalis of Meynert, a finding corroborated by many others.
Neuroimaging findings in some studies add further weight to the idea that the dichotomy is not strict. Starkstein et al , for example, compared patients with Alzheimer’s and Parkinson’s disease with dementia with patients with Parkinson’s disease without dementia, using single-photon emission computed tomography . They found that the two groups with dementia did not differ significantly from each other, but showed significantly more severe hypoperfusion in the superior frontal, superior temporal and parietal areas than did those without dementia. As a consequence, any classification of the dementias must be sensitive to the fact that they seem to lie along a continuum involving a greater or lesser degree of cortical and subcortical pathology.
Read Also: What Color Ribbon Is Alzheimer’s
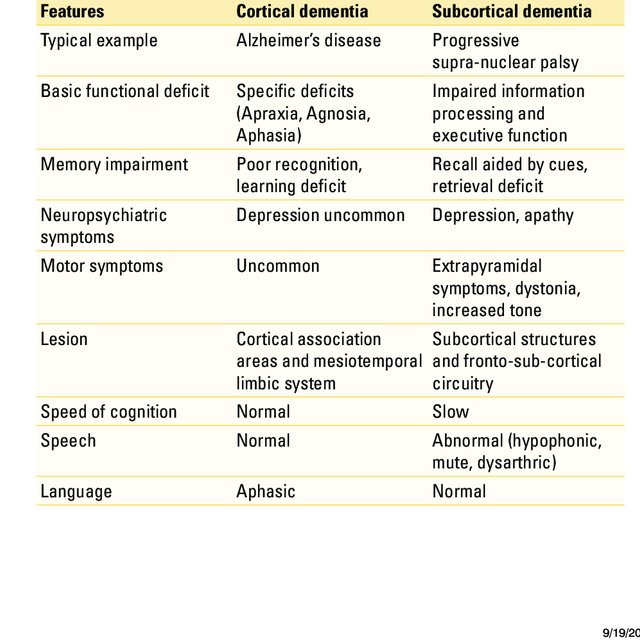
Features Of Cortical And Subcortical Dementia
Both dementias showcase different features that further explain their main differences like:
Basic function deficit
With cortical dementia, you can expect specific deficits like aphasia, which is an impairment of language that affects comprehension or production of speech and the ability to write and read.
Subcortical dementia presents progressive supra-nuclear palsy, a syndrome that can lead to severe problems with eye movement, balance, swallowing, mood and walking, etc.
Memory impairment
Persons with cortical dementia will often experience learning deficits and poor recognition. Individuals with subcortical dementia do not go through severe memory loss issues.
Caregivers and loved ones can use cues to help the affected individuals recall information without too much difficulty.
What Are The Subcortical Parts Of The Brain
Subcortical structures are not visible from the outside of the brain where mostly what you see is the cortex.
Subcortical structures include:
Subcortical vascular dementia is another type of dementia where theres a narrowing and thickening of blood vessels that supply blood to the subcortical regions of the brain resulting in widespread damage. This is also called Binswanger’s disease.
Don’t Miss: Ribbon Color For Dementia
Dementia & Alzheimer’s Disease
There are different types of dementia, one of them being subcortical dementia.
According to many studies and researches, this is a type of dementia that affects the white matter of the brain affecting structures below the cortex.
This type of dementia is a clinical syndrome that includes multiple diseases that primarily affects the subcortical structures that include:
- The midbrain
- Thalamus & hypothalamus
- Basal ganglia
The above are responsible for various functions, including procedural learning, eye movement, voluntary motor movement control, arousal, emotions, visuospatial skills learning of habits, and cognition.
The Keys To Subcortical Dementia
Well now take Parkinsons and Huntingtons diseases to explain the main characteristics of subcortical dementia. Some of them are:
- Motor impairment. One of the main characteristics of subcortical dementia, unlike cortical dementia, is the presence of a severe motor disorder, characterized by the patient slowing down and suffering a loss of balance. Although youll surely associate Parkinsons or Huntingtons diseases with a shaking of the hands, or chorea, the truth is that both subcortical dementias involve hypokinesia , akinesia , or bradykinesia . Theres also an inability to express themselves facially, as the person also loses facial mobility.
- Emotional changes. In cortical dementias, emotional changes may appear as the person comes to terms with the disease. In the case of subcortical dementias, these changes in personality can occur years before the dementia begins to manifest. These people may become irritable, apathetic, or sexually disinterested, among other things.
- Memory disorders. In subcortical dementias, theres a basic memory recovery deficit. The big difference with cortical dementias is that, in subcortical dementias, the patient maintains the ability to learn new information for a long time.
Don’t Miss: What Color Is The Alzheimer’s Ribbon
Difference Between Cortical And Subcortical Dementia
An in-depth look at the differences and similarities between cortical and subcortical dementia and what you should do about it.
Also known as a major neurocognitive disorder, dementia is a group of symptoms that causes problems with memory, reasoning, and thinking.
It occurs when parts of the brain responsible for memory, decision-making, language, and learning are diseased or damaged.
The illness mostly affects elderly persons who are above the age of 65.
Some persons will, however, receive dementia diagnosis when they are younger.
There are over fifty causes of dementia the most common ones being:
- Long-term abuse of drugs or alcohol
- The build-up of brain fluid, etc.
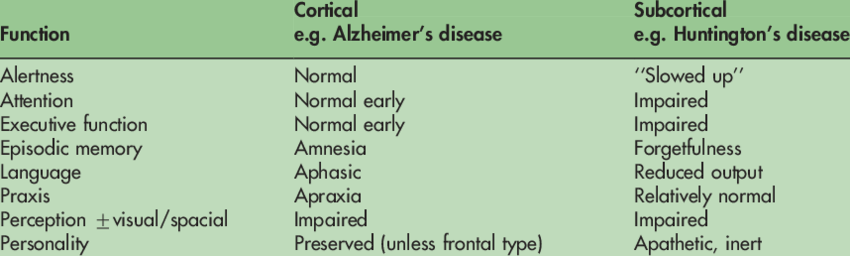
How Are Symptoms Different Between Subcortical And Cortical Dementias
Cortical dementias are associated with memory loss, changes in thinking, and language.
Subcortical dementias are associated more so with symptoms affecting personality and a slowing down of thought processes as well as apathy and depression and motor changes. Language and memory may not be as affected and some reports state that people with subcortical dementias lack the aphasia, agnosia and apraxia characteristic of cortical dementia i.e. Alzheimers disease.
Recommended Reading: What Color Ribbon Is Alzheimer’s
What Are The 10 Steps To Reviewing An Operative Report
- Step 2: Note the pre- and post-operative diagnoses.
- Step 3: Read the general statement of the procedure.
- Step 4: Check for complications.
- Step 5: Note the pathology specimen.
- Step 6: Check the EBL.
- Step 7: Review the findings.
- Step 8: Note the indications.
- Step 9: Read the description of the procedure carefully.
Subcortical Contribution To Psychiatric Disorder
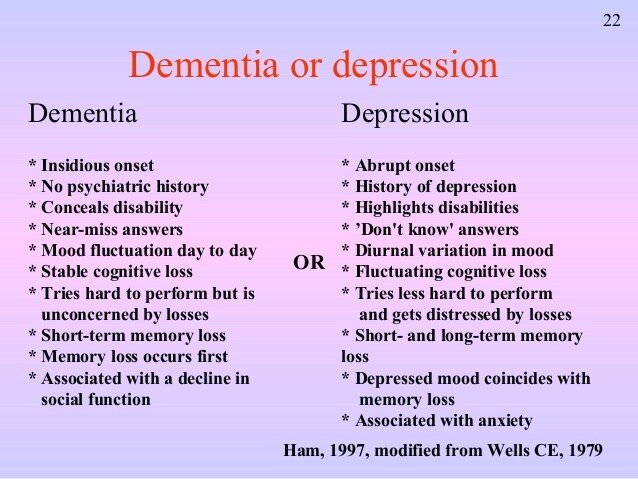
For the purposes of investigating cognitive impairments in depression, Caine defined pseudodementia as follows:
it is an intellectual impairment in a patient with a primary psychiatric disorder
the features of the neuropsychological disorder resemble, at least in part, the presentation of a neuropathologically induced cognitive deficit
the intellectual disorder is reversible
the patient has no apparent primary neuropathological process leading to the genesis of the disturbance.
The disorder in question is usually hysteria or depression but, because of the additional complexities of understanding the mechanism of the former and how it relates to the purposeful behaviour of malingering, attention is here confined to depressive pseudodementia.
Depression is common in subcortical disorders and it is perhaps not surprising therefore that the pattern of cognitive impairment that one sees in the context of depression can be subcortical. As Lishman eloquently puts it:
Don’t Miss: Senility Vs Dementia Vs Alzheimer’s
The Differences Between Cortical And Subcortical Dementia
22 May, 2020
Dementias located in cortical areas wont have the same impact on a person as those in subcortical areas. In this article, well be looking at the differences between cortical and subcortical dementia.
When we talk about dementia, we mean progressive global cognitive impairment. Contrary to what many people may think, aging isnt a cause of neurogenerative diseases. Although theres comorbidity , theres no causality.
A curious fact is that 30 percent of Parkinsons patients have dementia, but the remaining 70 percent dont. But are all dementias the same? The answer is no there are two main types of dementia, associated with different diagnoses. In this article, as we mentioned above, well be talking about the differences between cortical and subcortical dementia.
During the first half of the 20th century, dementia was equivalent to progressive intellectual deterioration. In 1987, the American Psychological Association established diagnostic criteria. They stated that cognitive impairment had to be accompanied by a deterioration in memory, and
In 2012, the term dementia was eliminated and replaced by neurocognitive disorder.
Impaired Ideomotor Limb Apraxia In Cortical And Subcortical Dementia: A Comparison Of Alzheimers And Huntingtons Disease
Log in to MyKarger to check if you already have access to this content.
Buy a Karger Article Bundle and profit from a discount!
If you would like to redeem your KAB credit, please log in.
Save over 20%
- Rent for 48h to view
- Buy Cloud Access for unlimited viewing via different devices
- Synchronizing in the ReadCube Cloud
- Printing and saving restrictions apply
USD 8.50
- Access to all articles of the subscribed year guaranteed for 5 years
- Unlimited re-access via Subscriber Login or MyKarger
- Unrestricted printing, no saving restrictions for personal use
The final prices may differ from the prices shown due to specifics of VAT rules.
Also Check: Does Smelling Farts Help Prevent Dementia
What Is Cortical And Subcortical
4.9/5corticalcortexcortexsubcortical
Similarly, it is asked, what are the subcortical areas of the brain?
Subcortical Structures and Functions
- Tectum.
- Tegmentum.
Subsequently, question is, is the cerebellum cortical or subcortical? Cortical vs. Subcortical Strokes. A stroke may affect cortical regions of the cerebral cortex, including the frontal, parietal, temporal and occipital lobes, or structures subcortically, below the cortex, including the internal capsule, thalamus, basal ganglia, brainstem and cerebellum.
Thereof, what is the difference between cortical and subcortical dementia?
In most common types of dementias there is widespread degeneration in the cerebral cortex such as the plaques and neuro fibrillation tangles which are the hallmark of Alzheimer’s disease. In subcortical dementia, there is targeted damage to regions lying under the cortex.
What is cortical function?
Cortical functions are well-defined for primary cortical areas like motor, sensory and visual functions. Recent data from functional imaging indicate that large and diverse areas of the cerebral cortex are involved in planning motor tasks or coding .
Subcortical Dementia Treatment Options

Although this kind of dementia remains highly controversial, some researchers believe that they are part of the dementias that can be treated. This is because most disorders that are associated with dementia respond to appropriate treatment and some may be reserved completely.
Consulting your physician will give you a better idea of which treatment route to take while dealing with this dementia type.
Recommended Reading: What Is The Difference Between Dementia And Senility
Mixed Cortical Vascular Dementia
Cortical dementia develops as a result of disorders that affect the cerebral cortex, the outermost layer of the brain. Cortical dementia typically yields a dementia signature consistent with symptoms of Alzheimers disease, meaning symptoms primarily involve a decline in cognitive abilities, such as memory. Mixed cortical vascular dementia is the combination of multiple dementias, including vascular dementia, that expresses the cortical dementia signature in addition to that of vascular dementia.
In the most common form, the beta-amyloid plaques and neurofibrillary tangles associated with Alzheimers disease are present in addition to blood vessel changes associated with vascular dementia. According to the Alzheimers Society, this form of mixed dementia accounts for at least 10% of dementia diagnoses. Symptoms of mixed cortical vascular dementia may include those of Alzheimers, those of vascular dementia, or a combination of the two.