Types And Symptoms Of Dementia
Changes in the structure and chemistry of the brain cause memory and thinking problems in Parkinsons disease . The protein alpha-synuclein is central to Parkinsons. This protein forms sticky clumps, called Lewy bodies, that disrupt normal brain functioning. Parkinsons dementia is thought to be related to Lewy bodies.
Signs And Symptoms Of Pdd
Common signs and symptoms of Parkinsons disease dementia include:
- Poor memory and concentration
- Depression
- Visual hallucinations
If youve noticed some of the above signs and symptoms in yourself or a loved one, its important to get them checked out. But dont jump to conclusions. People with Parkinsons often experience cognitive changes such as anxiety, lack of motivation, and slowed thinking. These symptoms do not automatically mean dementia.
How Is Parkinson Disease Diagnosed
Parkinson disease can be hard to diagnose. No single test can identify it. Parkinson can be easily mistaken for another health condition. A healthcare provider will usually take a medical history, including a family history to find out if anyone else in your family has Parkinson’s disease. He or she will also do a neurological exam. Sometimes, an MRI or CT scan, or some other imaging scan of the brain can identify other problems or rule out other diseases.
Recommended Reading: Bob Knight Health Condition
Epidemiology Of Dementia And Parkinson’s Disease
Dementia and PD are both diagnosed frequently and increase mortality . Perhaps dementia is perceived more so as a memory problem and a disease of old age, but the incidence of dementia and PD in younger age is similar. In the Netherlands, for dementia, the incidence per 1,000 person-years is 0.4 among those aged 6064 , and for PD, it is 0.3 . Dementia incidence patterns, however, show a much steeper increase with age mounting to 27 per 1,000 person-years for those 85 and over, compared to 4 for PD over 85. In view of similar mortality , therefore, the prevalence of dementia in the general population is much higher than prevalence of PD . However, adjusted for age and other factors, 6-year mortality in PD is higher than in Alzheimer’s dementia . Age adjustment is relevant also as it shows that comorbid disease may be equally prevalent for Alzheimer’sa main type of dementiaand PD across the same age groups .
S For Caring For A Person With Parkinsons Dementia
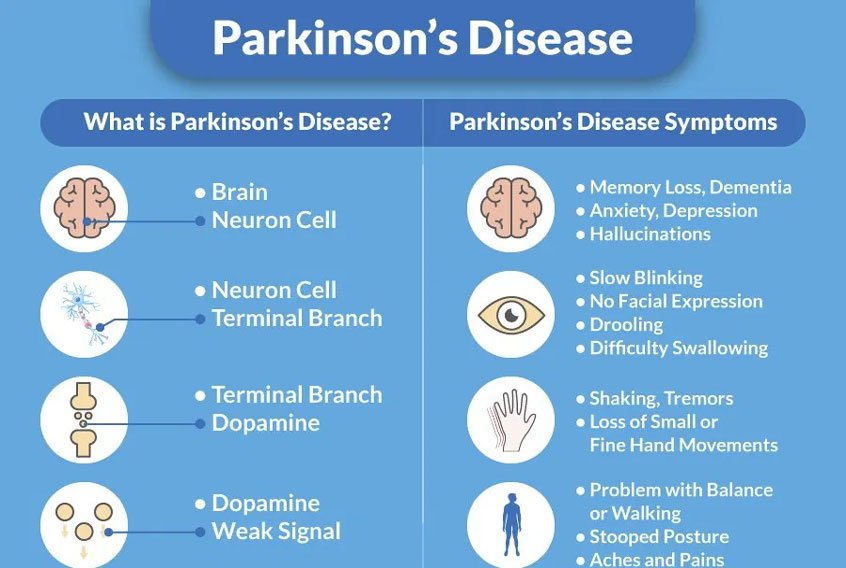
Parkinsons disease is known for its associated motor symptoms, such as tremor and slowed movement. People can be surprised to learn that cognitive changes are among common PD non-motor symptoms. Significant cognitive impairment can impact care partners, too. Education and healthy coping strategies ensure everyones best care.
The following article is based on a Parkinsons Foundation Expert Briefings webinar exploring care partner strategies to identify and help people with PD dementia, hosted by Joseph Quinn, MD, a neurologist at Parkinsons Foundation Center of Excellence Oregon Health & Science University and the Portland VA Medical Center. Dr. Quinn, the Parkinsons Center director for both institutions, focuses his research on cognitive decline prevention and dementia treatment.
What is PD Dementia?
Mild cognitive impairment is very common with Parkinsons disease. It can impact memory and thinking but doesnt always affect daily activities. Dementia, however, is when cognitive changes impact daily living. Dementia may or may not occur in people with PD. According to recent research, 30 percent of people with Parkinsons do not develop dementia as part of the disease progression.
The different types of dementia include:
Parkinsons Disease Dementia and Lewy Body Dementia Family Checklist
Read Also: Alzheimer Ribbon
Tip : Make It A Priority To Be Socially Engaged
The more socially active you are, the more you connect face-to-face with others, the stronger your memory and cognition is likely to be. You dont need to be a social butterfly or the life of the party, but you do need to regularly connect with people who care about you.
Connecting with others is the most effective means of relieving stress which left unchecked can exacerbate symptoms of Parkinsons disease. Staying socially engaged also stimulates immune function that may slow the progress of disease. While many of us become more isolated as we get older, its never too late to meet others and develop new friendships.
Tips for meeting new people
- Volunteer
Hotlines and support
In the U.S.: Call the Helpline at 1-800-473-4636 or visit Parkinsons Foundation for resources and support. For Parkinsons Disease Dementia, call the Alzheimers Association helpline at 1-800-272-3900.
UK: Call the helpline at 0808 800 0303 or visit Parkinsons UK to find support
Australia: Call the info line at 1800 644 189 or visit Parkinsons Australia for links to state organizations that provide support and services.
Canada: Call 1 800 565-3000 for information or referrals or visit Parkinson Society of Canada for regional resources and support.
How Is Age Related To Pdd
Both PD and PDD are more common with increasing age. Most people with PD start having movement symptoms between ages 50 and 85, although some people have shown signs earlier. Up to 80% of people with PD eventually develop dementia. The average time from onset of movement problems to the development of dementia is about 10 years.
Read Also: Neurotransmitter Alzheimers
Parkinsons Dementia Vs Alzheimers Dementia
According to experts, Parkinsons dementia can cause impaired physical activity and impacts motor skills. Two neurotransmitters called dopamine and serotonin tend to be damaged by Parkinsons.
In addition to causing issues with movement and coordination, this form of dementia can also cause a slower thought process and memory problems. This is usually less pronounced however, until the later stages of the disease.
With Alzheimers, two types of proteins in the brain, tangles and plaques , accumulate and kill brain cells. This Alzheimers-induced dementia affects memory, clear thinking, language skills, and orientation. It reduces comprehension, learning capacity, and judgement. Storing new information and memory retrieval are impacted more than motor skills.
Distinguishing between these neurodegenerative conditions is important to determine the best treatment approach. Medications for one of condition might create problems when given to a patient with the other condition.
Wondering how to support a loved ones goal of being able to age at home? Were here to help. Whether its for one month or ten years, our caregivers can help your loved one live the life they want at home. Call a Care Advisor today at or and learn more about how we can support your needs.
Typical Timescale For Pdd
According to the Parkinsons Foundation, PDD is typically diagnosed when a person living with Parkinsons disease experiences cognitive decline after a year or more of motor symptoms. But in most cases, people experience many years of tremors, slowness of movement, and muscle cramps before showing signs of significant cognitive decline. The Weill Institute for Neurosciences estimates the average time from onset of movement problems to developing dementia is 10 years. An estimated 50% to 80% of people with Parkinsons will eventually experience Parkinsons disease dementia, says the Alzheimers Association.
Recommended Reading: Alzheimer’s Neurotransmitters Affected
How Are Parkinsons And Dementia Related
Parkinsons and dementia are two of the most common degenerative neurological conditions in this country, affecting many thousands of people. However, there are a lot of myths and misunderstandings about the illnesses.
If you have been told that you have either condition, the future may seem bleak and bewildering. Whether youve found this blog having been recently been diagnosed, or are worried about a loved one, then read on, hopefully, we can help you to gain some understanding.
Relation Of The Neural Network Perspective To The Neuropathology Of Parkinsons Disease Dementia
At the neuropathological level the consensus from most studies to date is that the amount of Lewy-related pathology in neocortical and limbic areas is the most important factor in the development of PDD . However, the significance of Lewy-related pathology occurrence in particular cortical areas is debated, for example one retrospective autopsy study found that severity of cognitive decline in PDD correlated with Lewy-related pathology in the frontal and cingulate gyri , while another found no significant correlations in these regions but did find one in relation to temporal lobe Lewy-related pathology . Meanwhile some patients with Parkinsons disease with cortical Lewy-related pathology do not develop dementia at all . The significance of concurrent Alzheimer-type pathologies is hotly debated , although a recent study quantitatively assessing cortical Lewy-related pathology and Alzheimer-type pathologies found that a combination of both correlated most robustly with development of PDD . The relative contributions of other pathologies including microvascular disease, cerebral amyloid angiopathy, argyrophilic grains and TARDBP remain unclear .
Also Check: Difference Between Senility And Dementia
What Is Parkinsons Disease Dementia
Parkinsons disease dementia is a brain disorder that occurs in somebut not allpeople living with Parkinsons disease. The brain cell damage caused by the disease can lead to a loss of memory and other cognitive functions such as problem solving and speed of thinking. These changes in thinking and behavior can impact your daily living, independence, and relationships.
In those who do develop Parkinsons disease dementia, there is at least one yearand usually 10 to 15 yearsbetween the Parkinsons diagnosis and the onset of dementia. According to estimates by the Alzheimers Association, 50% or more of people with Parkinsons disease eventually experience dementia, although there are a number of risk factors that impact the likelihood of developing symptoms:
- Parkinsons patients who experience hallucinations, excessive daytime sleepiness, and more severe motor control problems are at higher risk for dementia.
- Dementia is more common in people who are older at onset of Parkinsons.
- Dementia is a bigger risk factor in non-tremor predominant Parkinsons.
- Overwhelming stress, cardiovascular disease, and adverse reactions to the Parkinsons disease drug levodopa can also indicate an increased risk for developing dementia.
- Dementia is relatively rare in people who develop Parkinsons before age 50, no matter how long they have had the disease.
How Is Parkinsons Disease Dementia Diagnosed
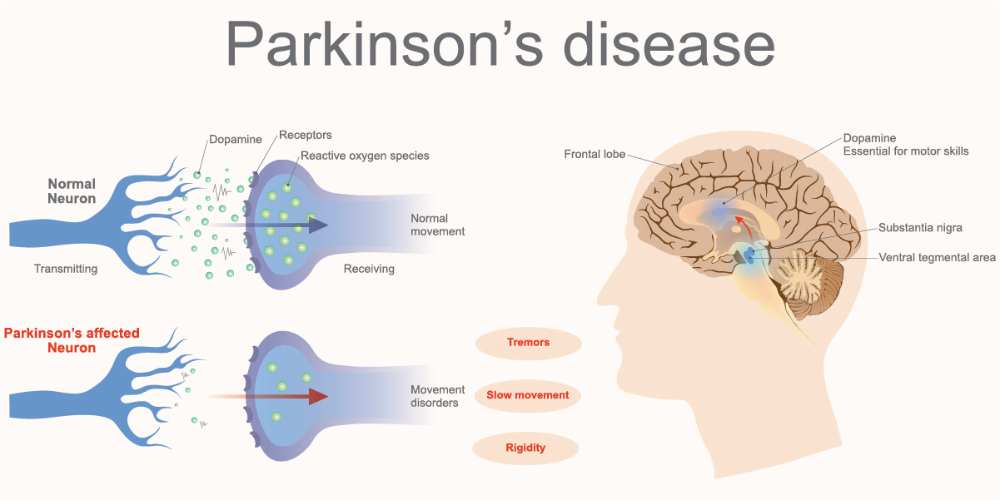
No single test can diagnose Parkinsons disease dementia. Instead, doctors rely on a series or combination of tests and indicators.
Your neurologist will likely diagnose you with Parkinsons and then track your progression. They may monitor you for signs of dementia. As you get older, your risk for Parkinsons dementia increases.
Your doctor is more likely to conduct regular testing to monitor your cognitive functions, memory recall, and mental health.
Also Check: Senility Vs Dementia
Clinical Diagnostic Criteria For Pdd
Prior to the development of the MDS-proposed clinical diagnostic criteria , PD patients were diagnosed with dementia according to the DSM-IV criteria on the basis of dementia due to other general medical conditions. Unfortunately, within these criteria, the section devoted to PDD is rather generic and imprecise, with reference to cognitive and motor slowing, executive dysfunction, impairment in memory retrieval and frequent exacerbation by depression. A comprehensive, systematic review of the literature related to the epidemiological, cognitive and neuropsychiatric motor and other clinical features, ancillary examinations, and clinico-pathological correlations enabled the MDS Task Force to propose clinical criteria for the diagnosis of possible and probable PDD .
Managing The Effects Of Parkinsons Disease
Currently there is no cure for Parkinsons disease but UK and international research is ongoing.
With Parkinsons disease the interventions are focused on support, management of the changes, working with the person and their family to ensure they can live as well as possible with the condition. The physical effects of Parkinsons disease can be managed by:
- adapting the home environment so any trip hazards are removed and risks minimised
- a referral to Speech and Language Therapy if there are speech or swallowing problems
- a referral to a physiotherapist if there are movement issues
- a referral to an occupational therapist for aids and devices that may help around the house
If the person with Parkinsons has significant communication or cognitive issues they can be reduced by:
- reviewing the medication given for Parkinsons as this may be worsening the cognitive symptoms
- speaking slowly and clearly if understanding and thought processes are slowed
- reducing distractions
- giving time for communication it may take longer to respond
- asking questions to narrow down the answer, give choices or use yes/no cards or picture cards the person may have word finding difficulties as well as needing longer to respond
- using a mobile phone, tablet or electronic communication aid
- avoid unfamiliar or noisy places as they can cause distress
- providing a routine and activities that the person enjoys and feels comfortable with
Read Also: Dementia Ribbon Color
Living With Parkinson Disease
These measures can help you live well with Parkinson disease:
- An exercise routine can help keep muscles flexible and mobile. Exercise also releases natural brain chemicals that can improve emotional well-being.
- High protein meals can benefit your brain chemistry
- Physical, occupational, and speech therapy can help your ability to care for yourself and communicate with others
- If you or your family has questions about Parkinson disease, want information about treatment, or need to find support, you can contact the American Parkinson Disease Association.
Dysexecutive Symptoms May Emerge When Inter
How dysfunction in the fronto-striatal and mesocortical dopaminergic networks may interact to cause dysexecutive symptoms in PDD is unclear. However the results of suggest that it is supervening dysfunction in the mesocortical projections to the insular upon existing fronto-striatal network disruption that heralds major executive impairment. Indeed there is limited evidence suggesting some redundancy between the two systems in early Parkinsons disease: in one study patients performing a set-shifting task did not display behavioural impairment despite fronto-striatal hypoactivation on functional MRI, possibly because they displayed concurrent hyper-activation in the insular and fronto-parietal networks, which was not present in controls . Using functional MRI, also noted a relative increase in blood-oxygen level-dependent activity within frontal regions in patients during a matching task. Although this evidence is indirect it suggests that the mesocortical network may partially compensate for fronto-striatal dysfunction in early disease, until it too is damaged, compensation is lost, and a full-blown dysexecutive syndrome develops. Such a proposal is compatible with, and extends, the hypothesis proposed by others that deficient interplay between the fronto-striatal and mesocortical dopamine networks underlies the dysexecutive syndrome of Parkinsons disease .
Read Also: Alzheimer’s Ribbon Color
Early Signs Of Parkinsons Disease Dementia
In the beginning, PDD can be subtle. Early on, there may be memory loss and difficulties with daily activities, says Michael S. Okun, M.D., executive director of the Norman Fixel Institute for Neurological Diseases at University of Florida Health in Gainesville. Delusions or hallucinations may also start to happen. Dr. Petrossian points out that there can be an overlap between the early signs of dementia and mild cognitive impairment due to Parkinsons disease, which can make it difficult to learn new skills and recall information or conversations.
Epidemiology And Natural History Of Dlb And Pdd
Approximately 12% of those aged above 65 years are diagnosed with DLB worldwide , affecting approximately 5% of all dementia cases in those over the age of 75 . Its incidence is 0.71.4 new cases/100,000 person-years or 3.5/100,000 person-years . For PDD, the cumulative prevalence is of 75% of PD patients surviving more than 10 years , 83% after 20 years , and up to 95% by age 90 years , with an overall prevalence of 31.1% and incidence rates from 0.43 to 1.13/100,000 person-years , indicating that, annually, approximately 10% of a PD population will develop dementia . The data concerning age at disease or dementia onset are highly variable. Whereas in the Olmsted County study DLB patients were younger at symptom onset than those with PDD and had more hallucinations and cognitive fluctuations, others have reported younger age at disease onset in PDD , or no essential differences between disorders .
Don’t Miss: Is Bobby Knight Still Alive
Can Parkinsons Dementia Be Reversed
No specific cure has been identified for Parkinsons Disease Dementia. Rather, treatments have been aimed at reducing the symptoms of dementia and helping the patient maintain a high quality of life. Doctors treating patients of PD Dementia generally prescribe medications such as:
- Antidepressants
- Cholinesterase inhibitors
- Clonazepam and L-dopa
Serotonin reuptake inhibitors are known to reduce depression symptoms. The ones widely prescribed by doctors include:
- Prozac
- Zoloft and
- Lexapro
Cholinesterase inhibitors help reduce the effects of cognitive decline in people with dementia whereas Clonazepam helps enhance sleep quality. L-dopa helps reduce movement issues caused by PD but runs the risk of making confusion and dementia symptoms worse.
Doctors treating PD Dementia patients may also prescribe antipsychotic drugs but generally do so with caution, the reason being these reduce psychotic episodes but increase Parkinsons symptoms. The use of these drugs may also cause increased confusion and change in consciousness. For the record, Pimavanserin and Nuplazid have been identified as effective antipsychotic drugs.
What Are The Symptoms Of Parkinson’s Disease Dementia

Cognitive impairment in Parkinson’s disease may range from a single isolated symptom to severe dementia.
- The appearance of a single cognitive symptom does not mean that dementia will develop.
- Cognitive symptoms in Parkinson’s disease usually appear years after physical symptoms are noted.
- Cognitive symptoms early in the disease suggest dementia with Parkinsonian features, a somewhat different condition.
Cognitive symptoms in Parkinson’s disease include the following:
- Loss of decision-making ability
- Loss of short- and long-term memory
- Difficulty putting a sequence of events in the correct order
- Problems using complex language and comprehending others’ complex language
Persons with Parkinson’s disease, with or without dementia, may often respond slowly to questions and requests. They may become dependent, fearful, indecisive, and passive. As the disease progresses, many people with Parkinson’s disease may become increasingly dependent on spouses or caregivers.
Major mental disorders are common in Parkinson’s disease. Two or more of these may appear together in the same person.
The combination of depression, dementia, and Parkinson’s disease usually means a faster cognitive decline and a more severe disability. Hallucinations, delusions, agitation, and manic states can occur as adverse effects of drug treatment of Parkinson’s disease, this might complicate the diagnosis of Parkinson’s dementia.
Also Check: Diet Coke And Dementia