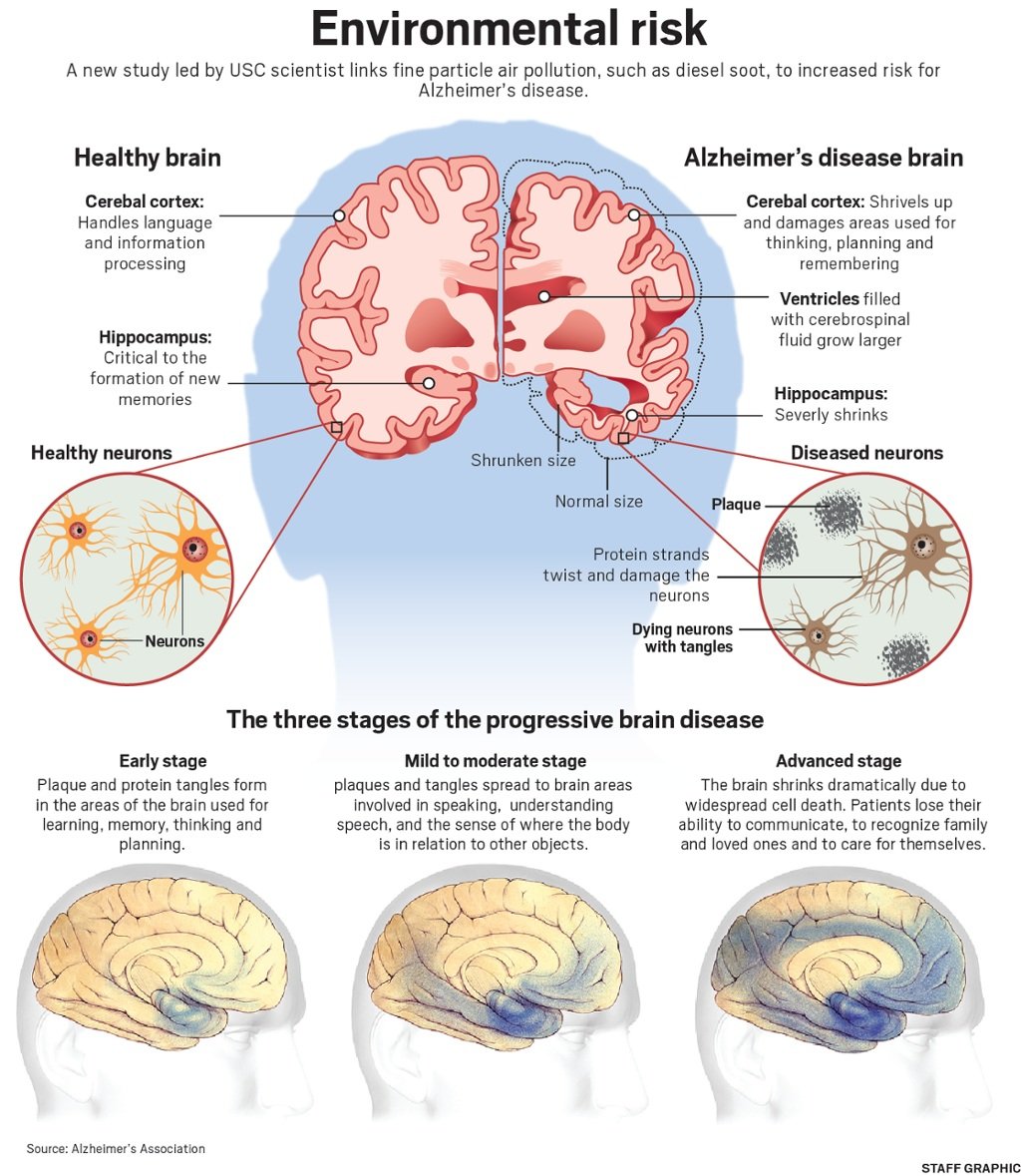
Mystery: What Does Inflammation Have To Do With Alzheimer’s Disease
Another characteristic brain abnormality of Alzheimer’s disease is inflammation meaning the excessive action of the immune cells in the brain.
It’s unclear whether inflammation is a result of having Alzheimer’s disease, or whether the inflammatory process plays a role in its development. It’s also possible that inflammation is both a cause and effect of the disease.
What’s known is that there are immune cells in the brain known as microglia that are normally present to clean up infections, which helps protect the brain, Selkoe said. There is also good evidence that these immune cells get upset about the buildup of too much amyloid in the brain, which makes them aggravated, causing the microglia to release too much protein, he said.
The release of too much protein by microglia can cause trouble at the synapses, or connections, between nerve cells, Selkoe said.Scientists wonder whether drugs aimed at controlling inflammation in the brain could also help control memory problems, he said.
Frontotemporal Dementia Versus Psychiatric Disorders
When behavioral symptoms predominate, people with FTD who become ill in mid-life may be confused with patients who have late life depression. When the onset is in younger persons, the FTD may be confused with schizophrenia or bipolar disorder. Repetitive compulsive behaviors are very common in bvFTD, and some patients may initially be given the diagnosis of obsessive-compulsive disorder. Since the history and exam of a person with a psychiatric disorder and a person with FTD may look very similar, neuropsychological testing and a brain image may help clarify the picture. MRI can help rule out other diseases and support a diagnosis of FTD.
Relationship Between Npss And Alzheimers Disease
Behavioral and neuropsychiatric symptoms are associated with abnormalities in specific brain regions, such as the prefrontal and subcortical limbic regions, which disrupt the normal balance of neurotransmission. According to neuroimmunoregulation theory, this, in turn, is associated with inflammatory pathways that lead to microglial activation and aggregation and the formation of neurofibrillary tangles, ultimately triggering neuronal loss . In addition, NPSs are related to the dysfunction of various neurotransmitter pathways related to AD, including the dopamine system, the serotonin system, and the cholinergic system . In the current section, we will further discuss the molecular and cellular changes associated with stages of AD progression and their relationship to NPSs.
NPSs in preclinical Alzheimers disease
NPSs are variable and sporadic throughout the course of the disease, but an important group appears early ,1), especially emotional symptoms , before the clinical diagnosis of cognitive impairment .
NPSs in mild to severe Alzheimers disease
In the final stage of AD, the pathology of all NPSs becomes complicated and difficult to treat. Worsening mental symptoms cause confusion between reality and morbid fantasies, and patients exhibit severe abnormal motor behaviour, often characterized by scratching, which can lead to recurrent hyperfascial skin infections. These destructive NPSs accelerate the death of AD patients.
Summary
Also Check: How Quickly Does Alzheimer’s Progress
Frontotemporal Dementia Causes And Risk Factors
Scientists donât know for sure what causes FTD. But it starts when nerve cells in two parts, or âlobes,â of the brain â the front and the side â die. That causes the lobes to shrink.
Doctors believe FTD may be genetic. About 4 out of 10 people who have it also have a relative who had it or some other form of dementia.
Genetic FTD happens when you have a mutation, or change, in one of three genes:
- C9ORF72
The type of mutation you have affects the type of symptoms you have.
Delusions And Hallucinations In Ad
Frontotemporal region lesions in AD delusion
Delusions are characterized by asymmetrical brain structure change in the frontal and temporal regions as well as mainly atrophy in the right temporal lobe and left frontal lobe . In addition, delusions are associated with gray matter change in the right hippocampus, left frontal lobe, right frontoparietal cortex, and left claustrum , and white matter changes in the bilateral frontal, parieto-occipital region, left basal ganglia, the body of the corpus callosum and the superior temporal gyrus . The severity of delusions is associated with hypometabolism in the frontal lobe, especially in the right lateral frontal cortex, ACC and OFC , but the association with metabolism in the temporal lobe and occipital lobe is inconsistent. Some studies showed delusions had hypometabolism in the bilateral temporal cortex and the left medial occipital region , while other studies showed delusions had higher metabolism in the superior temporal, left inferior temporal gyrus and inferior parietal lobe or no connection . The discrepancies among previous studies are likely due to sex differences. One study showed that women with delusions had frontotemporal atrophy in AD, but men with delusions did not have brain atrophy compared to men without delusions .
Anterior-posterior neural network lesions in AD hallucination
Summary
Recommended Reading: Ben Carson Dementia
Pathogenesis Of Alzheimers Disease
A number of hypotheses have been proposed that may explain AD pathogenesis: the A-amyloid hypothesis, the A-amyloid oligomer hypothesis, the presenilin hypothesis, the Ca2+ dysregulation hypothesis, the lysosome hypothesis, and the tau hypothesis . Although the amyloid hypothesis is the best-developed hypothesis,, multiple reports have suggested a weak correlation between A deposition and neuronal atrophy and cognitive impairment.,
Pathogenic hypotheses for synaptic and neuronal toxicity in Alzheimers disease.
A is the most widely studied component of AD pathogenesis. The isolation and partial sequencing of the meningovascular A by George Glenner and Caine Wong in 1984 was a turning point for modern research of the fundamental mechanisms of AD. Multiple forms of A are derived by proteolytic cleavage from the type I cell-surface protein amyloid precursor protein . The amyloid hypothesis broadly posits that excessive amounts of A peptide in the brain are responsible for AD-related pathology, including amyloid plaques, neurofibrillary tangles, synapse loss, and eventual neuronal cell death.,,,
Imaging of amyloid plaques reveals the rapid formation of plaque structures over a 24 hour time period dystrophic swelling of adjacent dendrites begins to appear within one week., Instability of spines in the vicinity of A plaques reflects dynamically dysfunctional plasticity in neuronal structures. These processes enhance functional deficit in the regions surrounding plaques.
Can We Predict Molecular Pathologies In Frontotemporal Dementia
Despite recent histopathological and genetic advances,24 accurate prediction of underlying molecular pathologies within the FTD spectrum remains problematic . This has important implications for targeting future disease modifying therapies and, more immediately, for counselling of patients and family members. While phenotypic variation and overlap are substantial, certain clinico-anatomical profiles are consistently associated with particular molecular pathologies .21 These include FTD with motor neurone disease associated with TDP-43 pathology the semantic dementia syndrome and focal, asymmetric temporal lobe atrophy with TDP-43 type C pathology behavioural variant FTD of very young onset and prominent caudate atrophy with FUS pathology and the progressive supranuclear palsy syndrome with a specific tauopathy. Non-fluent speech breakdown and the development of parkinsonism are more commonly associated with tau than non-tau pathologies. The heritability of particular FTD syndromes varies substantially3: semantic dementia is generally sporadic, whereas behavioural variant FTD and corticobasal syndrome are highly genetically as well as pathologically heterogeneous. Useful neuroanatomical associations which may help guide genetic testing include relatively symmetric anteromesial temporal lobe atrophy with MAPT mutations and striking asymmetric hemispheric atrophy with GRN mutations .4
Read Also: Alzheimer’s Aphasia
Spinal Fluid Biomarkers Detect Neurodegeneration Alzheimer’s Disease In Living Patients
by Perelman School of Medicine at the University of Pennsylvania
Alzheimer’s disease and related diseases can still only be confirmed in deceased patients’ brains via autopsy. Even so, the development of biomarkers can give patients and their families answers during life: Alzheimer’s disease can be accurately detected via peptides and proteins in a patient’s cerebrospinal fluids , which can be collected through a lumbar puncture and tested while the patient is alive. In 2018, a new framework suggested combining three Alzheimer’s disease biomarkers in CSFpathologic amyloid plaques , tangles , and neurodegeneration , collectively called ATN. According to recent research from the Perelman School of Medicine at the University of Pennsylvania, the ATN framework can be extended to detect another neurodegenerative condition: frontotemporal degeneration.
Patients with frontotemporal degeneration can experience a range of symptoms, including behavioral changes, executive dysfunction, and language impairments. Distinguishing frontotemporal degeneration from Alzheimer’s disease can be a challenge for clinicians: the symptoms of frontotemporal degeneration can sometimes overlap with Alzheimer’s disease, and a subset of patients can even have both pathologies. Biomarkers can fill the gap by providing evidence of whether Alzheimer’s pathology underlies a patient’s symptoms.
Explore further
Microglial Activation And Aberrant Tnf
Depressive-like behavior has been reported in transgenic models of AD . Here, we first extended those findings using APPSwe/PS1E9 mice, a well characterized AD model . Consistent with findings in transgenic AD models, we reported recently that a single intracerebroventricular infusion of AOs induces depressive-like behavior and cognitive deficit in mice . In an effort to elucidate the mechanisms underlying this effect, we initially investigated whether proteins implicated in depressive-like behavior in mice or in human depressive disorder might mediate the impact of AOs. We examined the expression levels of p11 , BDNF , GATA-1 and indoleamine-2,3-dioxygenase in mouse brains after intracerebroventricular infusion of AOs. No changes in mRNA levels were detected for any of these proteins either 24 h or 10 d after infusion. Interestingly, a robust increase in brain expression of TNF-, a proinflammatory cytokine implicated in depressive behavior and recently found to mediate AO-induced memory impairment in mice , was verified 24 h after infusion of AOs . Increased brain expression of TNF- persisted for 8 d after AO infusion . We further found increased hippocampal levels of TNF- and soluble TNF- receptor 1 5 h after infusion of AOs in mice. Underlining the pathophysiological relevance of elevated TNF- signaling in AD, significantly higher plasma levels of sTNFR1 were verified in AD patients compared with age-matched healthy subjects .
You May Like: Jigsaw Puzzles Alzheimer’s
Molecular Mechanisms Of Neurodegeneration In The Entorhinal Cortex That Underlie Its Selective Vulnerability During The Pathogenesis Of Alzheimer’s Disease
Competing interests
The authors declare no competing or financial interests.
Biol Open
Olayemi Joseph Olajide, Marcus E. Suvanto, Clifton Andrew Chapman Molecular mechanisms of neurodegeneration in the entorhinal cortex that underlie its selective vulnerability during the pathogenesis of Alzheimer’s disease. Biol Open 15 January 2021 10 : bio056796. doi:
What Are The Complications Of Frontotemporal Dementia
FTD is not life-threatening people may live with it for years. But it can lead to an increased risk for other illnesses that can be more serious. Pneumonia is the most common cause of death, with FTD. People are also at increased risk for infections and fall-related injuries.
As FTD progressively worsens, people may engage in dangerous behaviors or be unable to care for themselves. They may need 24-hour nursing care or to stay in an assisted living facility or nursing home.
You May Like: Reading With Dementia
Recommended Reading: Shampoos That Cause Alzheimer’s
Framing Heterogeneity And Complexity In The Ad Syndrome
AD phenotype is strongly affected by age of onset, genetic profile, and comorbidities. AD subtypes reflect the interactions between these three axes. When the onset is later, ApoE 4 is present, and comorbidities absent, the resulting pattern is generally prototypic AD. Changes along any of these three axes shift the observed phenotype towards one of the rarer AD variants .
Figure 7
Proposed framework for Alzheimer’s disease subtypes. Bubbles represent subpopulations of Alzheimer’s disease by subtype, located along each of the three axes of heterogeneity: age of onset, apolipoprotein E status, and co-pathology. Exact size, positioning and degree of overlap for each subtype remain uncertain areas of active research.
Warning Signs Of Alzheimer’s
Memory often changes as people grow older. Some people notice changes in themselves before anyone else does. For other people, friends and family are the first to see changes in memory, behavior, or abilities. Memory loss that disrupts daily life is not a typical part of aging. People with one or more of these 10 warning signs should see a doctor to find the cause. Early diagnosis gives them a chance to seek treatment and plan for the future.
1. Memory loss that disrupts daily life: forgetting events, repeating yourself or relying on more aids to help you remember .
2.Challenges in planning or solving problems: having trouble paying bills or cooking recipes you have used for years.
3.Difficulty completing familiar tasks at home, at work, or at leisure: having problems with cooking, driving places, using a cell phone, or shopping.
4.Confusion with time or place: having trouble understanding an event that is happening later, or losing track of dates.
5.Trouble understanding visual images and spatial relations: having more difficulty with balance or judging distance, tripping over things at home, or spilling or dropping things more often.
The Centers for Disease Control and Prevention and the Alzheimers Association have created the Healthy Brain Initiatives State and Local Public Health Partnerships to Address Dementia: The 2018-2023 Road Map.
8. being a victim of a scam, not managing money well, paying less attention to hygiene, or having trouble taking care of a pet.
You May Like: Alzheimer Ribbon Color
Animal Models And Behavior
Memory and learning are dependent upon alterations in synaptic transmission within the hippocampus and other areas of the brain. Transgenic animals that over-express A accurately model familial-type AD and may contribute to increased understanding of the pathogenesis of cognitive and memory deficits., Synaptic function and plasticity have been extensively studied in transgenic APP and APP/PS mice, with a focus on the dentate gyrus and CA1 subfields of the hippocampus. AD transgenic mice show abnormal synaptic transmission and impaired LTP, often well in advance of plaque formation., Memory and learning deficits may occur within 3 months in mouse models, suggesting that soluble A contributes to AD pathogenesis., Alternate studies report later onset of symptoms at more advanced ages, implicating insoluble A plaques., The specific structure of A that is responsible for cognitive deficits has been the subject of great debate. Amygdala-dependent learning is strongly inhibited with increasing age in Tg2576 mice models, suggesting that the amygdala is susceptible to A toxcicity.,,
Mystery: What Is The Relationship Between The Plaques And The Tangles Found In The Brain
Since 1906 when the disease was first described by Alois Alzheimer, researchers have known about the presence of plaques and tangles in the brains of people with Alzheimer’s. But one of the big mysteries of the disease is how these two hallmarks of the disease might be related, Selkoe said.
Scientists have unraveled part of the answer to this mystery by discovering that the plaques develop in the brain first, before the tangles, Selkoe told Live Science. It’s also known that the buildup of amyloid beta protein causes injury to nerve cells, and that strands of tau protein twist and form tangles inside nerve cells, he said.
But researchers don’t yet know exactly how these plaques and tangles affect brain function, eventually leading to the memory problems, behavioral changes and other symptoms of Alzheimer’s disease. Selkoe said. And they also don’t know whether amyloid in plaque and tau in tangles work separately, or together, to damage nerve cells, he added.
These are some reasons why therapies aimed solely at reducing amyloid buildup might not be enough by itself to treat Alzheimer’s disease, and why there may also be a need for a drug that helps lower tau levels, Selkoe said.
Read Also: Aphasia And Alzheimer’s
How Do You Diagnose Frontal Lobe Dementia
Signs Of Frontotemporal Dementia
A group of disorders caused by cell degeneration, frontotemporal dementia affects the brain, specifically its areas associated with personality, behavior and language. Once considered a rare disease, FTD may account for 20-50% of dementia cases in people younger than age 65, according to the Alzheimers Association.
FTD causes cell damage that shrinks the brains frontal and temporal lobes. The disease generally starts with personality and behavior changes and may eventually lead to severe memory loss.
Often miscategorized as psychiatric illness, frontotemporal dementia typically strikes between the ages of 45 and 65. However, the Association for Frontotemporal Dementia Degeneration indicates that cases have occurred as early as age 21 and as late as age 80.
Cognitive Reserve And Prevention
The quantitative function known as brain reserve has wide ranging biological implications for the pathogenesis of AD. For example, environmental stimuli trigger upregulation of BDNF and neurogenesis, encouraging neural plasticity., Cognitive and brain reserves, enhance our understanding of the differences in the clinical pathology of the brains of AD patients., A number of studies have evaluated the association between leisure activities and AD incidence. Engagement in intellectual activities or social activities was assessed in a large cohort of elderly New Yorkers who had not been diagnosed with AD individuals engaged in numerous leisure activities had a dramatically reduced risk of developing AD during follow-up evaluation.,
Recommended Reading: Purple Ribbon Alzheimer’s
Treatments For Frontotemporal Dementia
Thereâs currently no cure for frontotemporal dementia or any treatment that will slow it down.
But there are treatments that can help control some of the symptoms, possibly for several years.
Treatments include:
- medicines to control some of the behavioural problems
- therapies such as physiotherapy, occupational therapy, and speech and language therapy for problems with movement, everyday tasks and communication
- dementia activities such as memory cafes, which are drop-in sessions for people with memory problems and their carers to get support and advice
- support groups who can offer tips on managing symptoms from dementia experts and people living with frontotemporal dementia, and their families
Also Check: What Color Ribbon Is Alzheimerâs
Association With Rates Of Decline
Agitation, alone and in combination with other BPSD, has been associated with disease severity over time, but inconsistently with disease progression. There are few studies that assess agitation as an isolated factor. Haupt and Kurz , in a small clinic-based study, found that aggression was one factor that predicted institutionalization over 1 year. Similarly, Peters et al. in the Cache County Dementia Progression Study, found that agitation/aggression was a significant predictor of the risks of both of severe dementia and death in a Cox proportional hazards model, although the baseline status of participants in that cohort is unclear. Further, Lopez et al. in their study of the effects of psychiatric symptoms and psychiatric medications on disease progression found that the presence of either aggression or agitation was independently associated with a significantly increased risk of shorter time to significant functional impairment while controlling for age, education, sex, and baseline cognitive and functional status.
Of note, Hallikainen et al. found that, along with agitation and aggression, aberrant motor behavior tended to track with disease severity and was a predictor of disease progression . Aberrant motor behaviors are sometimes, but not always, clustered together with agitation in studies that have looked for grouping of neuropsychiatric symptoms out of the neuropsychiatric inventory by methods such as factor analysis and latent class analysis.
Read Also: Can Prevagen Help Dementia