What Is Dementia Symptoms Types And Diagnosis
Dementia is the loss of cognitive functioning thinking, remembering, and reasoning to such an extent that it interferes with a person’s daily life and activities. Some people with dementia cannot control their emotions, and their personalities may change. Dementia ranges in severity from the mildest stage, when it is just beginning to affect a person’s functioning, to the most severe stage, when the person must depend completely on others for basic activities of living.
Dementia is more common as people grow older but it is not a normal part of aging. Many people live into their 90s and beyond without any signs of dementia.
There are several different forms of dementia, including Alzheimers disease. A persons symptoms can vary depending on the type.
What To Expect With A Head Ct Scan
If you decide to get a head CT scan, the process usually starts with contrast dye. Depending on your situation, this may be ingested orally or intravenously with a needle. This is simply dye that allows the images to show up on the screen.
Then, you get into the CT machine. While there are some standing CT machines, you generally need to use a machine that lets you lie down for a head scan. During the procedure, there is no pain, and in fact, all you have to do is stay still. Note that you may hear some noises, and some people feel anxious due to the confined space. If you anticipate feeling worried during the procedure, you may want to talk with your doctor about anti-anxiety medicine.
Facing the idea that you might have Alzheimers can be incredibly scary, but its important to remember that the earlier you detect the more likely you are to be able to manage the symptoms. To set up an appointment, contact American Health Imaging today.
The Use Of Ct In Dementia
Published online by Cambridge University Press: 10 June 2011
- Department of Neurological and Psychiatric Sciences, University of Florence, Florence, Italy
- Anna Poggesi
- Department of Neurological and Psychiatric Sciences, University of Florence, Florence, Italy
- Leonardo Pantoni*
- Department of Neurological and Psychiatric Sciences, University of Florence, Florence, Italy
- *
- Correspondence should be addressed to: Leonardo Pantoni, MD, PhD, Department of Neurological and Psychiatric Sciences ,
You May Like: What Shampoos Cause Alzheimer’s Disease And Cancer
Signs You May Need A Scan
If you have a family history of Alzheimers or dementia, you may want to get tested proactively so that you can determine if you have this condition. In other situations, you may want to get tested if you have any of the following symptoms:
- Memory loss
- Issues with depth perception
- Delusions or hallucinations
Many people believe that some memory loss is inevitable with aging, but this is simply not true. If you or your loved one is experiencing chronic or progressive memory loss or memory loss combined with the above symptoms, it may be a sign of Alzheimers.
Early Alzheimers Detection With Digital Imaging
Digital imaging of the brain is one of the most promising areas of research being focused on for early detection of Alzheimers disease. Imaging such as an magnetic resonance imaging and positron emission tomography scans are able to show changes in the brains of patients diagnosed with Alzheimers disease. In the past, these tests were used primarily to rule out other conditions that may cause symptoms that were similar to those for Alzheimers.
Experts believe that Alzheimers is a disease that begins many years before symptoms like memory loss and personality changes even become apparent, so a test or scan for early detection is paramount. The current Alzheimers treatments can prevent further deterioration of the brain but not repair the brain. This means that once an Alzheimers diagnosis is reached, the patient has often already experienced years of irreversible brain damage.
Because of this, early detection of Alzheimers is crucial. Researchers who study the brains of Alzheimers patients have found they are different than those of patients with dementia or mild cognitive impairment. Different types of brain imaging help us to find these changes.
Here at Independent Imaging, we offer the areas most advanced diagnostic imaging equipment and technology. Call or request an appointment online with one of our board-certified radiologists in Wellington, Belle Glade, or Lake Worth today.
Also Check: How Do You Spell Alzheimers Disease
Read Also: Terry Semel Alzheimer’s
Additional Tests To Treat And Manage Dementia
Once an individual is diagnosed with dementia, the next step that follows is helping them understand how the condition will affect them and how to manage it.
Several other medical assessments exist to help physicians understand how the condition affects a specific person. And also help families, as well as caregivers, figure out the best course of treatment for the individual.
Did you HEAR of the peanut butter test?
Neuropsychological Testing
Neuropsychologists and psychologists who have specialized training can also prescribe neuropsychological tests to detect dementia.
The process involves WRITTEN and ORAL tests that can take several hours to complete.
They use these methods to assess the cognitive functions of the person suspected to have dementia.
It helps them figure out if certain areas are impaired.
The tests assess aspects like vision-motor, memory, comprehension, reasoning, coordination, and writing abilities.
Physicians may administer additional tests to find out if the person in question is SUFFERING from mood problems or dementia.
Functional Assessments
Dementia is a cognitive disorder that affects the afflicted persons daily functioning in different regards.
Objective assessments can establish what a person is STILL ABLE to do versus what they can no longer do in light of the condition.
Family members are asked to fillquestionnaires that provide details about the persons daily life in terms of the activities they are able to perform.
Psychosocial evaluation
Structural Signs Of Dementia
Structural imaging of the brain consists of computed tomography and the popularly known magnetic resonance imaging scans. This kind of imaging focuses on the morphology as well as the structural details of the brain’s composition. It is a very physical kind of scan, searching for solid, visible signs of degeneration or abnormalities.
Degenerative dementia causes a number of visible physical signs in the brain in some patients, but is not always easy to detect. CT scans can usually observe some atrophy of the brain’s medial temporal lobe, but the CT scans’ lack of sensitivity can occasionally be problematic. MRI scans, of much higher resolution, can capture atrophy of the hippocampus in nearly 90 percent of all cases of Alzheimer’s disease.
Read Also: Dementia Ribbon Colors
Why Doctors Consider Mri To Detect Dementia
Medical experts will advise on the use of MRI when they suspect that a person has dementia.
MRI uses focused radio waves and magnetic fields to detect the presence of hydrogen atoms in tissues in the human body.
MRI scans also reveal the brains anatomic structure with 3D imaging allowing doctors to get a clear view of the current state of the organ.
This way, the doctor is able to rule out other health problems like hydrocephalus, hemorrhage, stroke, and tumors that can mimic dementia.
With these scans, physicians can also detect loss of brain mass that relates to different types of dementia.
fMRI records blood flow changes that are linked to the activities of the brain. This may help physicians differentiate dementia types.
Verywellhealth.com also suggests that MRI scans can at times identify reversible cognitive decline.
In such a case, a doctor will recommend appropriate treatment that will reverse this decline and restore cognitive functioning.
Do I Need A Brain Scan To Diagnose Alzheimers Disease
Question: Do I need a brain scan to diagnose Alzheimers disease?
Answer: Yes, No, Maybe..
Alzheimers disease and dementia are diagnosed by physicians by taking a careful medical history from the patient and a family member, doing a number of brief memory and cognitive tests, and performing a physical exam. Whether your doctor will also order a brain scan might depend on where you live!
In the U.S., it is recommended that everyone being investigated for dementia have a CT scan or MRI . In Canada, we suggest that brain scans are only essential in cases where the history and physical exam suggest that the dementia is caused by something other than Alzheimers disease . Even in Canada, however, if you are seen by a dementia specialist, you will likely have a brain scan ordered, because of the extra information the scans can provide. Besides helping with the diagnosis for rarer forms of dementia, they can also help determine the presence of cerebrovascular disease. Cerebrovascular disease can be a primary cause of dementia, but can also frequently be mixed with other pathology like Alzheimers disease.
Don’t Miss: 7th Stage Of Dementia
Rate Of Change Of Brain Atrophy
Changes in the rate of atrophy progression can be useful in diagnosing Alzheimer disease. Longitudinal changes in brain size are associated with longitudinal progression of cognitive loss, and enlargement of the third and lateral ventricles is greater in patients with Alzheimer disease than in control subjects.
CT scan indices of hippocampal atrophy are highly associated with Alzheimer disease, but the specificity is not well established. Use of a nonquantitative rating scale showed a sensitivity of 81% and a specificity of 67% in differentiating 21 patients with Alzheimer disease with moderate dementia from 21 age-matched control subjects. Hippocampal volumes in a sample of similar size permitted correct classification of 85% of control subjects.
Brain Imaging Can Aid Professionals
In most cases, brain imaging can assist professionals in diagnosing dementia, ruling out other possibilities with similar symptoms and verifying which stage a patient may be experiencing. Using scans to analyze signs of dementia can exclude the possibility of lesions that cause cognitive degeneration or impairment .
It can also help to determine which kind of dementia a patient is experiencing. For instance, vascular dementia may not show evidence of a cortical loss, whereas this qualifier could still allow a patient to have Alzheimer’s disease. Also, by undergoing frequent scans, neurologists can make a determination of how the disease is progressing. If a diagnosis is uncertain, follow-up scans taken after a few years can prove that degeneration is occurring. Finally, brain imaging can assist researchers in determining how each disease can affect a patient, and whether certain treatments are effective.
Also Check: Alzheimer Ribbon Color
The Limitations Of Amyloid Pet In Ad
Major deterrents to the widespread use of amyloid PET remain cost and availability. Availability has been improved by the development of F-18-labeled agents that can be distributed to PET scanners not associated with a cyclotron. Cost remains an issue, especially where CSF measurement of A42 can provide very similar information when the question is simply the presence or absence of brain A deposition. Being an early event in the pathogenesis of AD, amyloid PET is not a good surrogate marker of progression during the clinical stage of the disease . This role is filled much better by structural MRI and FDG PET . Similarly, amyloid imaging gives much more of a binary diagnostic readout than techniques such as MRI and FDG PET. That is, amyloid imaging has a certain specificity for the pathology of AD, but when that pathology is absent, a negative amyloid PET scan will be identical regardless of the non-AD etiology of the dementia. In contrast, MRI and FDG PET may give an indication of a frontotemporal or vascular pathology when an amyloid PET scan would be ambiguously negative in both cases. The threshold of sensitivity of amyloid PET has yet to be precisely determined, but it is clear that some level of amyloid deposition is histologically detectable prior to the in vivo signal becoming positive .
Future Directions In Diagnosis Research
Considerable research effort is being put into the development of better tools for accurate and early diagnosis. Research continues to provide new insights that in the future may promote early detection and improved diagnosis of dementia, including:
- Better dementia assessment tests that are suitable for people from diverse educational, social, linguistic and cultural backgrounds.
- New computerised cognitive assessment tests which can improve the delivery of the test and simplify responses.
- Improved screening tools to allow dementia to be more effectively identified and diagnosed by GPs.
- The development of blood and spinal fluid tests to measure Alzheimers related protein levels and determine the risk of Alzheimers disease.
- The use of sophisticated brain imaging techniques and newly developed dyes to directly view abnormal Alzheimers protein deposits in the brain, yielding specific tests for Alzheimers disease.
You May Like: What Color Ribbon Is Alzheimer’s
Brain Scans: Your Rights
Brain scans are not considered an essential part of a dementia diagnosis, so you arent automatically entitled to receive one on the NHS. Dementia Guidelines by NICE state that brain scans may not always be needed in those presenting with moderate to severe dementia, if the diagnosis is already clear. The guidelines also say that if you want a brain scan your GP must provide detailed clinical information suggesting why it is necessary.
In other words, those who are elderly, frail or already showing obvious signs of dementia you probably wont be offered a brain scan. But those who are young, or have symptoms which could also indicate other brain diseases such as tumours and cancers, should be referred to hospital for a scan, though the waiting times can vary from days to several weeks, depending on where you live.
Other Types Of Biomarkers
Blood Tests
Proteins that originate in the brain, such as tau and beta-amyloid 42, may be measured with sensitive blood tests. Levels of these proteins may change because of Alzheimer’s, a stroke, or other brain disorders. These blood biomarkers are less accurate than CSF biomarkers for identifying Alzheimer’s and related dementias. However, new methods to measure these brain-derived proteins, particularly beta-amyloid 42/beta-amyloid 40 and phospho-tau 181, have improved, suggesting that blood tests may be used in the future for screening and perhaps diagnosis.
Many other proteins, lipids, and other substances can be measured in the blood, but so far none has shown value in diagnosing Alzheimer’s.
Currently, dementia researchers use blood biomarkers to study early detection, prevention, and the effects of potential treatments. They are not used in doctors’ offices and other clinical settings.
Genetic Testing
Genes are structures in a body’s cells that are passed down from a person’s birth parents. They carry information that determines a person’s traits and keep the body’s cells healthy. Problems with genes can cause diseases like Alzheimer’s.
A genetic test is a type of medical test that analyzes DNA from blood or saliva to determine a person’s genetic makeup. A number of genetic combinations may change the risk of developing a disease that causes dementia.
Read more about Alzheimer’s disease genetics.
Biomarkers in Development
Read Also: Ribbon Color For Alzheimer’s
Is It Possible For A Ct Scan To Show A Recent Tia
Wouldnt it be great if a TIA could leave footprints that can be seen on a CT scan?
This way, a doctor can point to the footprints and tell the patient with conviction, Yes, you had a transient ischemic attack, or, You did NOT have a TIA.
The answer to whether a CT scan can detect a recent TIA is Yes and no, says Rob Lapporte, MD, board certified in emergency medicine and chief medical officer of Physician 360, a telemedicine service.
A CT scan is useful in the workup for TIA in two ways, explains Dr. Lapporte.
First if all is if the CT scan shows evidence of an infarct or hemorrhage, then it rules out a TIA.
An infarct refers to a localized area of tissue that has died from lack of blood .
So in scenario #1, the patient is then diagnosed with a stroke. In the second way that a CT scan can help in diagnosing a TIA, the scan does not show evidence of an acute infarct or hemorrhage, continues Dr. Lapporte.
In addition to that, the symptoms of the patient are consistent with a TIA, and the diagnosis of transient ischemic attack is made.
Dr. Lapporte adds, If youre asking if you can see a TIA on a CT scan, the answer is no. Its a clinical diagnosis.
Changes In Brain Structure
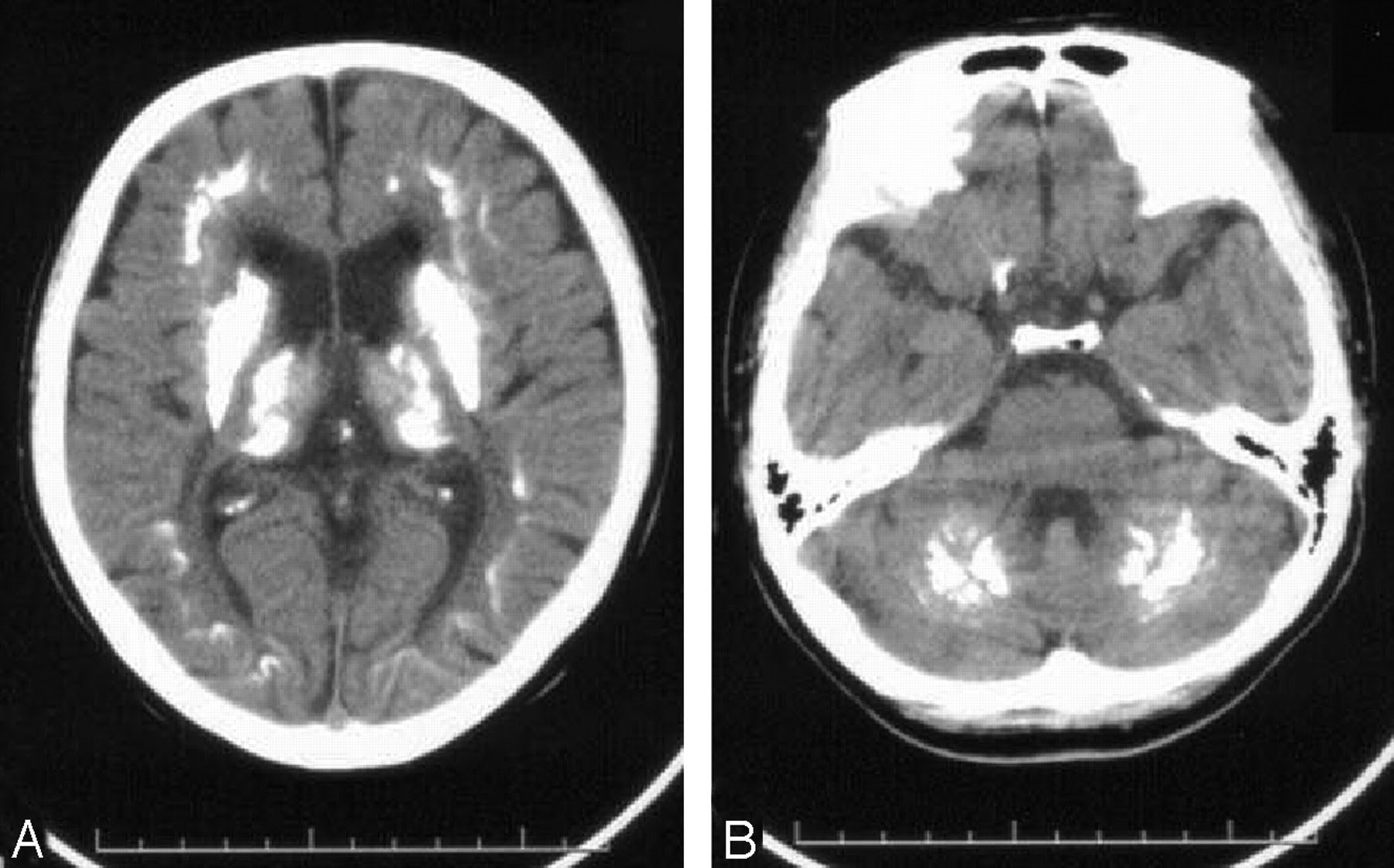
Diffuse cerebral atrophy with widened sulci and dilatation of the lateral ventricles can be observed. Disproportionate atrophy of the medial temporal lobe, particularly of the volume of the hippocampal formations , can be seen.
The hippocampus is one of the earliest affected brain regions in Alzheimer disease, and its dysfunction is believed to underlie the core feature of the disease-memory impairment. Changes in hippocampal volume, shape, symmetry, and activation are reflected by cognitive impairment.
Dilatation of the perihippocampal fissure is a useful radiologic marker for the initial diagnosis of Alzheimer disease, with a predictive accuracy of 91%. The hippocampal fissure is surrounded laterally by the hippocampus, superiorly by the dentate gyrus, and inferiorly by the subiculum. These structures are all involved in the early development of Alzheimer disease and explain the enlargement in the early stages. At the medial aspect, the fissure communicates with the ambient cistern, and its enlargement on CT scans is often seen as hippocampal lucency or hypoattenuation in the temporal area medial to the temporal horn.
The temporal horns of the lateral ventricles may be enlarged. Prominence of the choroid and hippocampal fissures and enlargement of the sylvian fissure may be noted. White matter attenuation is not a feature of Alzheimer disease.
Also Check: Puzzles For Dementia Patients
What Is The Role Of Imaging Studies In The Workup Of Delirium Dementia And Amnesia
A head CT scan without intravenous contrast should be obtained if CNS infection, trauma, or a cerebral vascular accident is suspected. A CT scan is excellent for detecting acute hematomas and most subarachnoid hemorrhages but is most accurate early in the course. Follow-up lumbar puncture may be needed to rule out SAH.
One study found a high prevalence of abnormal CT scan findings in patients with acute mental status changes in the ED. Eight clinical predictors were significantly associated with an abnormal scan, including diastolic blood pressure of more than 80 mm Hg, focal weakness, a Glasgow Coma Score of less than 15, antiplatelet use, upgoing plantar response, headache, anticoagulant use, and dilated pupils.
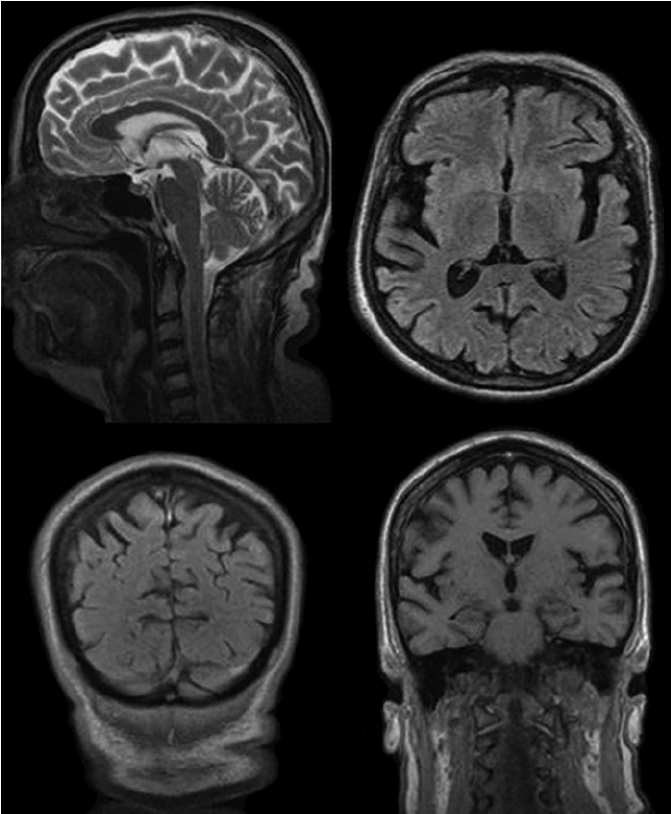
Although not typically part of the workup in the ED, a brain MRI may be considered if readily available and the need confirmed by neurologist and/or radiologist. MRI helps distinguish between Alzheimer disease and vascular causes of dementia. The MRI may show subtle signs of stroke missed on CT and is the imaging modality of choice for multiple sclerosis. An example of MRI in a patient with moderate Alzheimer disease is shown in the image below.
Plain abdominal radiographs may reveal swallowed bags that contain drugs of abuse or radiodense substances such as iron tablets.
References
Han JH, Morandi A, Ely EW, et al. Delirium in the nursing home patients seen in the emergency department. J Am Geriatr Soc. 2009 May. 57:889-94. .