What Are The Treatments For Lewy Body Dementia
There is no cure for LBD, but treatments can help with the symptoms:
- Medicines may help with some of the cognitive, movement, and psychiatric symptoms
- Physical therapy can help with movement problems
- Occupational therapy may help find ways to more easily do everyday activities
- Speech therapy may help with swallowing difficulties and trouble speaking loudly and clearly
- Mental health counseling can help people with LBD and their families learn how to manage difficult emotions and behaviors. It can also help them plan for the future.
- Music or art therapy may reduce anxiety and improve well-being
Support groups can also be helpful for people with LBD and their caregivers. Support groups can give emotional and social support. They are also a place where people can share tips about how to deal with day-to-day challenges.
NIH: National Institute of Neurological Disorders and Stroke
Medications For Cognitive Symptoms
Some medications used to treat Alzheimer’s disease are also used to treat the cognitive symptoms of LBD. These drugs, called cholinesterase inhibitors, act on a chemical in the brain that is important for memory and thinking. They may also improve behavioral symptoms.
The U.S. Food and Drug Administration approves specific drugs for certain uses after rigorous testing and review. However, doctors can prescribe a drug for any use if they think it will help a patient. The FDA has approved one Alzheimer’s drug, rivastigmine , to treat cognitive symptoms in Parkinson’s disease dementia. This and other Alzheimer’s drugs can have side effects such as nausea and diarrhea.
Evaluation Of Pain Management: Responsiveness
To perform valid responsiveness studies, RCTs with appropriate sample sizes are a prerequisite, but most of the current controlled studies did not include a representative sample of elderly with dementia. Further, it is vital that the final evaluation of the psychometric qualities of a scale considers the criterion of responsiveness against the criterion of reliability. Focusing only on the volatile and state-like aspects of pain in an instrument may increase its responsiveness, because every change is detected, but may neglect resistant and trait-like pain features . The result might be a premature all-clear when pain has not been fully addressed.
Recommended Reading: What Is The Difference Between Dementia And Senility
Data Collection And Analysis
The semi-structured interview guide was developed by the PI and revised in response to suggestions from LBDA staff, two experts guiding the LBDA, and three caregivers for individuals who died from DLB. The guide included 11 open-ended questions regarding EOL experiences of the participant and his or her loved one with DLB . The PI, a physician specializing in DLB, conducted all the interviews. She had no prior relationship with participants. A professional service transcribed interviews verbatim, therefore member checking was not employed. Participants had the opportunity to receive study results when available.
Building A Lewy Body Dementia Care Team

After receiving a diagnosis, a person with LBD may benefit from seeing a neurologist who specializes in dementia and/or movement disorders. Your primary doctor can work with other professionals to follow your treatment plan. Depending on an individual’s particular symptoms, physical, speech, and occupational therapists, as well as mental health and palliative care specialists, can be helpful.
Support groups are another valuable resource for people with LBD and their caregivers. Sharing experiences and tips with others in the same situation can help people find practical solutions to day-to-day challenges and get emotional and social support.
Don’t Miss: What Shampoos Cause Alzheimer’s Disease And Cancer
Two Of The Following Are Present :
- Fluctuating cognition: Mental problems varying during the day, especially attention and alertness.
- Visual hallucinations: Detailed and well-formed visions, which occur and recur.
- RBD: Physically acting out dreams while asleep.
A DLB diagnosis is even more likely if the individual also experiences any of the following: repeated falls, fainting, brief loss of consciousness, delusions, apathy, anxiety, problems with temperature and blood pressure regulation, urinary incontinence, and chronic constipation, loss of smell, or sensitivity to neuroleptic medications that are given to control hallucinations and other psychiatric symptoms.
Finally, the timing of symptoms is a reliable clue: if cognitive symptoms appear before or within a year of motor symptoms, DLB is more likely the cause than Parkinsonâs disease. Signs of stroke or vascular dementia usually negate the likelihood of DLB.
Testing is usually done to rule out other possible causes of dementia, motor, or behavioral symptoms. Brain imaging can detect brain shrinkage and help rule out stroke, fluid on the brain , or subdural hematoma. Blood and other tests might show vitamin B12 deficiency, thyroid problems, syphilis, HIV, or vascular disease. Depression is also a common cause of dementia-like symptoms. Additional tests can include an electroencephalogram or spinal tap .
Assessment Of Neuropathic Pain
Neuropathic pain is often based on underlying diseases such as diabetic neuropathy, after stroke and amputation. Assessing this form of pain in dementia is extremely challenging. The assessment of central neuropathic pain, which is defined as pain caused by a lesion, or dysfunction of the central nervous system, is even more complex. Approximately 35% of stroke patients suffer from post-stroke central neuropathic pain. Because this deafferentiation also takes place in VaD, it has been suggested that central neuropathic pain is by far the most undertreated type of pain in patients with dementia. The assessment and treatment of this type of pain is of high clinical relevance, but it has hardly been described in the literature, most likely because it requires assessment and treatment approaches that differ from those of other types of pain. In 2004, the European Federation of Neurological Societies Panel on Neuropathic Pain published guidelines on neuropathic pain assessment that included thorough sensory bedside testing in individuals with neuropathic pain. This guidance would provide a useful basis for an assessment tool for neuropathic pain. However, as far as the authors are aware, no such instrument has been developed to date.
Read Also: Does Bob Knight Have Dementia
How Is Lewy Body Dementia Diagnosed
There isn’t one test that can diagnose LBD. It is important to see an experienced doctor to get a diagnosis. This would usually be specialist such as a neurologist. The doctor will
- Do a medical history, including taking a detailed account of the symptoms. The doctor will talk to both the patient and caregivers.
- Do physical and neurological exams
- Do tests to rule out other conditions that could cause similar symptoms. These could include blood tests and brain imaging tests.
- Do neuropsychological tests to evaluate memory and other cognitive functions
LBD can be hard to diagnose, because Parkinson’s disease and Alzheimer’s disease cause similar symptoms. Scientists think that Lewy body disease might be related to these diseases, or that they sometimes happen together.
It’s also important to know which type of LBD a person has, so the doctor can treat that type’s particular symptoms. It also helps the doctor understand how the disease will affect the person over time. The doctor makes a diagnosis based on when certain symptoms start:
- If cognitive symptoms start within a year of movement problems, the diagnosis is dementia with Lewy bodies
- If cognitive problems start more than a year after the movement problems, the diagnosis is Parkinson’s disease dementia
What Happens After Referral
Once your GP has referred you to a specialist, you may be required to attend an appointment at a specialist clinic. When you attend the clinic you can expect someone to ask about your symptoms, your medical history and your background. Various tests are carried out and usually a family member is asked to discuss any changes they have noticed in you. They may be asked to complete an assessment form to help clinic staff understand the problems clearly. Sometimes this is done during one long clinic session and sometimes it is split over two visits. Normally you will have a short physical examination. A nurse may also be in attendance. This is the nurse who is likely to see you once any diagnosis has been made.
Recommended Reading: How To Deal With Dementia Accusations
Biological Perspective: The Effect And Consequences Of Neuropathological Changes In Dementia On Pain
Both neuropathological and neuroimaging studies have described interconnected brain areas that are important in the mediation of pain processing.,, Most studies describe two neuronal networks, the medial and lateral pain systems. The medial pain system comprising the amygdala, medial thalamus, hippocampus, anterior cortex cinguli, and prefrontal cortex is a pathway that mediates cognitiveevaluative and motivational-affective aspects of pain. In addition, autonomicendocrine aspects are also mediated by the medial system., The lateral pain system comprises, among others, the primary somatosensoric areas and the lateral thalamic nuclei. The sensorydiscriminative aspects are mediated by the lateral pain system. Overlap of the two systems might occur in the insula. Recently, the existence of a third pathway mediating other critical aspects of pain has been proposed. This is thought to be a rostral, or limbic, pain system, which mediates behavioral aspects of pain for example, agitated behavior as a reaction to pain.
Tests For Lewy Body Dementia
There is no specific blood test for LBD. However, blood and urine samples are usually tested to exclude the possibility of other causes of your symptoms.
At the specialist clinic, further assessments and investigations including brain scans are usually carried out.
There are a number of different types of brain scans. Some scans look at how the different parts of the brain fit together, rather than how the parts work together.
A diagnosis cannot be made by just looking at these types of scans other medical information will also be needed.
Recommended Reading: Dementia Awareness Ribbon Color
Treatment Of Behavior And Mood Problems In Lewy Body Dementia
Behavioral and mood problems in people with LBD can arise from hallucinations, delusions, pain, illness, stress, or anxiety. They may also be the result of frustration, fear, or feeling overwhelmed. The person may resist care or lash out verbally or physically.
Medications are appropriate if the behavior interferes with the person’s care or the safety of the person or others. If medication is used, then the lowest possible dose for the shortest period of time is recommended.
The first step is to visit a doctor to see if a medical condition unrelated to LBD is causing the problem. Injuries, fever, urinary tract or pulmonary infections, pressure ulcers , and constipation can worsen behavioral problems and increase confusion.
Certain medications, such as anticholinergics and antihistamines may also cause behavioral problems. For example, some medications for sleep problems, pain, bladder control, and LBD-related movement symptoms can cause confusion, agitation, hallucinations, and delusions. Similarly, some anti-anxiety medicines can actually increase anxiety in people with LBD. Review your medications with your doctor to determine if any changes are needed.
Antidepressants can be used to treat depression and anxiety, which are common in LBD. Many of them are often well tolerated by people with LBD.
Pain Reduced By Mozarts Music
A Salt Lake Tribune article said researchers found that in the surgical pain model, the study found music alone reduced pain 77 percent, compared to no music. Ibuprofen and music reduced pain responses in the inflammation pain model by 93 percent, compared to ibuprofen without music. With CBD, the difference in swelling was 21 percent with music compared to without music.
Music has been known to be calming, and remarkably effective with various aspects of cognition and mood for those with dementia. If similar results are replicated in humans, itll be a wonderful option which could potentially improve mood as well as reduce pain, with less, or no, medication.
Its well worth trying to incorporate music into every day, for everyone, for so many reasons.
Strength to all! Timothy Hudson
Learn more about the research:
Also Check: What Color Ribbon Is Alzheimer’s
Lewy Body Dementia Canada
Learn to live best with LBD
Menu
Pain seems to be more related to autonomic issues than mobility issues in a new Parkinsons Disease pain study. And by extension, it seems likely thatd be the same with Lewy Body Dementia.
Many, if not most, people with Lewy Body Dementia have Parkinsonism mobility issues. Pain, of an often inexplicable source is very common, and has often been believed to be related to lack of mobility from the condition. However, this study concludes that perception of pain is mostly related to central nervous system issues. This implies that for the same pathology two people with the same degree of arthritis can sense pain very differently.
- There was no correlation between musculoskeletal pain and motor symptoms
- There was also no correlation between radicular pain and motor symptoms
- Very weak correlation between lower abdominal pain and constipation scores
Get as much exercise as possible, and as is safe and approved by a specialist. There are few situations when it will be bad, and even if it doesnt fix all the pain issues, it will aid in sleep improvement. It also usually leads to better mood and any method of maintaining as much mobility and flexibility is beneficial.
Behavioral And Mood Symptoms Of Lewy Body Dementia
Changes in behavior and mood are possible in LBD and may worsen as the persons thinking abilities decline. These changes may include:
- Depression
- Apathy, or a lack of interest in normal daily activities or events and less social interaction
- Anxiety and related behaviors, such as asking the same questions over and over or being angry or fearful when a loved one is not present
- Agitation, or restlessness, and related behaviors, such as pacing, hand wringing, an inability to get settled, constant repeating of words or phrases, or irritability
- Delusions, or strongly held false beliefs or opinions not based on evidence. For example, a person may think his or her spouse is having an affair or that relatives long dead are still living.
- Paranoia, or an extreme, irrational distrust of others, such as suspicion that people are taking or hiding things
Recommended Reading: How To Stop Alzheimer’s Patient From Picking Skin
Lbd Tyenol And Opiates
- Constipation, which is likely already an issue for anyone with LBD.
- Sleepiness and additional confusion is common, with an increased the risk of fractures caused by falls.
- Disordered breathing, with slower or shallow breathing patterns, especially during sleep.
- Heart problems. Some opioids increase the risk of heart attack or heart failure. Ask the doctor about this before agreeing to any opiate drugs for your loved one.
Reference:Denham A. Pain Management in Dementia. University of North Carolina School of Medicine. July 10, 2013. https://www.med.unc.edu/pcare/files/pain-management-in-dementia
A Long Road To A Diagnosis Of Lewy Body Dementia
In addition to the initial pain, Maureen developed headaches and issues with her vision. I started getting some weird lights in the side of my eyes, just a bunch of crazy things, she says. Still, Maureen continued to put her children and other responsibilities first. As other symptoms came along, I would try to fit my kids in before me, she says.
Then one day in late 2009 when she was teaching, something felt wrong. She stopped by her doctors office on the way home from school. When they took her blood pressure, they told her, Youre going right to the hospital. Youre off the charts. Her list of symptoms expanded to include high blood pressure that was especially difficult to treat.
The disease also manifested in sleeping problems. At first, Maureens kids told her she was talking in her sleep. Then they told her she was yelling in her sleep. My son came in to try to wake me up one night, and somehow I had the remote control in my hand, and I threw it, Maureen says. I didnt know he was in the room.
Maureens neurologist referred her to a sleep doctor, who diagnosed her with an REM sleep behavior disorder. She had been acting out her dreams. It was then that Maureen heard about Lewy body dementia for the first time. But the doctor assured her Lewy body dementia wasnt the cause. No, no, no, not you, she remembers hearing. The sleep doctor told her she was too young. Instead, they believed she had Parkinsons disease.
You May Like: Parkinsons And Alzheimers Together
What Is Lewy Body Dementia: A Caregivers Guide
Lewy body dementia is one of the most common forms of dementia. However, it is frequently misdiagnosed as more commonly known illnesses, such as Alzheimer’s disease or schizophrenia.
Caring for someone with dementia can be scary, confusing, and overwhelming. If you feel like youre in the dark, youre not alone.
Below, we take a closer look at the symptoms of LBD and unpack what caregivers should know about this complex disease.
Causes Of Dementia With Lewy Bodies
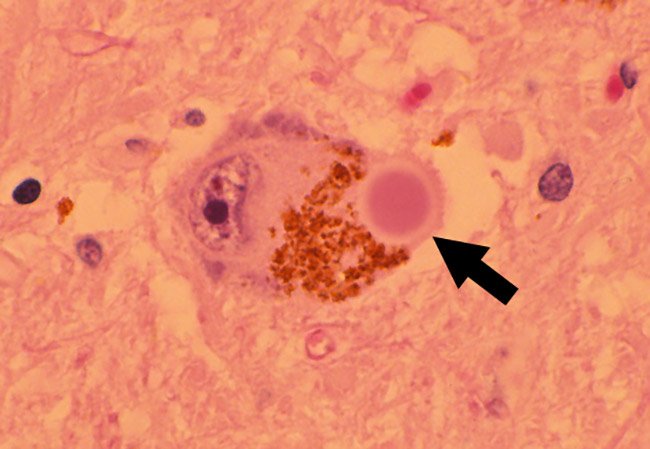
Dementia with Lewy bodies is caused by clumps of protein forming inside brain cells. These abnormal deposits are called Lewy bodies.
These deposits are also found in people with Parkinson’s disease, and they build up in areas of the brain responsible for functions such as thinking, visual perception and muscle movement.
It’s not clear why the deposits develop and how exactly they damage the brain. It’s thought that part of the problem is the proteins affecting the brain’s normal functions by interfering with signals sent between brain cells.
Dementia with Lewy bodies usually occurs in people with no family history of the condition, although there have been very rare cases that seem to run in families.
You May Like: Neil Diamond Alzheimer’s
Lewy Body Dementia Research
Many avenues of research are being explored to improve our understanding of LBD. Some researchers are working to identify the specific differences in the brain between the two types of LBD. Others are looking at the disease’s underlying biology, genetics, and environmental risk factors. Still other scientists are trying to identify biomarkers , improve screening tests to aid diagnosis, and research new treatments.
Scientists hope that new knowledge about LBD will one day lead to more effective treatments and even ways to cure and prevent the disorder. Until then, researchers need volunteers with and without LBD for clinical studies.
NIH and other groups help people learn about clinical trials and studies and find research opportunities near them. Visit the following websites for details: